Favorable Local Control From Consolidative Radiation Therapy in High-Risk Neuroblastoma Despite Gross Residual Disease, Positive Margins, or Nodal Involvement
- PMID: 28244417
- PMCID: PMC5502807
- DOI: 10.1016/j.ijrobp.2016.11.043
Favorable Local Control From Consolidative Radiation Therapy in High-Risk Neuroblastoma Despite Gross Residual Disease, Positive Margins, or Nodal Involvement
Abstract
Purpose: To report the influence of radiation therapy (RT) dose and surgical pathology variables on disease control and overall survival (OS) in patients treated for high-risk neuroblastoma at a single institution.
Methods and materials: We conducted a retrospective study of 67 high-risk neuroblastoma patients who received RT as part of definitive management from January 2003 until May 2014.
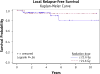
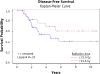
Results: At a median follow-up of 4.5 years, 26 patients (38.8%) failed distantly; 4 of these patients also failed locally. One patient progressed locally without distant failure. Local control was 92.5%, and total disease control was 59.5%. No benefit was demonstrated for RT doses over 21.6 Gy with respect to local relapse-free survival (P=.55), disease-free survival (P=.22), or OS (P=.72). With respect to local relapse-free survival, disease-free survival, and OS, no disadvantage was seen for positive lymph nodes on surgical pathology, positive surgical margins, or gross residual disease. Of the patients with gross residual disease, 75% (6 of 8) went on to have no evidence of disease at time of last follow-up, and the 2 patients who failed did so distantly.
Conclusions: Patients with high-risk neuroblastoma in this series maintained excellent local control, with no benefit demonstrated for radiation doses over 21.6 Gy, and no disadvantage demonstrated for gross residual disease after surgery, positive surgical margins, or pathologic lymph node positivity. Though the limitations of a retrospective review for an uncommon disease must be kept in mind, with small numbers in some of the subgroups, it seems that dose escalation should be considered only in exceptional circumstances.
Copyright © 2016 Elsevier Inc. All rights reserved.
Conflict of interest statement
Conflict of interest: none.
Figures
Similar articles
-
Dose-escalation is needed for gross disease in high-risk neuroblastoma.Pediatr Blood Cancer. 2018 Jul;65(7):e27009. doi: 10.1002/pbc.27009. Epub 2018 Feb 22. Pediatr Blood Cancer. 2018. PMID: 29469198 Free PMC article. Clinical Trial.
-
Excellent local control from radiation therapy for high-risk neuroblastoma.Int J Radiat Oncol Biol Phys. 2009 Aug 1;74(5):1549-54. doi: 10.1016/j.ijrobp.2008.10.069. Epub 2009 Feb 11. Int J Radiat Oncol Biol Phys. 2009. PMID: 19211198
-
Hyperfractionated low-dose radiotherapy for high-risk neuroblastoma after intensive chemotherapy and surgery.J Clin Oncol. 2001 Jun 1;19(11):2821-8. doi: 10.1200/JCO.2001.19.11.2821. J Clin Oncol. 2001. PMID: 11387353 Clinical Trial.
-
259 Patients with DCIS of the breast applying USC/Van Nuys prognostic index: a retrospective review with long term follow up.Breast Cancer Res Treat. 2008 Jun;109(3):405-16. doi: 10.1007/s10549-007-9668-7. Epub 2007 Aug 9. Breast Cancer Res Treat. 2008. PMID: 17687650 Review.
-
Role and toxicity of radiation therapy in neuroblastoma patients: A literature review.Crit Rev Oncol Hematol. 2020 May;149:102924. doi: 10.1016/j.critrevonc.2020.102924. Epub 2020 Mar 3. Crit Rev Oncol Hematol. 2020. PMID: 32172225 Review.
Cited by
-
Analysis of the risk factor for the poor prognosis of localized neuroblastoma after the surgical.Medicine (Baltimore). 2018 Oct;97(40):e12718. doi: 10.1097/MD.0000000000012718. Medicine (Baltimore). 2018. PMID: 30290678 Free PMC article.
-
Musculoskeletal outcomes and the effect of radiation to the vertebral bodies on growth trajectories for long-term survivors of high-risk neuroblastoma.J Radiat Oncol. 2018 Jun;7(2):187-193. doi: 10.1007/s13566-018-0349-4. Epub 2018 Mar 29. J Radiat Oncol. 2018. PMID: 34178250 Free PMC article.
-
MYCN Impact on High-Risk Neuroblastoma: From Diagnosis and Prognosis to Targeted Treatment.Cancers (Basel). 2022 Sep 12;14(18):4421. doi: 10.3390/cancers14184421. Cancers (Basel). 2022. PMID: 36139583 Free PMC article. Review.
-
Patterns of recurrence after radiation therapy for high-risk neuroblastoma.Radiat Oncol J. 2019 Sep;37(3):224-231. doi: 10.3857/roj.2019.00353. Epub 2019 Sep 30. Radiat Oncol J. 2019. PMID: 31591871 Free PMC article.
-
Pediatric minimally invasive surgery for malignant abdominal tumor: Single center experience.Medicine (Baltimore). 2019 Aug;98(33):e16776. doi: 10.1097/MD.0000000000016776. Medicine (Baltimore). 2019. PMID: 31415380 Free PMC article.
References
-
- Haas-Kogan DA, Swift PS, Selch M, et al. Impact of radiotherapy for high-risk neuroblastoma: A Children’s Cancer Group study. Int J Radiat Oncol Biol Phys. 2003;56:28–39. - PubMed
-
- Rosen EM, Cassady JR, Frantz CN, et al. Improved survival in neuroblastoma using multimodality therapy. Radiother Oncol. 1984;2:189–200. - PubMed
-
- Rosen EM, Cassady JR, Frantz CN, et al. Neuroblastoma: The Joint Center for Radiation Therapy/Dana-Farber Cancer Institute/Children’s Hospital experience. J Clin Oncol. 1984;2:719–732. - PubMed
-
- Gatcombe HG, Marcus RB, Jr, Katzenstein HM, et al. Excellent local control from radiation therapy for high-risk neuroblastoma. Int J Radiat Oncol Biol Phys. 2009;74:1549–1554. - PubMed
-
- Browne M, Kletzel M, Cohn SL, et al. Excellent local tumor control regardless of extent of surgical resection after treatment on the Chicago Pilot II protocol for neuroblastoma. J Pediatr Surg. 2006;41:271–276. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical