Clinical outcomes of gastrointestinal brain metastases treated with radiotherapy
- PMID: 28245881
- PMCID: PMC5331623
- DOI: 10.1186/s13014-017-0774-3
Clinical outcomes of gastrointestinal brain metastases treated with radiotherapy
Abstract
Background: Brain metastases of gastrointestinal origin are a rare occurrence. Radiation therapy (RT) in the form of stereotactic radiosurgery (SRS) or whole brain radiation therapy (WBRT) is an effective established treatment modality in either the definitive or adjuvant setting. The aim of this study is to assess the long-term clinical outcomes of patients with gastrointestinal (GI) brain metastases treated with SRS or WBRT.
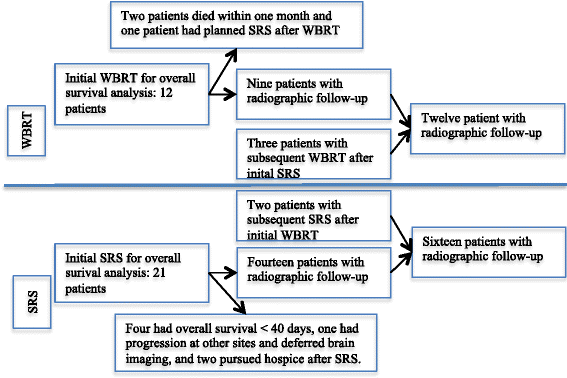
Methods: In this single institutional retrospective review, we detail the outcomes of patients diagnosed with metastatic brain tumors from an adenocarcinoma gastrointestinal primary. Patients were treated using stereotactic radiosurgery or whole brain radiation therapy. Initial site control (defined as lesions visualized on imaging at time of treatment), new site control (defined as new intracranial lesions visualized on follow-up imaging), and overall survival were calculated using the Kaplan-Meier method.
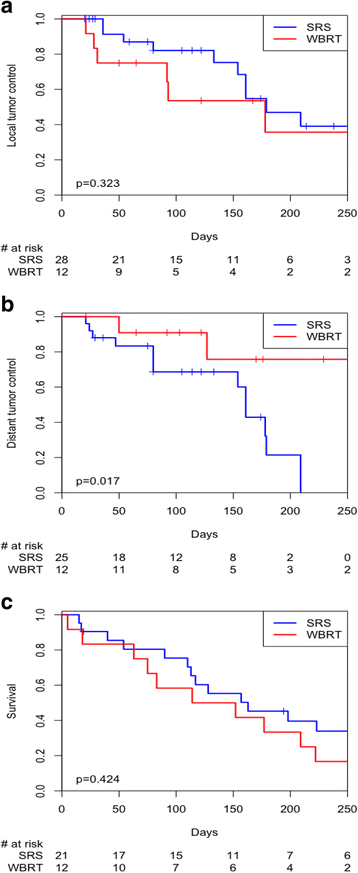
Results: Thirty-three patients were treated from August 2008 to December 2015. Primary malignancy locations were as follows: 18 colon, 6 esophagus, 4 rectum, 5 other. Median total dose delivered was 25 Gy (18-35 Gy) in a median of 4 fractions for SRS and 30 Gy (10.8-40 Gy) in 10 fractions for WBRT. Crude initial site control at last radiographic follow-up was 64.3% after SRS and 41.7% after WBRT. Eleven of the 28 brain lesions (39.3%) treated with SRS had resection of the SRS-treated lesion prior to radiation therapy. Five of the twelve patients (41.7%) undergoing WBRT underwent cranial resection prior to radiation therapy. Crude new site control at last radiographic follow-up was 46.4% after SRS and 83.3% after WBRT. Kaplan-Meier analysis of overall survival did not show any statistically significant difference between WBRT and SRS (p = 0.424). Median overall survival for SRS patients was 5.2 months (0.5-57.5) and for WBRT patients 4.4 months (0-15). Kaplan-Meier analysis of new site control was significantly improved with WBRT versus SRS (p = 0.017). Total dose, treatment with WBRT, and active extracranial disease were statistically significant on multivariate analysis for new site control (p < 0.05).
Conclusions: Survival and intracranial disease control are poor following RT for brain metastases from GI primaries. In this small series, outcomes are worse than published series for other primary malignancies metastatic to the brain and further research into methods of local control improvement is warranted. Future studies should explore the utility of dose escalation or radiosensitization in this patient population.
Keywords: Brain neoplasm; Gastrointestinal neoplasms; Metastases; Radiosurgery.
Figures
Similar articles
-
Cost-effectiveness of stereotactic radiosurgery with and without whole-brain radiotherapy for the treatment of newly diagnosed brain metastases.J Neurosurg. 2014 Dec;121 Suppl:84-90. doi: 10.3171/2014.7.GKS14972. J Neurosurg. 2014. PMID: 25434941
-
Potential role for LINAC-based stereotactic radiosurgery for the treatment of 5 or more radioresistant melanoma brain metastases.J Neurosurg. 2015 Nov;123(5):1261-7. doi: 10.3171/2014.12.JNS141919. Epub 2015 Jul 3. J Neurosurg. 2015. PMID: 26140482
-
Early Gamma Knife stereotactic radiosurgery to the tumor bed of resected brain metastasis for improved local control.J Neurosurg. 2014 Dec;121 Suppl:69-74. doi: 10.3171/2014.7.GKS141488. J Neurosurg. 2014. PMID: 25434939
-
Clinical outcomes of stereotactic radiosurgery in the treatment of patients with metastatic brain tumors.World Neurosurg. 2011 May-Jun;75(5-6):673-83. doi: 10.1016/j.wneu.2010.12.006. World Neurosurg. 2011. PMID: 21704935 Review.
-
Congress of Neurological Surgeons Systematic Review and Evidence-Based Guidelines on the Role of Whole Brain Radiation Therapy in Adults With Newly Diagnosed Metastatic Brain Tumors.Neurosurgery. 2019 Mar 1;84(3):E159-E162. doi: 10.1093/neuros/nyy541. Neurosurgery. 2019. PMID: 30629211
Cited by
-
Treatment of brain metastases from gastrointestinal primaries: Comparing whole-brain radiotherapy and stereotactic radiosurgery in terms of survival.North Clin Istanb. 2021 Feb 11;9(1):47-56. doi: 10.14744/nci.2021.65725. eCollection 2022. North Clin Istanb. 2021. PMID: 35340309 Free PMC article.
-
Stereotactic Radiosurgery Results for Patients With Brain Metastases From Gastrointestinal Cancer: A Retrospective Cohort Study of 802 Patients With GI-GPA Validity Test.Adv Radiat Oncol. 2021 May 18;6(6):100721. doi: 10.1016/j.adro.2021.100721. eCollection 2021 Nov-Dec. Adv Radiat Oncol. 2021. PMID: 34934852 Free PMC article.
-
Brain metastasis in colorectal cancer presenting as refractory hypertension.J Community Hosp Intern Med Perspect. 2018 Aug 23;8(4):215-219. doi: 10.1080/20009666.2018.1490138. eCollection 2018. J Community Hosp Intern Med Perspect. 2018. PMID: 30181829 Free PMC article.
-
Stereotactic radiosurgery for the treatment of brain metastasis from gastrointestinal primary cancers.J Radiosurg SBRT. 2019;6(1):27-34. J Radiosurg SBRT. 2019. PMID: 30775072 Free PMC article.
-
Multi-institutional Outcomes after Stereotactic Radiosurgery for Gastrointestinal Brain Metastases.Adv Radiat Oncol. 2025 May 10;10(7):101795. doi: 10.1016/j.adro.2025.101795. eCollection 2025 Jul. Adv Radiat Oncol. 2025. PMID: 40538502 Free PMC article.
References
-
- Surveillance, Epidemiology, and End Results (SEER) Program (http://www.seer.cancer.gov) Research Data (1973–2013). National Cancer Institute, DCCPS, Surveillance Research Program, Surveillance Systems Branch. Accessed 19 July 2016.
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical