Newly divided eosinophils limit ozone-induced airway hyperreactivity in nonsensitized guinea pigs
- PMID: 28258108
- PMCID: PMC5495948
- DOI: 10.1152/ajplung.00530.2016
Newly divided eosinophils limit ozone-induced airway hyperreactivity in nonsensitized guinea pigs
Abstract
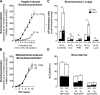
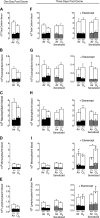
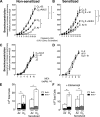
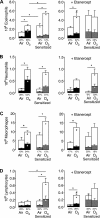
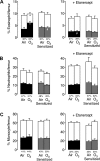
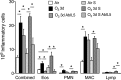
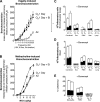
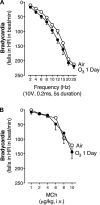
Ozone causes vagally mediated airway hyperreactivity and recruits inflammatory cells, including eosinophils, to lungs, where they mediate ozone-induced hyperreactivity 1 day after exposure but are paradoxically protective 3 days later. We aimed to test the role of newly divided eosinophils in ozone-induced airway hyperreactivity in sensitized and nonsensitized guinea pigs. Nonsensitized and sensitized guinea pigs were treated with 5-bromo-2-deoxyuridine (BrdU) to label newly divided cells and were exposed to air or ozone for 4 h. Later (1 or 3 days later), vagally induced bronchoconstriction was measured, and inflammatory cells were harvested from bone marrow, blood, and bronchoalveolar lavage. Ozone induced eosinophil hematopoiesis. One day after ozone, mature eosinophils dominate the inflammatory response and potentiate vagally induced bronchoconstriction. However, by 3 days, newly divided eosinophils have reached the lungs, where they inhibit ozone-induced airway hyperreactivity because depleting them with antibody to IL-5 or a TNF-α antagonist worsened vagally induced bronchoconstriction. In sensitized guinea pigs, both ozone-induced eosinophil hematopoiesis and subsequent recruitment of newly divided eosinophils to lungs 3 days later failed to occur. Thus mature eosinophils dominated the ozone-induced inflammatory response in sensitized guinea pigs. Depleting these mature eosinophils prevented ozone-induced airway hyperreactivity in sensitized animals. Ozone induces eosinophil hematopoiesis and recruitment to lungs, where 3 days later, newly divided eosinophils attenuate vagally mediated hyperreactivity. Ozone-induced hematopoiesis of beneficial eosinophils is blocked by a TNF-α antagonist or by prior sensitization. In these animals, mature eosinophils are associated with hyperreactivity. Thus interventions targeting eosinophils, although beneficial in atopic individuals, may delay resolution of airway hyperreactivity in nonatopic individuals.
Keywords: 5-bromo-2-deoxyuridine; airway hyperreactivity; eosinophil hematopoiesis; ozone; sensitization.
Copyright © 2017 the American Physiological Society.
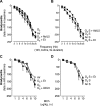
Figures
Similar articles
-
Protective Role of Eosinophils and TNFa after Ozone Inhalation.Res Rep Health Eff Inst. 2017 Mar;2017(191):1-41. Res Rep Health Eff Inst. 2017. PMID: 29659241 Free PMC article.
-
IL-1 receptors mediate persistent, but not acute, airway hyperreactivity to ozone in guinea pigs.Am J Respir Cell Mol Biol. 2008 Dec;39(6):730-8. doi: 10.1165/rcmb.2008-0045OC. Epub 2008 Jul 10. Am J Respir Cell Mol Biol. 2008. PMID: 18617681 Free PMC article.
-
Antigen sensitization influences organophosphorus pesticide-induced airway hyperreactivity.Environ Health Perspect. 2008 Mar;116(3):381-8. doi: 10.1289/ehp.10694. Environ Health Perspect. 2008. PMID: 18335107 Free PMC article.
-
The influence of sensitization on mechanisms of organophosphorus pesticide-induced airway hyperreactivity.Am J Respir Cell Mol Biol. 2015 Nov;53(5):738-47. doi: 10.1165/rcmb.2014-0444OC. Am J Respir Cell Mol Biol. 2015. PMID: 25897622 Free PMC article.
-
The changing role of eosinophils in long-term hyperreactivity following a single ozone exposure.Am J Physiol Lung Cell Mol Physiol. 2005 Oct;289(4):L627-35. doi: 10.1152/ajplung.00377.2004. Epub 2005 May 27. Am J Physiol Lung Cell Mol Physiol. 2005. PMID: 15923207
Cited by
-
Ozone-induced eosinophil recruitment to airways is altered by antigen sensitization and tumor necrosis factor-α blockade.Physiol Rep. 2017 Dec;5(24):e13538. doi: 10.14814/phy2.13538. Physiol Rep. 2017. PMID: 29242307 Free PMC article.
-
Eosinophil and airway nerve interactions in asthma.J Leukoc Biol. 2018 Jul;104(1):61-67. doi: 10.1002/JLB.3MR1117-426R. Epub 2018 Apr 6. J Leukoc Biol. 2018. PMID: 29633324 Free PMC article. Review.
-
Inflammatory mechanisms linking maternal and childhood asthma.J Leukoc Biol. 2020 Jul;108(1):113-121. doi: 10.1002/JLB.3MR1219-338R. Epub 2020 Feb 10. J Leukoc Biol. 2020. PMID: 32040236 Free PMC article. Review.
-
Parasympathetic Airway Hyperreactivity Is Enhanced in Acute but Not Chronic Eosinophilic Asthma Mouse Models.Am J Respir Cell Mol Biol. 2025 Jun;72(6):698-707. doi: 10.1165/rcmb.2024-0360OC. Am J Respir Cell Mol Biol. 2025. PMID: 39626221
-
The innate immune brakes of the lung.Front Immunol. 2023 Jan 27;14:1111298. doi: 10.3389/fimmu.2023.1111298. eCollection 2023. Front Immunol. 2023. PMID: 36776895 Free PMC article. Review.
References
-
- Alexis NE, Lay JC, Haczku A, Gong H, Linn W, Hazucha MJ, Harris B, Tal-Singer R, Peden DB. Fluticasone propionate protects against ozone-induced airway inflammation and modified immune cell activation markers in healthy volunteers. Environ Health Perspect 116: 799–805, 2008. doi:10.1289/ehp.10981. - DOI - PMC - PubMed
-
- American Lung Association. State of the Air 2016. http://www.lung.org/local-content/california/our-initiatives/state-of-th.... Chicago, IL: ALA, 2016. Date accessed: 1 March 2017.
-
- Arjomandi M, Wong H, Donde A, Frelinger J, Dalton S, Ching W, Power K, Balmes JR. Exposure to medium and high ambient levels of ozone causes adverse systemic inflammatory and cardiac autonomic effects. Am J Physiol Heart Circ Physiol 308: H1499–H1509, 2015. doi:10.1152/ajpheart.00849.2014. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

