Ultrasonographic prevalence and characteristics of non-palpable thyroid incidentalomas in a hospital-based population in a sub-Saharan country
- PMID: 28259145
- PMCID: PMC5336663
- DOI: 10.1186/s12880-017-0194-8
Ultrasonographic prevalence and characteristics of non-palpable thyroid incidentalomas in a hospital-based population in a sub-Saharan country
Abstract
Background: Thyroid incidentalomas (TI) are highly prevalent asymptomatic thyroid nodules with ultrasound as the best imaging modality for their detection and characterization. Although they are mostly benign, potential for malignancy is up to 10-15%. In sub-Saharan Africa little data exists on the prevalence and risk categorization of TI. The aim of this study was to determine the prevalence and ultrasound characteristics of non-palpable thyroid incidentalomas among adults in sub-Saharan setting.
Methods: A cross sectional study was carried out between March and August 2015, at two university teaching hospitals. Sampling was consecutive and included all adults aged ≥ 16 years, presenting for any ultrasound other than for the thyroid, with no history or clinical signs of thyroid disease, and no palpable thyroid lesion. Ultrasound was done using 4 to 11 MHz linear probes. Subjects with diffuse thyroid abnormalities were excluded. Variables studied were age, gender, thyroid volume, ultrasound characteristics of thyroid nodules, TIRADS scores. Differences were considered statistically significant for p-value < 0.05.
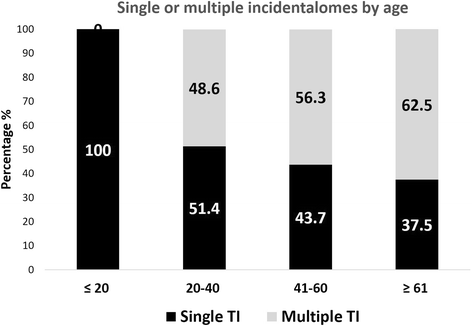
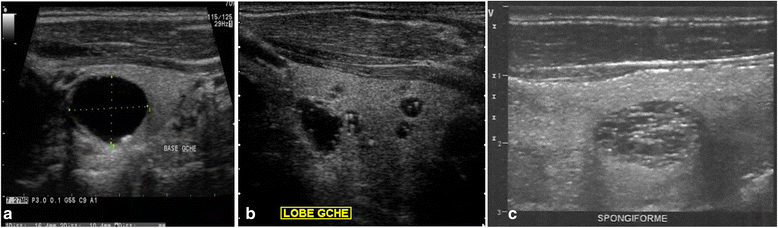
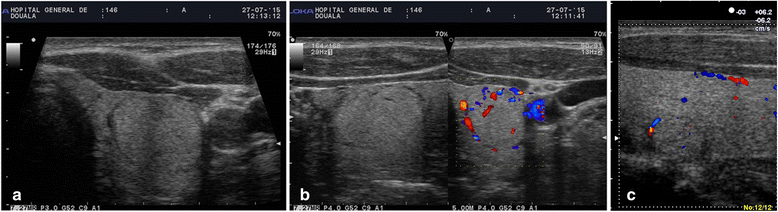
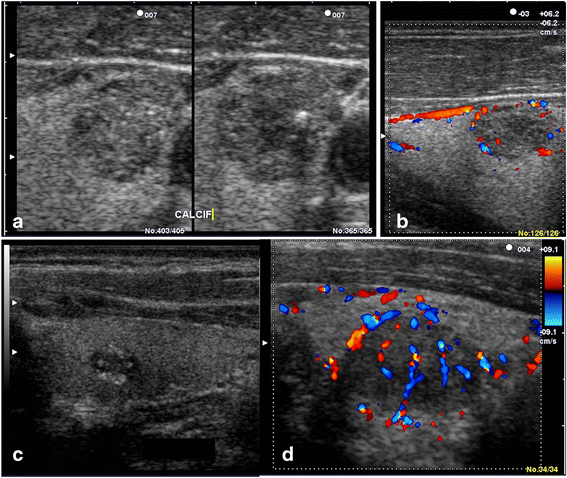
Results: The prevalence of TI was 28.3% (126 persons with TI /446 examined). This prevalence was 46.2% in population ≥ 61-year-old; 6.3% in population ≤ 20-year-old; 33.3% for females and 18.4% for males (p < 0.001). Of the 241 TI found, 49.4% were cysts, 33.6% solid, 17.0% mixed; 37.8% <5 mm and 22% >10 mm. Solid TI were mainly hyperechoic (42.0%), 3/81 were markedly hypoechoic. Sixty-nine out of 126 persons with TI (54.8%) had at least two nodules. Solitary nodules were predominant in the age group ≤20 years. Of 241 TI, 129 (53.5%) were classified TIRADS 2, 81 (33.6%) TIRADS 3, 25 (10.4%) TIRADS 4A, 6 (2.5%) TIRADS 4B, and none TIRADS 5. Characteristics associated with increased risk of malignancy where mostly founded on solid nodules (p < 0.000) and nodules larger than 15 mm (p < 0.001).
Conclusion: Thyroid incidentalomas were very frequent with a prevalence of 28.3% and potential risk of malignancy in 12.9%. Prevalence had a tendency to increase with age and in female. Cystic nodules were the most prevalent. Potential for malignancy would be increased for larger and solid nodules.
Keywords: Prevalence; Sub-Saharan country; TIRADS; Thyroid incidentaloma; Thyroid nodule.
Figures
References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

