Impact of comorbid conditions in COPD patients on health care resource utilization and costs in a predominantly Medicare population
- PMID: 28260880
- PMCID: PMC5327909
- DOI: 10.2147/COPD.S112256
Impact of comorbid conditions in COPD patients on health care resource utilization and costs in a predominantly Medicare population
Abstract
Background: Patients with chronic obstructive pulmonary disease (COPD) often have multiple underlying comorbidities, which may lead to increased health care resource utilization (HCRU) and costs.
Objective: To describe the comorbidity profiles of COPD patients and examine the associations between the presence of comorbidities and HCRU or health care costs.
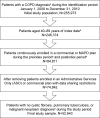
Methods: A retrospective cohort study utilizing data from a large US national health plan with a predominantly Medicare population was conducted. COPD patients aged 40-89 years and continuously enrolled for 12 months prior to and 24 months after the first COPD diagnosis during the period of January 01, 2009, through December 31, 2010, were selected. Eleven comorbidities of interest were identified 12 months prior through 12 months after COPD diagnosis. All-cause and COPD-related hospitalizations and costs were assessed 24 months after diagnosis, and the associations with comorbidities were determined using multivariate statistical models.
Results: Ninety-two percent of 52,643 COPD patients identified had at least one of the 11 comorbidities. Congestive heart failure (CHF), coronary artery disease, and cerebrovascular disease (CVA) had the strongest associations with all-cause hospitalizations (mean ratio: 1.56, 1.32, and 1.30, respectively; P<0.0001); other comorbidities examined had moderate associations. CHF, anxiety, and sleep apnea had the strongest associations with COPD-related hospitalizations (mean ratio: 2.01, 1.32, and 1.21, respectively; P<0.0001); other comorbidities examined (except chronic kidney disease [CKD], obesity, and osteoarthritis) had moderate associations. All comorbidities assessed (except obesity and CKD) were associated with higher all-cause costs (mean ratio range: 1.07-1.54, P<0.0001). CHF, sleep apnea, anxiety, and osteoporosis were associated with higher COPD-related costs (mean ratio range: 1.08-1.67, P<0.0001), while CVA, CKD, obesity, osteoarthritis, and type 2 diabetes were associated with lower COPD-related costs.
Conclusion: This study confirms that specific comorbidities among COPD patients add significant burden with higher HCRU and costs compared to patients without these comorbidities. Payers may use this information to develop tailored therapeutic interventions for improved management of patients with specific comorbidities.
Keywords: COPD; Medicare; comorbidities; cost; database; utilization.
Conflict of interest statement
Disclosure This study was funded by Humana Inc. and Boehringer Ingelheim Pharmaceuticals Inc. Andrew Renda is an employee and shareholder of Humana Inc.; Amol D Dhamane, Kate Burslem, and Shuchita Kaila are employees of Boehringer Ingelheim Pharmaceuticals Inc.; Phil Schwab, Sari D Hopson, Chad Moretz, and Srinivas Annavarapu are employees of Comprehensive Health Insights, Inc., a wholly-owned subsidiary of Humana Inc., who were paid consultants to Boehringer Ingelheim Pharmaceuticals Inc. in connection with the analysis described in this study and with manuscript development. The authors report no other conflicts of interest in this work.
Figures
Similar articles
-
Impact of roflumilast on exacerbations of COPD, health care utilization, and costs in a predominantly elderly Medicare Advantage population.Int J Chron Obstruct Pulmon Dis. 2015 Mar 16;10:565-76. doi: 10.2147/COPD.S79025. eCollection 2015. Int J Chron Obstruct Pulmon Dis. 2015. PMID: 25834417 Free PMC article.
-
COPD exacerbation frequency and its association with health care resource utilization and costs.Int J Chron Obstruct Pulmon Dis. 2015 Dec 3;10:2609-18. doi: 10.2147/COPD.S90148. eCollection 2015. Int J Chron Obstruct Pulmon Dis. 2015. PMID: 26664109 Free PMC article.
-
Impact of exacerbations on health care cost and resource utilization in chronic obstructive pulmonary disease patients with chronic bronchitis from a predominantly Medicare population.Int J Chron Obstruct Pulmon Dis. 2012;7:757-64. doi: 10.2147/COPD.S36997. Epub 2012 Nov 1. Int J Chron Obstruct Pulmon Dis. 2012. PMID: 23152680 Free PMC article.
-
Economic Burden of Chronic Obstructive Pulmonary Disease (COPD): A Systematic Literature Review.Int J Chron Obstruct Pulmon Dis. 2020 Feb 26;15:439-460. doi: 10.2147/COPD.S234942. eCollection 2020. Int J Chron Obstruct Pulmon Dis. 2020. PMID: 32161455 Free PMC article.
-
Impact of PAP therapy on hospitalization rates in Medicare beneficiaries with COPD and coexisting OSA.Sleep Breath. 2019 Mar;23(1):193-200. doi: 10.1007/s11325-018-1680-0. Epub 2018 Jun 22. Sleep Breath. 2019. PMID: 29931497 Free PMC article.
Cited by
-
Insights about the economic impact of chronic obstructive pulmonary disease readmissions post implementation of the hospital readmission reduction program.Curr Opin Pulm Med. 2018 Mar;24(2):138-146. doi: 10.1097/MCP.0000000000000454. Curr Opin Pulm Med. 2018. PMID: 29210750 Free PMC article. Review.
-
Effectiveness of Nationwide COPD Pay-for-Performance Program on COPD Exacerbations in Taiwan.Int J Chron Obstruct Pulmon Dis. 2021 Oct 18;16:2869-2881. doi: 10.2147/COPD.S329454. eCollection 2021. Int J Chron Obstruct Pulmon Dis. 2021. PMID: 34703221 Free PMC article.
-
The contribution of symptoms and comorbidities to the economic impact of COPD: an analysis of the German COSYCONET cohort.Int J Chron Obstruct Pulmon Dis. 2017 Dec 4;12:3437-3448. doi: 10.2147/COPD.S141852. eCollection 2017. Int J Chron Obstruct Pulmon Dis. 2017. PMID: 29270005 Free PMC article.
-
The Economic Burden of Comorbid Obstructive Sleep Apnea Among Patients with Chronic Obstructive Pulmonary Disease.J Manag Care Spec Pharm. 2020 Oct;26(10):1353-1362. doi: 10.18553/jmcp.2020.26.10.1353. J Manag Care Spec Pharm. 2020. PMID: 32996389 Free PMC article.
-
Impact of Positive Airway Pressure Therapy Adherence on Outcomes in Patients with Obstructive Sleep Apnea and Chronic Obstructive Pulmonary Disease.Am J Respir Crit Care Med. 2022 Jul 15;206(2):197-205. doi: 10.1164/rccm.202109-2035OC. Am J Respir Crit Care Med. 2022. PMID: 35436176 Free PMC article.
References
-
- Miniño A, Xu J, Kochanek K. Deaths: preliminary data for 2008. Natl Vital Stat Rep. 2010;59(2):1–52. - PubMed
-
- Ford ES, Murphy LB, Khavjou O, Giles WH, Holt JB, Croft JB. Total and state-specific medical and absenteeism costs of COPD among adults aged ≥18 years in the United States for 2010 and projections through 2020. Chest. 2015;147(1):31–45. - PubMed
-
- Andersson F, Borg S, Jansson SA, et al. The costs of exacerbations in chronic obstructive pulmonary disease (COPD) Respir Med. 2002;96(9):700–708. - PubMed
-
- Global Initiative for Chronic Obstructive Lung Disease global Strategy for Diagnosis, Management and Prevention of COPD. 2015. [Accessed October 27, 2015]. Available from: http://www.goldcopd.org/uploads/users/files/GOLD_Report_2015_Feb18.pdf.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

