Molecular Mechanisms of Bipolar Disorder: Progress Made and Future Challenges
- PMID: 28261061
- PMCID: PMC5306135
- DOI: 10.3389/fncel.2017.00030
Molecular Mechanisms of Bipolar Disorder: Progress Made and Future Challenges
Abstract
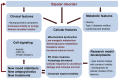
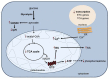
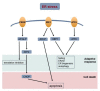
Bipolar disorder (BD) is a chronic and progressive psychiatric illness characterized by mood oscillations, with episodes of mania and depression. The impact of BD on patients can be devastating, with up to 15% of patients committing suicide. This disorder is associated with psychiatric and medical comorbidities and patients with a high risk of drug abuse, metabolic and endocrine disorders and vascular disease. Current knowledge of the pathophysiology and molecular mechanisms causing BD is still modest. With no clear biological markers available, early diagnosis is a great challenge to clinicians without previous knowledge of the longitudinal progress of illness. Moreover, despite recommendations from evidence-based guidelines, polypharmacy is still common in clinical treatment of BD, reflecting the gap between research and clinical practice. A major challenge in BD is the development of effective drugs with low toxicity for the patients. In this review article, we focus on the progress made and future challenges we face in determining the pathophysiology and molecular pathways involved in BD, such as circadian and metabolic perturbations, mitochondrial and endoplasmic reticulum (ER) dysfunction, autophagy and glutamatergic neurotransmission; which may lead to the development of new drugs.
Keywords: bipolar disorder; disease modeling; endoplasmic reticulum stress; glutamate; hyperexcitability; mitochondrial dysfunction; oxidative stress.
Figures
Similar articles
-
Interventions for interpersonal communication about end of life care between health practitioners and affected people.Cochrane Database Syst Rev. 2022 Jul 8;7(7):CD013116. doi: 10.1002/14651858.CD013116.pub2. Cochrane Database Syst Rev. 2022. PMID: 35802350 Free PMC article.
-
Cyclophosphamide for connective tissue disease-associated interstitial lung disease.Cochrane Database Syst Rev. 2018 Jan 3;1(1):CD010908. doi: 10.1002/14651858.CD010908.pub2. Cochrane Database Syst Rev. 2018. PMID: 29297205 Free PMC article.
-
Ketamine and other glutamate receptor modulators for depression in adults with bipolar disorder.Cochrane Database Syst Rev. 2021 Oct 8;10(10):CD011611. doi: 10.1002/14651858.CD011611.pub3. Cochrane Database Syst Rev. 2021. PMID: 34623633 Free PMC article.
-
Antidepressants for the treatment of depression in people with cancer.Cochrane Database Syst Rev. 2018 Apr 23;4(4):CD011006. doi: 10.1002/14651858.CD011006.pub3. Cochrane Database Syst Rev. 2018. Update in: Cochrane Database Syst Rev. 2023 Mar 31;3:CD011006. doi: 10.1002/14651858.CD011006.pub4. PMID: 29683474 Free PMC article. Updated.
-
Pharmacological interventions for people with borderline personality disorder.Cochrane Database Syst Rev. 2022 Nov 14;11(11):CD012956. doi: 10.1002/14651858.CD012956.pub2. Cochrane Database Syst Rev. 2022. PMID: 36375174 Free PMC article.
Cited by
-
Mitochondrial Alterations in Fibroblasts of Early Stage Bipolar Disorder Patients.Biomedicines. 2021 May 7;9(5):522. doi: 10.3390/biomedicines9050522. Biomedicines. 2021. PMID: 34066918 Free PMC article.
-
Endoplasmic reticulum stress differentially inhibits endoplasmic reticulum and inner nuclear membrane protein quality control degradation pathways.J Biol Chem. 2019 Dec 20;294(51):19814-19830. doi: 10.1074/jbc.RA119.010295. Epub 2019 Nov 13. J Biol Chem. 2019. PMID: 31723032 Free PMC article.
-
Reductions in regional theta power and fronto-parietal theta-gamma phase-amplitude coupling during gaze processing in bipolar disorder.Psychiatry Res Neuroimaging. 2023 Jun;331:111629. doi: 10.1016/j.pscychresns.2023.111629. Epub 2023 Mar 18. Psychiatry Res Neuroimaging. 2023. PMID: 36966619 Free PMC article.
-
Translational evidence for lithium-induced brain plasticity and neuroprotection in the treatment of neuropsychiatric disorders.Transl Psychiatry. 2021 Jul 5;11(1):366. doi: 10.1038/s41398-021-01492-7. Transl Psychiatry. 2021. PMID: 34226487 Free PMC article. Review.
-
Pharmaco-psychiatry and gut microbiome: a systematic review of effects of psychotropic drugs for bipolar disorder.Microbiology (Reading). 2025 Jun;171(6):001568. doi: 10.1099/mic.0.001568. Microbiology (Reading). 2025. PMID: 40528728 Free PMC article. Review.
References
-
- Altschule M. D., Henneman D. H., Holliday P., Goncz R. M. (1956). Carbohydrate metabolism in brain disease. VI. Lactate metabolism after infusion of sodium d-lactate in manic-depressive and schizophrenic psychoses. AMA. Arch. Intern. Med. 98, 35–38. 10.1001/archinte.1956.00250250041006 - DOI - PubMed
-
- American Psychiatric Association (2013). Diagnostic and Statistical Manual of Mental Disorders DSM-5. 5th Edn. Arlington, VA: American Psychiatric Association
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

