A hypoperfusion context may aid to interpret hyperlactatemia in sepsis-3 septic shock patients: a proof-of-concept study
- PMID: 28281216
- PMCID: PMC5344869
- DOI: 10.1186/s13613-017-0253-x
A hypoperfusion context may aid to interpret hyperlactatemia in sepsis-3 septic shock patients: a proof-of-concept study
Abstract
Background: Persistent hyperlactatemia is particularly difficult to interpret in septic shock. Besides hypoperfusion, adrenergic-driven lactate production and impaired lactate clearance are important contributors. However, clinical recognition of different sources of hyperlactatemia is unfortunately not a common practice and patients are treated with the same strategy despite the risk of over-resuscitation in some. Indeed, pursuing additional resuscitation in non-hypoperfusion-related cases might lead to the toxicity of fluid overload and vasoactive drugs. We hypothesized that two different clinical patterns can be recognized in septic shock patients through a multimodal perfusion monitoring. Hyperlactatemic patients with a hypoperfusion context probably represent a more severe acute circulatory dysfunction, and the absence of a hypoperfusion context is eventually associated with a good outcome. We performed a retrospective analysis of a database of septic shock patients with persistent hyperlactatemia after initial resuscitation.
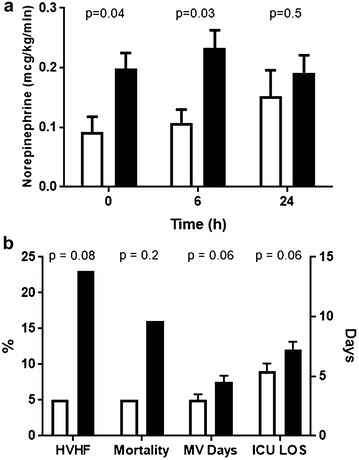
Results: We defined hypoperfusion context by the presence of a ScvO2 < 70%, or a P(cv-a)CO2 ≥6 mmHg, or a CRT ≥4 s together with hyperlactatemia. Ninety patients were included, of whom seventy exhibited a hypoperfusion-related pattern and 20 did not. Although lactate values were comparable at baseline (4.8 ± 2.8 vs. 4.7 ± 3.7 mmol/L), patients with a hypoperfusion context exhibited a more severe circulatory dysfunction with higher vasopressor requirements, and a trend to longer mechanical ventilation days, ICU stay, and more rescue therapies. Only one of the 20 hyperlactatemic patients without a hypoperfusion context died (5%) compared to 11 of the 70 with hypoperfusion-related hyperlactatemia (16%).
Conclusions: Two different clinical patterns among hyperlactatemic septic shock patients may be identified according to hypoperfusion context. Patients with hyperlactatemia plus low ScvO2, or high P(cv-a)CO2, or high CRT values exhibited a more severe circulatory dysfunction. This provides a starting point to launch further prospective studies to confirm if this approach can lead to a more selective resuscitation strategy.
Keywords: Capillary refill time; Central venous oxygen saturation; Central venous-arterial PCO2 gradient; Hyperlactatemia; Hypoperfusion; Resuscitation; Septic shock.
Figures

References
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

