Identification, genetic testing, and management of hereditary melanoma
- PMID: 28283772
- PMCID: PMC5385190
- DOI: 10.1007/s10555-017-9661-5
Identification, genetic testing, and management of hereditary melanoma
Abstract
Several distinct melanoma syndromes have been defined, and genetic tests are available for the associated causative genes. Guidelines for melanoma genetic testing have been published as an informal "rule of twos and threes," but these guidelines apply to CDKN2A testing and are not intended for the more recently described non-CDKN2A melanoma syndromes. In order to develop an approach for the full spectrum of hereditary melanoma patients, we have separated melanoma syndromes into two types: "melanoma dominant" and "melanoma subordinate." Syndromes in which melanoma is a predominant cancer type are considered melanoma dominant, although other cancers, such as mesothelioma or pancreatic cancers, may also be observed. These syndromes are associated with defects in CDKN2A, CDK4, BAP1, MITF, and POT1. Melanoma-subordinate syndromes have an increased but lower risk of melanoma than that of other cancer(s) seen in the syndrome, such as breast and ovarian cancer or Cowden syndrome. Many of these melanoma-subordinate syndromes are associated with well-established predisposition genes (e.g., BRCA1/2, PTEN). It is likely that these predisposition genes are responsible for the increased susceptibility to melanoma as well but with lower penetrance than that observed for the dominant cancer(s) in those syndromes. In this review, we describe our extension of the "rule of twos and threes" for melanoma genetic testing. This algorithm incorporates an understanding of the spectrum of cancers and genes seen in association with melanoma to create a more comprehensive and tailored approach to genetic testing.
Keywords: Gene panel sequencing; Genetic syndromes; Genetic testing; Inherited cancer risk; Melanoma.
Figures

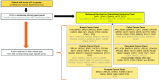
References
-
- Taber JM, Aspinwall LG, Stump TK, Kohlmann W, Champine M, Leachman SA. Genetic test reporting enhances understanding of risk information and acceptance of prevention recommendations compared to family history-based counseling alone. Journal of Behavioral Medicine. 2015;38(5):740–753. doi: 10.1007/s10865-015-9648-z. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

