Pituitary Carcinoma in a Patient with an SDHB Mutation
- PMID: 28284009
- PMCID: PMC5694522
- DOI: 10.1007/s12022-017-9474-7
Pituitary Carcinoma in a Patient with an SDHB Mutation
Abstract
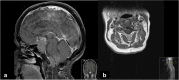
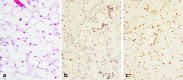
We present the first case of pituitary carcinoma occurring in a patient with a succinate dehydrogenase subunit B (SDHB) mutation and history of paraganglioma. She was initially treated for a glomus tumour with external beam radiotherapy. Twenty-five years later, she was diagnosed with a non-functioning pituitary adenoma, having developed bitemporal hemianopia. Recurrence of the pituitary lesion (Ki-67 10% and p53 overexpressed) occurred 5 years after her transsphenoidal surgery, for which she underwent two further operations followed by radiotherapy. Histology showed large cells with vacuolated clear cytoplasm with positive immunostaining for steroidogenic factor 1 (SF1) and negative staining for pituitary hormones. Four years after the pituitary radiotherapy, two metastatic deposits were identified: a foramen magnum lesion and an intradural extra-medullary cervical lesion at the level of C3/C4. There was also significant growth of the primary pituitary lesion with associated visual deterioration. A biopsy of the foramen magnum lesion, demonstrating cells with vacuolated, clear cytoplasm and positive SF1 staining confirmed a pituitary carcinoma, for which she was commenced on temozolomide chemotherapy. There was dramatic clinical improvement after three cycles and reduction in the size of the lesions was observed following six cycles of temozolomide, and further shrinkage after 10 cycles. The plan is for a total of 12 cycles of temozolomide chemotherapy. SDH mutation-related pituitary tumours have an aggressive phenotype which, in this case, led to metastatic disease. SF1 immunostaining was helpful to identify the tissue origin of the metastatic deposit and to confirm the pituitary carcinoma.
Keywords: Paraganglioma; Pituitary carcinoma; SDHB; Succinate dehydrogenase; Temozolomide.
Conflict of interest statement
Ethics Approval and Consent to Participate
Study is approved by the local Ethics Committee.
Consent for Publication
We have informed consent from the patient.
Competing Interests
The authors declare that they have no conflict of interest.
Funding
N.T. is supported by The Medical College of Saint Bartholomew’s Hospital Trust. We are grateful for the support from the NIHR (National Institute of Health Research, UK). This work was supported by an MRC project grant to MK. We are grateful to the British Neuropathological Society for supporting this study.
Figures

Similar articles
-
An aggressive cabergoline-resistant, temozolomide-responsive macroprolactinoma due to a germline SDHB pathogenic variant in the absence of paraganglioma or pheochromocytoma.Front Endocrinol (Lausanne). 2023 Dec 13;14:1273093. doi: 10.3389/fendo.2023.1273093. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 38152133 Free PMC article.
-
Non-pheochromocytoma (PCC)/paraganglioma (PGL) tumors in patients with succinate dehydrogenase-related PCC-PGL syndromes: a clinicopathological and molecular analysis.Eur J Endocrinol. 2013 Nov 22;170(1):1-12. doi: 10.1530/EJE-13-0623. Print 2014 Jan. Eur J Endocrinol. 2013. PMID: 24096523
-
Malignant paraganglioma and somatotropinoma in a patient with germline SDHB mutation-genetic and clinical features.Endocrine. 2019 Jan;63(1):182-187. doi: 10.1007/s12020-018-1726-x. Epub 2018 Aug 28. Endocrine. 2019. PMID: 30155846
-
Succinate dehydrogenase and MYC-associated factor X mutations in pituitary neuroendocrine tumours.Endocr Relat Cancer. 2022 Sep 2;29(10):R157-R172. doi: 10.1530/ERC-22-0157. Print 2022 Oct 1. Endocr Relat Cancer. 2022. PMID: 35938916 Free PMC article. Review.
-
Temozolomide Is a Potential Therapeutic Tool for Patients With Metastatic Pheochromocytoma/Paraganglioma-Case Report and Review of the Literature.Front Endocrinol (Lausanne). 2020 Feb 18;11:61. doi: 10.3389/fendo.2020.00061. eCollection 2020. Front Endocrinol (Lausanne). 2020. PMID: 32132978 Free PMC article. Review.
Cited by
-
SDHx mutation and pituitary adenoma: can in vivo 1H-MR spectroscopy unravel the link?Endocr Relat Cancer. 2023 Jan 5;30(2):e220198. doi: 10.1530/ERC-22-0198. Print 2023 Feb 1. Endocr Relat Cancer. 2023. PMID: 36449569 Free PMC article.
-
An aggressive cabergoline-resistant, temozolomide-responsive macroprolactinoma due to a germline SDHB pathogenic variant in the absence of paraganglioma or pheochromocytoma.Front Endocrinol (Lausanne). 2023 Dec 13;14:1273093. doi: 10.3389/fendo.2023.1273093. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 38152133 Free PMC article.
-
Clinical features of pituitary carcinoma: analysis based on a case report and literature review.Front Endocrinol (Lausanne). 2024 Oct 31;15:1440247. doi: 10.3389/fendo.2024.1440247. eCollection 2024. Front Endocrinol (Lausanne). 2024. PMID: 39544231 Free PMC article. Review.
-
The 2022 WHO classification of tumors of the pituitary gland: An update on aggressive and metastatic pituitary neuroendocrine tumors.Brain Pathol. 2025 Jan;35(1):e13302. doi: 10.1111/bpa.13302. Epub 2024 Sep 1. Brain Pathol. 2025. PMID: 39218431 Free PMC article. Review.
-
A Comprehensive Target Panel Allows to Extend the Genetic Spectrum of Neuroendocrine Tumors.Neuroendocrinology. 2025;115(5):381-401. doi: 10.1159/000542223. Epub 2024 Nov 13. Neuroendocrinology. 2025. PMID: 39536727 Free PMC article.
References
-
- Xekouki P, Pacak K, Almeida M, Wassif CA, Rustin P, Nesterova M, et al. Succinate dehydrogenase (SDH) D subunit (SDHD) inactivation in a growth-hormone-producing pituitary tumor: a new association for SDH? J Clin Endocrinol Metab. 2012;97(3):E357–E366. doi: 10.1210/jc.2011-1179. - DOI - PMC - PubMed
-
- Papathomas TG, Gaal J, Corssmit EP, Oudijk L, Korpershoek E, Heimdal K, et al. Non-pheochromocytoma (PCC)/paraganglioma (PGL) tumors in patients with succinate dehydrogenase-related PCC-PGL syndromes: a clinicopathological and molecular analysis. Eur J Endocrinol. 2014;170(1):1–12. doi: 10.1530/EJE-13-0623. - DOI - PubMed
-
- Denes J, Swords F, Rattenberry E, Stals K, Owens M, Cranston T, et al. Heterogeneous genetic background of the association of pheochromocytoma/paraganglioma and pituitary adenoma: results from a large patient cohort. J Clin Endocrinol Metab. 2015;100(3):E531–E541. doi: 10.1210/jc.2014-3399. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

