Use of dabigatran and rivaroxaban in non-valvular atrial fibrillation: one-year follow-up experience in an Italian centre
- PMID: 28287377
- PMCID: PMC5839619
- DOI: 10.2450/2017.0196-16
Use of dabigatran and rivaroxaban in non-valvular atrial fibrillation: one-year follow-up experience in an Italian centre
Abstract
Background: Direct oral anticoagulants (DOAC) have been shown to be non-inferior to traditional vitamin K antagonists in preventing stroke and arterial thromboembolism in patients with non-valvular atrial fibrillation. Nevertheless, it is mandatory to record side effects and individual adherence to DOAC treatment.
Materials and methods: In this single-centre experience, patients with non-valvular atrial fibrillation were prospectively observed after switching from a vitamin K antagonist to dabigatran or rivaroxaban. The efficacy, safety, and tolerability of the novel treatment, and adherence to it, were evaluated over a period of 1 year. Clinical data were integrated with records of haemorrhagic and non-haemorrhagic complications. All the subjects were given an anonymous self-report questionnaire on the degree of their adherence/satisfaction with the treatment.
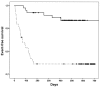
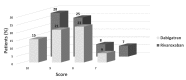
Results: Of 196 patients with non-valvular atrial fibrillation (median age, 78.5 years) who switched from a vitamin K antagonist to DOAC, 178 completed the 1-year follow up, of whom 87 were given dabigatran and 91 rivaroxaban. The efficacy of the two DOAC was similar. Patients given dabigatran had a higher frequency (n=32) of non-haemorrhagic complications (OR: 3.3; 95% CI: 1.7-7.8), which occurred earlier (HR: 6.1; 95% CI: 3.0-12.6) than those (n=7) recorded in subjects on rivaroxaban. The degree of satisfaction with therapy was higher among patients on rivaroxaban (mean score 9.1, SD 1.0) than among those on dabigatran (mean score 8.7; SD 0.9; p=0.01).
Discussion: Overall, in this experience, DOAC were shown to be effective, safe alternatives to vitamin K antagonists. Nevertheless, compared with rivaroxaban, dabigatran resulted in a higher rate and earlier occurrence of non-haemorrhagic events, and a lower satisfaction score.
Conflict of interest statement
The Authors declare no conflicts of interest.
Figures

Comment in
-
Dabigratan-related acute agranulocytosis.Blood Transfus. 2019 Mar;17(2):163-164. doi: 10.2450/2019.0237-18. Epub 2019 Jan 21. Blood Transfus. 2019. PMID: 31013250 Free PMC article. No abstract available.
Similar articles
-
Comparison of Treatment Persistence with Dabigatran or Rivaroxaban versus Vitamin K Antagonist Oral Anticoagulants in Atrial Fibrillation Patients: A Competing Risk Analysis in the French National Health Care Databases.Pharmacotherapy. 2018 Jan;38(1):6-18. doi: 10.1002/phar.2046. Epub 2017 Dec 11. Pharmacotherapy. 2018. PMID: 29028119
-
Effectiveness and safety of reduced dose non-vitamin K antagonist oral anticoagulants and warfarin in patients with atrial fibrillation: propensity weighted nationwide cohort study.BMJ. 2017 Feb 10;356:j510. doi: 10.1136/bmj.j510. BMJ. 2017. PMID: 28188243 Free PMC article.
-
Adherence and outcomes to direct oral anticoagulants among patients with atrial fibrillation: findings from the veterans health administration.BMC Cardiovasc Disord. 2017 Sep 2;17(1):236. doi: 10.1186/s12872-017-0671-6. BMC Cardiovasc Disord. 2017. PMID: 28865440 Free PMC article.
-
The safety and efficacy of non-vitamin K antagonist oral anticoagulants in atrial fibrillation in the elderly.Int J Cardiol. 2018 Aug 15;265:118-124. doi: 10.1016/j.ijcard.2018.02.066. Int J Cardiol. 2018. PMID: 29885678 Review.
-
Medication adherence to rivaroxaban and dabigatran in patients with non-valvular atrial fibrillation: a meta-analysis.J Thromb Thrombolysis. 2020 Apr;49(3):360-364. doi: 10.1007/s11239-019-01986-8. J Thromb Thrombolysis. 2020. PMID: 31691066
Cited by
-
High number of newly initiated direct oral anticoagulant users switch to alternate anticoagulant therapy.J Thromb Thrombolysis. 2017 Nov;44(4):435-441. doi: 10.1007/s11239-017-1565-2. J Thromb Thrombolysis. 2017. PMID: 29027097
-
Comparison of clinical effects and costs among dabigatran etexilate, rivaroxaban and warfarin in elderly patients with atrial fibrillation.Am J Transl Res. 2023 May 15;15(5):3639-3646. eCollection 2023. Am J Transl Res. 2023. PMID: 37303642 Free PMC article.
-
Role of rivaroxaban in the management of atrial fibrillation: insights from clinical practice.Vasc Health Risk Manag. 2018 Jan 9;14:13-21. doi: 10.2147/VHRM.S134394. eCollection 2018. Vasc Health Risk Manag. 2018. PMID: 29391805 Free PMC article. Review.
-
Dabigratan-related acute agranulocytosis.Blood Transfus. 2019 Mar;17(2):163-164. doi: 10.2450/2019.0237-18. Epub 2019 Jan 21. Blood Transfus. 2019. PMID: 31013250 Free PMC article. No abstract available.
-
Oral anticoagulant switching in patients with atrial fibrillation: a scoping review.BMJ Open. 2023 Apr 25;13(4):e071907. doi: 10.1136/bmjopen-2023-071907. BMJ Open. 2023. PMID: 37185198 Free PMC article.
References
-
- Hart RG, Pearce LA. Current status of stroke risk stratification in patients with atrial fibrillation. Stroke. 2009;40:2607–10. - PubMed
-
- Wang TJ, Massaro JM, Levy D, et al. A risk score for predicting stroke or death in individuals with new-onset atrial fibrillation in the community. JAMA. 2003;290:1049–56. - PubMed
-
- Connolly SJ, Ezekowitz MD, Yusuf F, et al. RE-LY steering committee and investigators. Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med. 2009;361:1139–51. - PubMed
-
- Patel MR, Mahaffey KW, Garg J the ROCKET AF Steering Committee, for the ROCKET AF Investigators. Rivaroxaban versus warfarin in nonvalvular atrial fibrillation. N Engl J Med. 2011;365:883–91. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
