[Profile and evolution of chronic complex patients in a subacute unit]
- PMID: 28292582
- PMCID: PMC6876035
- DOI: 10.1016/j.aprim.2016.11.010
[Profile and evolution of chronic complex patients in a subacute unit]
Abstract
Objective: To improve the management of geriatric pluripathologic patients in Catalonia, the identification of chronic complex patient (PCC) or patients with advanced chronic disease (MACA) has been promoted. Patients with exacerbated chronic diseases are promoted to be admitted in subacute units (SG) located in intermediate hospitals and specialized in geriatric care, as an alternative to acute hospital. The results of the care process in patients identified as PCC/MACA in SG have not been evaluated.
Design: Descriptive-comparative, cross-sectional, and quantitative study.
Location: SG located in intermediate care hospital.
Participants: Consecutive patients admitted in the SG during 6months.
Main measurements: We compared baseline characteristics (demographic, clinical and geriatric assessment data), results at discharge and 30days post-discharge between PCC/MACA patients versus other patients.
Results: Of 244 patients (mean age±SD=85,6±7,5; 65.6%women), 91 (37,3%) were PCC/MACA (PCC=79,1%, MACA=20,9%). These, compared with unidentified patients, had greater comorbidity (Charlson index=3,2±1,8 vs 2,0; p=0,001) and polypharmacy (9,5±3,7 drugs vs 8,1±3,8; p=0,009). At discharge, the return to usual residence and mortality were comparable. PCC/MACA had higher mortality adding the mortality at 30day post-discharge (15,4% vs 8%; p=0,010). In a multi-variable analysis, PCC/MACA identification (p=0,006), as well as a history of dementia (p=0,004), was associated with mortality. Although PCC/MACA patients had higher readmission rate at 30day (18,7% vs 10,5%; p=0,014), in the multivariable analyses, only male, polypharmacy, and heart failure were independently associated to readmission.
Conclusions: Despite having more comorbidity and polypharmacy, the outcomes of patients identified as PCC/MACA at discharge of SG, were comparable with other patients, although they experienced more readmissions within 30days, possibly due to comorbidity and polypharmacy.
Objetivo: Para mejorar el manejo de pacientes pluripatológicos, en Cataluña se ha promovido la identificación como paciente crónico complejo (PCC) o con enfermedad crónica avanzada (MACA). Ante descompensaciones se promueve el ingreso de estos pacientes en unidades de subagudos (SG) ubicadas en hospitales de atención intermedia y especializadas en geriatría, como alternativa al hospital de agudos. Queremos evaluar los resultados del ingreso de PCC/MACA en SG.
Diseño: Estudio cuantitativo descriptivo-comparativo, transversal.
Emplazamiento: Unidad de subagudos de un hospital de atención intermedia.
Participantes: Pacientes ingresados consecutivamente en SG durante 6 meses.
Mediciones principales: Comparamos características basales (datos demográficos, clínicos y de valoración geriátrica integral), resultados al alta y a 30 días post-alta entre pacientes identificados como PCC/MACA vs otros pacientes.
Resultados: De 244 pacientes (promedio edad ± DE = 85,6 ± 7,5; 65,6% mujeres), 91 (37,3%) eran PCC/MACA (PCC = 79,1%, MACA = 20,9%). Estos, comparado con los no identificados, presentaban mayor comorbilidad (Charlson = 3,2 ± 1,8 vs 2,0; p = 0,001) y polifarmacia (9,5 ± 3,7 fármacos vs 8,1 ± 3,8, p = 0,009). Al alta, el retorno al domicilio habitual y la mortalidad fueron comparables. PCC/MACA tuvieron mayor mortalidad sumando los 30 días post-alta (15,4% vs 8%; p = 0,010); en un análisis multivariable, la identificación PCC/MACA (p = 0,006) y demencia (p = 0,004) se asociaba a mayor mortalidad. A pesar de que PCC/MACA reingresaban más a 30 días (18,7% vs 10,5%; p = 0,014), en el análisis multivariable las únicas variables asociadas independientemente a reingresos fueron sexo masculino, polifarmacia e insuficiencia cardiaca.
Conclusiones: A pesar de mayor comorbilidad y polifarmacia, los resultados de PCC/MACA al alta de SG fueron comparables con los otros pacientes, aunque experimentaron más reingresos a 30 días, posiblemente por su comorbilidad y polimedicación.
Keywords: Atención intermedia; Chronicity; Cronicidad; Intermediate care; Mortalidad; Mortality; Multimorbidity; Multimorbilidad; Readmissions; Reingresos; Subacute care unit; Subagudos.
Copyright © 2017 Elsevier España, S.L.U. All rights reserved.
Figures
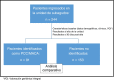
References
-
- Enquesta de salut de Catalunya 2013 [consultado 12 Feb 2016]. Disponible en: http://salutweb.gencat.cat/web/.content/home/el_departament/estadistique...
-
- De Brauwer I., d’Hoore W., Swine C., Thys F., Beguin C., Cornette P. Changes in the clinical features of older patients admitted from the emergency department. Arch Gerontol Geriatr. 2014;59:175–180. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

