Risk of tuberculosis in patients treated with TNF-α antagonists: a systematic review and meta-analysis of randomised controlled trials
- PMID: 28336735
- PMCID: PMC5372052
- DOI: 10.1136/bmjopen-2016-012567
Risk of tuberculosis in patients treated with TNF-α antagonists: a systematic review and meta-analysis of randomised controlled trials
Abstract
Objectives: An increased risk of tuberculosis (TB) has been reported in patients treated with TNF-α antagonists, an issue that has been highlighted in a WHO black box warning. This review aimed to assess the risk of TB in patients undergoing TNF-α antagonists treatment.
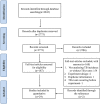
Methods: A systematic literature search for randomised controlled trials (RCTs) was performed in MEDLINE, Embase and Cochrane library and studies selected for inclusion according to predefined criteria. ORs with 95% CIs were calculated using the random-effect model. Subgroup analyses considered the effects of drug type, disease and TB endemicity. The quality of evidence was assessed using the Grades of Recommendation, Assessment, Development and Evaluation (GRADE) approach.
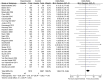
Results: 29 RCTs involving 11 879 patients were included (14 for infliximab, 9 for adalimumab, 2 for golimumab, 1 for etanercept and 3 for certolizumab pegol). Of 7912 patients allocated to TNF-α antagonists, 45 (0.57%) developed TB, while only 3 cases occurred in 3967 patients allocated to control groups, resulting in an OR of 1.94 (95% CI 1.10 to 3.44, p=0.02). Subgroup analyses indicated that patients of rheumatoid arthritis (RA) had a higher increased risk of TB when treated with TNF-α antagonists (OR 2.29 (1.09 to 4.78), p=0.03). The level of the evidence was recommended as 'low' by the GRADE system.
Conclusions: Findings from our meta-analysis indicate that the risk of TB may be significantly increased in patients treated with TNF-α antagonists. However, further studies are needed to reveal the biological mechanism of the increased TB risk caused by TNF-α antagonists treatment.
Keywords: RCTs; TNF-α antagonists; meta-analysis.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://www.bmj.com/company/products-services/rights-and-licensing/.
Conflict of interest statement
Figures


References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
