Balloon pulmonary angioplasty in chronic thromboembolic pulmonary hypertension
- PMID: 28356406
- PMCID: PMC9489135
- DOI: 10.1183/16000617.0119-2016
Balloon pulmonary angioplasty in chronic thromboembolic pulmonary hypertension
Erratum in
-
"Balloon pulmonary angioplasty in chronic thromboembolic pulmonary hypertension." Irene Lang, Bernhard C. Meyer, Takeshi Ogo, Hiromi Matsubara, Marcin Kurzyna, Hossein-Ardeschir Ghofrani, Eckhard Mayer and Philippe Brenot. Eur Respir Rev 2017; 26: 160119.Eur Respir Rev. 2017 Jun 14;26(144):165119. doi: 10.1183/16000617.5119-2016. Print 2017 Jun 30. Eur Respir Rev. 2017. PMID: 28615306 Free PMC article. No abstract available.
Abstract
Chronic thromboembolic pulmonary hypertension (CTEPH) is thought to result from incomplete resolution of pulmonary thromboemboli that undergo organisation into fibrous tissue within pulmonary arterial branches, filling pulmonary arterial lumina with collagenous obstructions. The treatment of choice is pulmonary endarterectomy (PEA) in CTEPH centres, which has low post-operative mortality and good long-term survival. For patients ineligible for PEA or who have recurrent or persistent pulmonary hypertension after surgery, medical treatment with riociguat is beneficial. In addition, percutaneous balloon pulmonary angioplasty (BPA) is an emerging option, and promises haemodynamic and functional benefits for inoperable patients. In contrast to conventional angioplasty, BPA with undersized balloons over guide wires exclusively breaks intraluminal webs and bands, without dissecting medial vessel layers, and repeat sessions are generally required. Observational studies report that BPA improves haemodynamics, symptoms and functional capacity in patients with CTEPH, but controlled trials with long-term follow-up are needed. Complications include haemoptysis, wire injury, vessel dissection, vessel rupture, reperfusion pulmonary oedema, pulmonary parenchymal bleeding and haemorrhagic pleural effusions. This review summarises the available evidence for BPA, patient selection, recent technical refinements and periprocedural imaging, and discusses the potential future role of BPA in the management of CTEPH.
Copyright ©ERS 2017.
Conflict of interest statement
Conflict of interest: Disclosures can be found alongside this article at
Figures
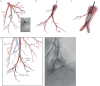
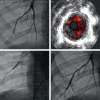
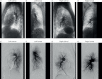

References
-
- Galiè N, Humbert M, Vachiery JL, et al. 2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension. The Joint Task Force for the Diagnosis and Treatment of Pulmonary Hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS). Eur Respir J 2015; 46: 903–975. - PubMed
-
- Banks DA, Pretorius GV, Kerr KM, et al. Pulmonary endarterectomy: part I. Pathophysiology, clinical manifestations, and diagnostic evaluation of chronic thromboembolic pulmonary hypertension. Semin Cardiothorac Vasc Anesth 2014; 18: 319–330. - PubMed
-
- Fedullo P, Kerr KM, Kim NH, et al. Chronic thromboembolic pulmonary hypertension. Am J Respir Crit Care Med 2011; 183: 1605–1613. - PubMed
-
- Kim NH. Group 4 pulmonary hypertension. Chronic thromboembolic pulmonary hypertension: epidemiology, pathophysiology, and treatment. Cardiol Clin 2016; 34: 435–441. - PubMed
-
- Lang IM, Dorfmüller P, Vonk Noordegraaf A. The pathobiology of chronic thromboembolic pulmonary hypertension. Ann Am Thorac Soc 2016; 13 Suppl 3: S215–S221. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
