Dynamic balance in children with attention-deficit hyperactivity disorder and its relationship with cognitive functions and cerebellum
- PMID: 28356743
- PMCID: PMC5367596
- DOI: 10.2147/NDT.S125169
Dynamic balance in children with attention-deficit hyperactivity disorder and its relationship with cognitive functions and cerebellum
Abstract
Background: Attention-deficit hyperactivity disorder (ADHD) is linked to the presence of motor deficiencies, including balance deficits. The cerebellum serves as an integrative structure for balance control and is also involved in cognition, including timing and anticipatory regulation. Cerebellar development may be delayed in children and adolescents with ADHD, and inconsistent reaction time is commonly seen in ADHD. We hypothesized that dynamic balance deficits would be present in children with ADHD and they would correlate with attention and cerebellar functions.
Methods: Sixty-two children with ADHD and no other neurological conditions and 62 typically developing (TD) children were examined with five trials of the Phyaction Balance Board, an electronic balancing platform. Cerebellar clinical symptoms were evaluated using an international ataxia rating scale. Conners' Continuous Performance Test was used to evaluate patterns of reaction.
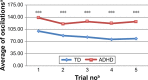
Results: Children with ADHD had poorer performance on balancing tasks, compared to TD children (P<0.001). They exhibited significantly greater sway amplitudes than TD children (P<0.001) in all of the five balancing trials. The effect size of the difference between the groups increased continuously from the first to the last trial. Balance score in both groups was related to the variation in the reaction time, including reaction time standard error (r =0.25; P=0.0409, respectively, r =0.31; P=0.0131) and Variability of Standard Error (r =0.28; P=0.0252, respectively, r =0.41; P<0.001). The burden of cerebellar symptoms was strongly related to balance performance in both groups (r =0.50, P<0.001; r =0.49, P=0.001).
Conclusion: This study showed that ADHD may be associated with poor dynamic balance control. Furthermore, we showed that maintaining balance correlates with neuropsychological measures of consistency of reaction time. Balance deficits and impaired cognitive functioning could reflect a common cerebellar dysfunction in ADHD children.
Keywords: attention-deficit hyperactivity disorder; balance; cerebellum; reaction time.
Conflict of interest statement
Disclosure Dr Goetz serves as a speaker for Eli Lilly CR. Dr Surman reports that since the last year, he has been a consultant to Ironshore, Rhodes, and Shire; has presented educational lectures for Neos, Graduate Medical Education Continuing Medical Education (CME), and Massachusetts General Hospital (MGH) Academy; and has received research support from Neurocentria, Pamlab, and Shire. He also reports receiving royalties for Fast Minds: How to Thrive If You Have ADHD (Or Think You Might) and ADHD in Adults: A Practical Guide to Evaluation and Management. Dr Schwabova, Dr Hlavka, and Dr Ptacek report no conflicts of interest in this work.
Figures
References
-
- Landgren MM, Pettersson RR, Kjellman BB, Gillberg CC. ADHD, DAMP and other neurodevelopmental/psychiatric disorders in 6-year-old children: epidemiology and co-morbidity. Dev Med Child Neurol. 1996;38(10):891–906. - PubMed
-
- Gustafsson P, Svedin CG, Ericsson I, Lindén C, Karlsson MK, Thernlund G. Reliability and validity of the assessment of neurological soft-signs in children with and without attention-deficit-hyperactivity disorder. Dev Med Child Neurol. 2010;52(4):364–370. - PubMed
-
- Ferrin M, Vance A. Examination of neurological subtle signs in ADHD as a clinical tool for the diagnosis and their relationship to spatial working memory. J Child Psychol Psychiatry. 2011;53(4):390–400. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

