Fast renal decline to end-stage renal disease: an unrecognized feature of nephropathy in diabetes
- PMID: 28366227
- PMCID: PMC5429989
- DOI: 10.1016/j.kint.2016.10.046
Fast renal decline to end-stage renal disease: an unrecognized feature of nephropathy in diabetes
Abstract
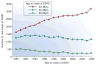
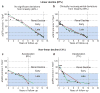
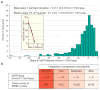
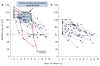
A new model of diabetic nephropathy in type 1 diabetes emerged from our studies of Joslin Clinic patients. The dominant feature is progressive renal decline, not albuminuria. This decline is a unidirectional process commencing while patients have normal renal function and, in the majority, progressing steadily (linearly) to end-stage renal disease (ESRD). While an individual's rate of renal decline is constant, the estimated glomerular filtration rate (eGFR) slope varies widely among individuals from -72 to -3.0 ml/min/year. Kidney Disease: Improving Global Outcomes guidelines define rapid progression as rate of eGFR declines > 5 ml/min/year, a value exceeded by 80% of patients in Joslin's type 1 diabetes ESRD cohort. The extraordinary range of slopes within the rapid progression category prompted us to partition it into "very fast," "fast" and "moderate" decline. We showed, for the first time, that very fast and fast decline from normal eGFR to ESRD within 2 to 10 years constitutes 50% of the Joslin cohort. In this review we present data about frequency of fast decliners in both diabetes types, survey some mechanisms underlying fast renal decline, discuss methods of identifying patients at risk and comment on the need for effective therapeutic interventions. Whether the initiating mechanism of fast renal decline affects glomerulus, tubule, interstitium or vasculature is unknown. Since no animal model mimics progressive renal decline, studies in humans are needed. Prospective studies searching for markers predictive of the rate of renal decline yield findings that may make detection of fast decliners feasible. Identifying such patients will be the foundation for developing effective individualized methods to prevent or delay onset of ESRD in diabetes.
Keywords: chronic kidney disease; diabetic nephropathy; end-stage renal disease; renal decline.
Copyright © 2017 International Society of Nephrology. Published by Elsevier Inc. All rights reserved.
Figures
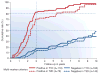
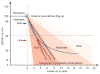
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

