Peripheral blood lymphocyte-to-monocyte ratio as a prognostic factor in advanced epithelial ovarian cancer: a multicenter retrospective study
- PMID: 28382135
- PMCID: PMC5381161
- DOI: 10.7150/jca.17668
Peripheral blood lymphocyte-to-monocyte ratio as a prognostic factor in advanced epithelial ovarian cancer: a multicenter retrospective study
Abstract
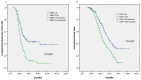
The lymphocyte-to-monocyte ratio (LMR), as a surrogate marker of systemic inflammation, has been found to be a novel prognostic indicator in various malignancies. Data from 672 advanced epithelial ovarian cancer (EOC) patients treated with neoadjuvant chemotherapy (NAC) followed by debulking surgery were analyzed, and the prognostic value of LMR were evaluated. The optimal cutoff point of LMR in prediction of survival was defined as 3.45 through receiver operating characteristics curve analysis. Patients with low LMR (≤3.45) at diagnosis tended to have more adverse clinical features, such as higher histological grade, chemotherapy resistance, and residual tumor >1cm after debulking surgery. No significant correlation was found between LMR level and age and histological type. Moreover, after NAC, the complete remission (CR) rate for the low-LMR group was lower than those for the high-LMR group (P<0.05). Patients with low LMR had poorer progression-free survival (PFS; P<0.001) and overall survival (OS; P<0.001). Multivariate analysis revealed that low LMR was an independent adverse predictor for PFS and OS. Results indicated that low LMR at diagnosis is a novel independent prognostic factor for advanced EOC. However, prospective study is needed to validate this prognostic factor and biological studies should further investigate the mechanisms underlying the correlation between low LMR and poor prognosis in advanced EOC.
Keywords: epithelial ovarian cancer; lymphocyte-to-monocyteratio; neoadjuvant chemotherapy; prognosis.
Conflict of interest statement
Competing Interests: The authors have declared that no competing interest exists.
Figures

Similar articles
-
Prognostic value of preoperative lymphocyte-monocyte ratio in elderly patients with advanced epithelial ovarian cancer.Obstet Gynecol Sci. 2017 Nov;60(6):558-564. doi: 10.5468/ogs.2017.60.6.558. Epub 2017 Oct 31. Obstet Gynecol Sci. 2017. PMID: 29184864 Free PMC article.
-
[The relationship of preoperativelymphocyte-monocyte ratio and the clinicopathological characteristics and prognosis of patients with epithelial ovarian cancer].Zhonghua Zhong Liu Za Zhi. 2017 Sep 23;39(9):676-680. doi: 10.3760/cma.j.issn.0253-3766.2017.09.007. Zhonghua Zhong Liu Za Zhi. 2017. PMID: 28926896 Chinese.
-
Lymphocyte-to-monocyte ratio after primary surgery is an independent prognostic factor for patients with epithelial ovarian cancer: A propensity score matching analysis.Front Oncol. 2023 Mar 22;13:1139929. doi: 10.3389/fonc.2023.1139929. eCollection 2023. Front Oncol. 2023. PMID: 37035193 Free PMC article.
-
Prognostic value of lymphocyte-to-monocyte ratio in ovarian cancer: a meta-analysis.J Ovarian Res. 2019 May 31;12(1):51. doi: 10.1186/s13048-019-0527-z. J Ovarian Res. 2019. PMID: 31151469 Free PMC article. Review.
-
The predictive value of dynamic monitoring of peripheral blood lymphocyte to monocyte ratio in patients with extranodal NK/T cell lymphoma.Cancer Cell Int. 2019 Oct 22;19:272. doi: 10.1186/s12935-019-0993-9. eCollection 2019. Cancer Cell Int. 2019. PMID: 31649489 Free PMC article. Review.
Cited by
-
Prognostic value of pretreatment lymphocyte-to-monocyte ratio in patients with urologic tumors: A PRISMA-compliant meta-analysis.Medicine (Baltimore). 2019 Jan;98(2):e14091. doi: 10.1097/MD.0000000000014091. Medicine (Baltimore). 2019. PMID: 30633220 Free PMC article.
-
The association of neutrophil-lymphocyte ratio and lymphocyte-monocyte ratio with 3-month clinical outcome after mechanical thrombectomy following stroke.J Neuroinflammation. 2020 Feb 18;17(1):60. doi: 10.1186/s12974-020-01739-y. J Neuroinflammation. 2020. PMID: 32070366 Free PMC article.
-
Diagnostic performances of neutrophil to lymphocyte ratio and lymphocyte to monocyte ratio in acute ischemic stroke caused by cervicocranial arterial dissection.J Clin Lab Anal. 2020 Dec;34(12):e23515. doi: 10.1002/jcla.23515. Epub 2020 Sep 7. J Clin Lab Anal. 2020. PMID: 32893925 Free PMC article.
-
Lymphocyte-to-Monocyte Ratio Is Independently Associated with Progressive Infarction in Patients with Acute Ischemic Stroke.Biomed Res Int. 2022 Dec 27;2022:2290524. doi: 10.1155/2022/2290524. eCollection 2022. Biomed Res Int. 2022. PMID: 36605104 Free PMC article.
-
Low Preoperative Lymphocyte to Monocyte Ratio Serves as a Worse Prognostic Marker in Patients with Esophageal Squamous Cell Carcinoma Undergoing Curative Tumor Resection.J Cancer. 2019 May 12;10(9):2057-2062. doi: 10.7150/jca.29383. eCollection 2019. J Cancer. 2019. PMID: 31205566 Free PMC article.
References
-
- Ferlay J, Parkin DM, Steliarova-Foucher E. Estimates of cancer incidence and mortality in Europe in 2008. European journal of cancer (Oxford, England: 1990) 2010;46(4):765–81. - PubMed
-
- Cannistra SA. Cancer of the ovary. The New England journal of medicine. 2004;351(24):2519–29. - PubMed
-
- Schwartz PE, Zheng W. Neoadjuvant chemotherapy for advanced ovarian cancer: the role of cytology in pretreatment diagnosis. Gynecologic oncology. 2003;90(3):644–50. - PubMed
-
- Lewin SN, Herzog TJ, Barrena Medel NI, Deutsch I, Burke WM, Sun X. et al. Comparative performance of the 2009 international Federation of gynecology and obstetrics' staging system for uterine corpus cancer. Obstetrics and gynecology. 2010;116(5):1141–9. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

