Coronary stenting: A matter of revascularization
- PMID: 28400917
- PMCID: PMC5368670
- DOI: 10.4330/wjc.v9.i3.207
Coronary stenting: A matter of revascularization
Abstract
In the last few decades, the recommended treatment for coronary artery disease has been dramatically improved by percutaneous coronary intervention (PCI) and the use of balloon catheters, bare metal stents (BMSs), and drug-eluting stents (DESs). Catheter balloons were burdened by acute vessel occlusion or target-lesion re-stenosis. BMSs greatly reduced those problems holding up the vessel structure, but showed high rates of in-stent re-stenosis, which is characterized by neo-intimal hyperplasia and vessel remodeling leading to a re-narrowing of the vessel diameter. This challenge was overtaken by first-generation DESs, which reduced re-stenosis rates to nearly 5%, but demonstrated delayed arterial healing and risk for late in-stent thrombosis, with inflammatory cells playing a pivotal role. Finally, new-generation DESs, characterized by innovations in design, metal composition, surface polymers, and anti-proliferative drugs, finally reduced the risk for stent thrombosis and greatly improved revascularization outcomes. New advances include bioresorbable stents potentially changing the future of revascularization techniques as the concept bases upon the degradation of the stent scaffold to inert particles after its function expired, thus theoretically eliminating risks linked with both stent thrombosis and re-stenosis. Talking about DESs also dictates to consider dual antiplatelet therapy (DAPT), which is a fundamental moment in view of the good outcome duration, but also deals with bleeding complications. The better management of patients undergoing PCI should include the use of DESs and a DAPT finely tailored in consideration of the potentially developing bleeding risk in accordance with the indications from last updated guidelines.
Keywords: Bare metal stent; Coronary artery disease; Drug-eluting stent; In-stent re-stenosis; Stent thrombosis.
Conflict of interest statement
Conflict-of-interest statement: Bonaventura A, Montecucco F and Liberale L declare no conflict of interest related to this publication.
Figures
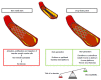
Similar articles
-
Efficacy and Safety of Drug-Eluting Stents Optimized for Biocompatibility vs Bare-Metal Stents With a Single Month of Dual Antiplatelet Therapy: A Meta-analysis.JAMA Cardiol. 2018 Nov 1;3(11):1050-1059. doi: 10.1001/jamacardio.2018.3551. JAMA Cardiol. 2018. PMID: 30383145 Free PMC article.
-
Percutaneous coronary intervention: assessing coronary vascular risk associated with bare-metal and drug-eluting stents.Am J Manag Care. 2009 Mar;15(2 Suppl):S42-7. Am J Manag Care. 2009. PMID: 19355808 Review.
-
Frequency of coronary arterial late angiographic stent thrombosis (LAST) in the first six months: outcomes with drug-eluting stents versus bare metal stents.Am J Cardiol. 2007 Mar 15;99(6):774-8. doi: 10.1016/j.amjcard.2006.10.033. Epub 2007 Jan 19. Am J Cardiol. 2007. PMID: 17350363
-
Meta-analysis of drug eluting stents compared with bare metal stents in high bleeding risk patients undergoing percutaneous coronary interventions.Catheter Cardiovasc Interv. 2019 Jul 1;94(1):98-104. doi: 10.1002/ccd.28045. Epub 2018 Dec 26. Catheter Cardiovasc Interv. 2019. PMID: 30585391
-
Meta-analysis of long-term outcomes for drug-eluting stents versus bare-metal stents in primary percutaneous coronary interventions for ST-segment elevation myocardial infarction.Am J Cardiol. 2012 Apr 1;109(7):932-40. doi: 10.1016/j.amjcard.2011.11.021. Epub 2012 Jan 3. Am J Cardiol. 2012. PMID: 22221949 Review.
Cited by
-
The association between stent type and developing angina pectoris following percutaneous coronary intervention.BMC Cardiovasc Disord. 2024 Sep 2;24(1):466. doi: 10.1186/s12872-024-04116-2. BMC Cardiovasc Disord. 2024. PMID: 39218866 Free PMC article.
-
Paclitaxel-eluting stents versus paclitaxel-coated balloons in coronary artery disease: a meta-analysis of randomized controlled trials.Glob Cardiol Sci Pract. 2024 Mar 3;2024(2):e202412. doi: 10.21542/gcsp.2024.12. eCollection 2024 Mar 3. Glob Cardiol Sci Pract. 2024. PMID: 38746063 Free PMC article. Review.
References
-
- Brophy JM, Belisle P, Joseph L. Evidence for use of coronary stents. A hierarchical bayesian meta-analysis. Ann Intern Med. 2003;138:777–786. - PubMed
-
- Stettler C, Wandel S, Allemann S, Kastrati A, Morice MC, Schömig A, Pfisterer ME, Stone GW, Leon MB, de Lezo JS, et al. Outcomes associated with drug-eluting and bare-metal stents: a collaborative network meta-analysis. Lancet. 2007;370:937–948. - PubMed
-
- Kastrati A, Mehilli J, Dirschinger J, Dotzer F, Schühlen H, Neumann FJ, Fleckenstein M, Pfafferott C, Seyfarth M, Schömig A. Intracoronary stenting and angiographic results: strut thickness effect on restenosis outcome (ISAR-STEREO) trial. Circulation. 2001;103:2816–2821. - PubMed
-
- Pache J, Kastrati A, Mehilli J, Schühlen H, Dotzer F, Hausleiter J, Fleckenstein M, Neumann FJ, Sattelberger U, Schmitt C, et al. Intracoronary stenting and angiographic results: strut thickness effect on restenosis outcome (ISAR-STEREO-2) trial. J Am Coll Cardiol. 2003;41:1283–1288. - PubMed
-
- Mehilli J, Pache J, Abdel-Wahab M, Schulz S, Byrne RA, Tiroch K, Hausleiter J, Seyfarth M, Ott I, Ibrahim T, et al. Drug-eluting versus bare-metal stents in saphenous vein graft lesions (ISAR-CABG): a randomised controlled superiority trial. Lancet. 2011;378:1071–1078. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

