Brain invasion in meningiomas-clinical considerations and impact of neuropathological evaluation: a systematic review
- PMID: 28419308
- PMCID: PMC5596167
- DOI: 10.1093/neuonc/nox071
Brain invasion in meningiomas-clinical considerations and impact of neuropathological evaluation: a systematic review
Abstract
With the release of the 2016 edition of the World Health Organization (WHO) Classification of Central Nervous System Tumors, brain invasion in meningiomas has been added as a stand-alone criterion for atypia and can therefore impact grading and indirectly adjuvant therapy. Regarding this rising clinical importance, we have reviewed the current knowledge about brain invasion with emphasis on its implications on current and future clinical practice. We found various definitions of brain invasion and approaches for evaluation in surgically obtained specimens described over the past decades. This heterogeneity is reflected by weak correlation with prognosis and remains controversial. Similarly, associated clinical factors are largely unknown. Preoperative, imaging-guided detection of brain invasion is unspecific, and intraoperative assessment using standard and new high-magnification microscopic techniques remains imprecise. Despite the increasing knowledge about molecular alterations of the tumor/ brain surface, pharmacotherapeutic options targeting brain invasive meningiomas are lacking. Finally, we summarize the impact of brain invasion on histopathological grading in the WHO classifications of brain tumors since 1979.In conclusion, standardized neurosurgical sampling and neuropathological analyses could improve diagnostic reliability and reproducibility of future studies. Further research is needed to improve pre- and intraoperative visualization of brain invasion and to develop adjuvant, targeted therapies.
Keywords: brain invasion; grading; meningioma; prognosis; resection.
© The Author(s) 2017. Published by Oxford University Press on behalf of the Society for Neuro-Oncology. All rights reserved. For permissions, please e-mail: journals.permissions@oup.com.
Figures
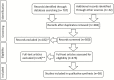
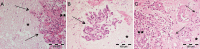
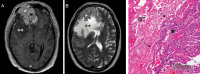

References
-
- Perry A, Louis DN, von Deimling A, et al. Meningiomas. In: Louis DN, Ohgaki H, Wiestler ODet al. , eds. WHO Classification of Tumors of the Central Nervous System. Lyon: International Agency on Cancer Research; 2016:232–245.
-
- Mantle RE, Lach B, Delgado MR, Baeesa S, Bélanger G. Predicting the probability of meningioma recurrence based on the quantity of peritumoral brain edema on computerized tomography scanning. J Neurosurg. 1999;91(3):375–383. - PubMed
-
- McLean CA, Jolley D, Cukier E, Giles G, Gonzales MF. Atypical and malignant meningiomas: importance of micronecrosis as a prognostic indicator. Histopathology. 1993;23(4):349–353. - PubMed
-
- Pizem J, Velnar T, Prestor B, Mlakar J, Popovic M. Brain invasion assessability in meningiomas is related to meningioma size and grade, and can be improved by extensive sampling of the surgically removed meningioma specimen. Clin Neuropathol. 2014;33(5):354–363. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

