ONC201 Demonstrates Antitumor Effects in Both Triple-Negative and Non-Triple-Negative Breast Cancers through TRAIL-Dependent and TRAIL-Independent Mechanisms
- PMID: 28424227
- PMCID: PMC5564301
- DOI: 10.1158/1535-7163.MCT-17-0121
ONC201 Demonstrates Antitumor Effects in Both Triple-Negative and Non-Triple-Negative Breast Cancers through TRAIL-Dependent and TRAIL-Independent Mechanisms
Abstract
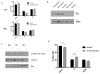
Breast cancer is a major cause of cancer-related death. TNF-related apoptosis-inducing ligand (TRAIL) has been of interest as a cancer therapeutic, but only a subset of triple-negative breast cancers (TNBC) is sensitive to TRAIL. The small-molecule ONC201 induces expression of TRAIL and its receptor DR5. ONC201 has entered clinical trials in advanced cancers. Here, we show that ONC201 is efficacious against both TNBC and non-TNBC cells (n = 13). A subset of TNBC and non-TNBC cells succumbs to ONC201-induced cell death. In 2 of 8 TNBC cell lines, ONC201 treatment induces caspase-8 cleavage and cell death that is blocked by TRAIL-neutralizing antibody RIK2. The proapoptotic effect of ONC201 translates to in vivo efficacy in the MDA-MB-468 xenograft model. In most TNBC lines tested (6/8), ONC201 has an antiproliferative effect but does not induce apoptosis. ONC201 decreases cyclin D1 expression and causes an accumulation of cells in the G1 phase of the cell cycle. pRb expression is associated with sensitivity to the antiproliferative effects of ONC201, and the compound synergizes with taxanes in less sensitive cells. All non-TNBC cells (n = 5) are growth inhibited following ONC201 treatment, and unlike what has been observed with TRAIL, a subset (n = 2) shows PARP cleavage. In these cells, cell death induced by ONC201 is TRAIL independent. Our data demonstrate that ONC201 has potent antiproliferative and proapoptotic effects in a broad range of breast cancer subtypes, through TRAIL-dependent and TRAIL-independent mechanisms. These findings develop a preclinical rationale for developing ONC201 as a single agent and/or in combination with approved therapies in breast cancer. Mol Cancer Ther; 16(7); 1290-8. ©2017 AACR.
©2017 American Association for Cancer Research.
Figures
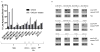
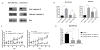


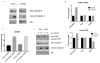
Similar articles
-
Metformin sensitizes triple-negative breast cancer to proapoptotic TRAIL receptor agonists by suppressing XIAP expression.Breast Cancer Res Treat. 2017 Jun;163(3):435-447. doi: 10.1007/s10549-017-4201-0. Epub 2017 Mar 21. Breast Cancer Res Treat. 2017. PMID: 28324269 Free PMC article.
-
ONC201 activates ER stress to inhibit the growth of triple-negative breast cancer cells.Oncotarget. 2017 Mar 28;8(13):21626-21638. doi: 10.18632/oncotarget.15451. Oncotarget. 2017. PMID: 28423492 Free PMC article.
-
Etoposide and doxorubicin enhance the sensitivity of triple negative breast cancers through modulation of TRAIL-DR5 axis.Apoptosis. 2017 Oct;22(10):1205-1224. doi: 10.1007/s10495-017-1400-4. Apoptosis. 2017. PMID: 28702823
-
Targeting TRAIL Death Receptors in Triple-Negative Breast Cancers: Challenges and Strategies for Cancer Therapy.Cells. 2022 Nov 22;11(23):3717. doi: 10.3390/cells11233717. Cells. 2022. PMID: 36496977 Free PMC article. Review.
-
ONC201 and imipridones: Anti-cancer compounds with clinical efficacy.Neoplasia. 2020 Dec;22(12):725-744. doi: 10.1016/j.neo.2020.09.005. Epub 2020 Oct 23. Neoplasia. 2020. PMID: 33142238 Free PMC article. Review.
Cited by
-
Role of Dopamine Receptors in the Anticancer Activity of ONC201.Neoplasia. 2018 Jan;20(1):80-91. doi: 10.1016/j.neo.2017.10.002. Epub 2017 Dec 5. Neoplasia. 2018. PMID: 29216597 Free PMC article.
-
Human ILC3 Exert TRAIL-Mediated Cytotoxicity Towards Cancer Cells.Front Immunol. 2022 Mar 1;13:742571. doi: 10.3389/fimmu.2022.742571. eCollection 2022. Front Immunol. 2022. PMID: 35300331 Free PMC article.
-
Dasatinib promotes TRAIL-mediated apoptosis by upregulating CHOP-dependent death receptor 5 in gastric cancer.FEBS Open Bio. 2018 Mar 23;8(5):732-742. doi: 10.1002/2211-5463.12404. eCollection 2018 May. FEBS Open Bio. 2018. PMID: 29744288 Free PMC article.
-
CDH1 overexpression sensitizes TRAIL resistant breast cancer cells towards rhTRAIL induced apoptosis.Mol Biol Rep. 2023 Sep;50(9):7283-7294. doi: 10.1007/s11033-023-08657-1. Epub 2023 Jul 8. Mol Biol Rep. 2023. PMID: 37422537
-
ONC201: a new treatment option being tested clinically for recurrent glioblastoma.Transl Cancer Res. 2017 Oct;6(Suppl 7):S1239-S1243. doi: 10.21037/tcr.2017.10.03. Transl Cancer Res. 2017. PMID: 30175049 Free PMC article.
References
-
- Walczak H, et al. Tumoricidal activity of tumor necrosis factor-related apoptosis-inducing ligand in vivo. Nat Med. 1999;5:157–163. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

