Self-reported adherence and associated factors to isoniazid preventive therapy for latent tuberculosis among people living with HIV/AIDS at health centers in Gondar town, North West Ethiopia
- PMID: 28435232
- PMCID: PMC5391840
- DOI: 10.2147/PPA.S131314
Self-reported adherence and associated factors to isoniazid preventive therapy for latent tuberculosis among people living with HIV/AIDS at health centers in Gondar town, North West Ethiopia
Abstract
Purpose: This study aimed to assess self-reported adherence and associated factors to isoniazid preventive therapy (IPT) for latent tuberculosis among people living with HIV/AIDS (PLWHA) at health centers in Gondar town, North West Ethiopia.
Patients and methods: An institution-based prospective cross-sectional study was conducted from March 10 to June 11, 2016. A total of 154 eligible participants were included in the study, using the simple random sampling method, from the available four health centers and one teaching referral hospital that provided antiretroviral therapy (ART) for HIV/AIDS patients. Adherence was measured by self-report of isoniazid (INH) tablets taken for the preceding 7 days. Participants were recruited through in-depth interviews. The collected data were entered and analyzed using the statistical packages for social sciences (SPSS) version 20.
Results: The adherence level to IPT was 90.3% for the last 7 days of the study. ART was initiated for 84.4%, and all of them were on a first-line regimen. Isoniazid-related side effects were reported by 48 (31.2%) participants, of which the most commonly identified were abdominal pain, vomiting, skin rash, jaundice, and numbness. Only 3 (2%) participants discontinued from the study. In the bivariate logistic regression analysis, respondents who had received an explanation about IPT were 83% times more likely to be adherent compared to those who had not received it (95% CI, AOR: 0.266 [0.23-3.127]). Respondents who had taken IPT for ≥5 months were more likely to be adherent than those who had taken it for 1-2 months [95% CI, COR: 1.484]. On the other hand, respondents who experienced side effects were 36% less likely to be adherent compared to those who did not experience any.
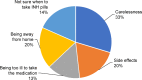
Conclusion: The level of adherence to IPT among PLWHA was high. Among the predictors reported, carelessness and/or forgetfulness, side effects, and absence from home were the major factors identified for being nonadherent. Health professionals and the Ministry of Health should design and deliver appropriate health education tips and messages. Moreover, counseling of patients who are in their first 2 months of therapy should be strengthened further.
Keywords: HIV/AIDS; adherence; isoniazid; preventive therapy; side effects.
Conflict of interest statement
Disclosure Financial support was provided only by the authors. The authors report no other conflicts of interest in this work.
Figures
References
-
- WHO . Global Tuberculosis Control. Geneva: World Health Organization; 2011. Available from: http://www.who.int/tb/publications/glob1port/2011/gtbr11_full.pdf.
-
- Sharma SK, Mohan A, Kadhiravan T. HIV-TB co-infection: epidemiology, diagnosis & management. Indian J Med Res. 2005;121:550–567. - PubMed
-
- Sterling TR, Pham PA, Chaisson RE. HIV Infection – related tuberculosis: clinical manifestations and treatment. Clin Infect Dis. 2010;50:S223–S230. - PubMed
-
- Getahun H, Gunneberg C, Granich R, Nunn P. HIV Infection associated tuberculosis: the epidemiology and the response. Clin Infect Dis. 2010;50:S201–S207. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources