Plasma concentrations of lipids during pregnancy and the risk of gestational diabetes mellitus: A longitudinal study
- PMID: 28436169
- PMCID: PMC5837900
- DOI: 10.1111/1753-0407.12563
Plasma concentrations of lipids during pregnancy and the risk of gestational diabetes mellitus: A longitudinal study
Abstract
Background: Abnormal lipid profiles have been associated with gestational diabetes mellitus (GDM), but studies with longitudinal measures of lipids throughout pregnancy are sparse. The aim of the present study was to characterize longitudinal changes in lipid profiles throughout pregnancy and prospectively examine the associations of plasma lipid concentrations with risk of GDM.
Methods: This study was a nested case-control study including 107 GDM cases and 214 matched non-GDM controls from participants in the National Institute of Child Health and Human Development (NICHD) Fetal Growth Studies - Singleton cohort. Blood samples were collected longitudinally at Gestational Weeks (GW) 10-14, 15-26 (fasting sample), 23-31, and 33-39. Plasma concentrations of triglycerides, total cholesterol, and high-density lipoprotein cholesterol (HDL-C) were measured by enzymatic assays. Low-density lipoprotein cholesterol (LDL-C) was calculated using Friedewald's formula.
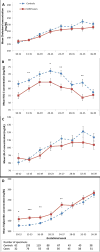
Results: Plasma triglycerides, total cholesterol, and LDL-C increased as pregnancy progressed. At GW 10-14, the adjusted odds ratios (aORs) of GDM comparing the highest versus lowest quartile were 3.15 (95% confidence interval [CI] 1.38-7.15; P trend = 0.002) for triglycerides and 0.44 (95% CI 0.18-1.09; P trend = 0.045) for HDL-C. At GW 15-26, the aORs were 6.57 (95% CI 2.25-19.17; P trend = 0.001) for triglycerides and 0.23 (95% CI 0.08-0.63; P trend = 0.005) for HDL-C. No significant associations were observed for total cholesterol and LDL-C concentrations with risk of GDM.
Conclusions: Higher plasma triglyceride and lower HDL-C concentrations in early and mid-pregnancy were significantly associated with a greater risk of GDM. Total cholesterol and LDL-C concentrations during pregnancy were not significantly associated with GDM risk.
Keywords: cholesterol; gestational diabetes; lipids; pregnancy; triglycerides; 三酰甘油; 妊娠; 妊娠糖尿病; 胆固醇; 血脂.
© 2017 Ruijin Hospital, Shanghai Jiaotong University School of Medicine and John Wiley & Sons Australia, Ltd.
Conflict of interest statement
Figures

Similar articles
-
[The value of fasting plasma glucose and lipid profiles between 7 and 15 gestational weeks in the prediction of gestational diabetes mellitus].Zhonghua Fu Chan Ke Za Zhi. 2016 Nov 25;51(11):835-839. doi: 10.3760/cma.j.issn.0529-567X.2016.11.007. Zhonghua Fu Chan Ke Za Zhi. 2016. PMID: 27916067 Chinese.
-
Early Pregnancy Maternal Lipid Profiles and the Risk of Gestational Diabetes Mellitus Stratified for Body Mass Index.Reprod Sci. 2015 Jun;22(6):712-7. doi: 10.1177/1933719114557896. Epub 2014 Nov 12. Reprod Sci. 2015. PMID: 25394643 Free PMC article.
-
Associations between maternal lipid profile and pregnancy complications and perinatal outcomes: a population-based study from China.BMC Pregnancy Childbirth. 2016 Mar 21;16:60. doi: 10.1186/s12884-016-0852-9. BMC Pregnancy Childbirth. 2016. PMID: 27000102 Free PMC article.
-
Changes in serum lipid levels during pregnancy in women with gestational diabetes. A narrative review.Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2021 Mar;165(1):8-12. doi: 10.5507/bp.2021.009. Epub 2021 Jan 25. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2021. PMID: 33500589 Review.
-
Maternal Dyslipidaemia in Pregnancy with Gestational Diabetes Mellitus: Possible Impact on Foetoplacental Vascular Function and Lipoproteins in the Neonatal Circulation.Curr Vasc Pharmacol. 2019;17(1):52-71. doi: 10.2174/1570161115666171116154247. Curr Vasc Pharmacol. 2019. PMID: 29149816 Review.
Cited by
-
Differences in HDL Remodeling during Healthy Pregnancy and Pregnancy with Cardiometabolic Complications.Antioxidants (Basel). 2024 Aug 3;13(8):948. doi: 10.3390/antiox13080948. Antioxidants (Basel). 2024. PMID: 39199194 Free PMC article.
-
Performance of early risk assessment tools to predict the later development of gestational diabetes.Eur J Clin Invest. 2021 Dec;51(12):e13630. doi: 10.1111/eci.13630. Epub 2021 Jun 18. Eur J Clin Invest. 2021. PMID: 34142723 Free PMC article.
-
Clinical Value of Circ-PNPT1 on Adverse Pregnancy Outcomes of Patients with Gestational Diabetes Mellitus.Endocr Metab Immune Disord Drug Targets. 2024;24(15):1835-1841. doi: 10.2174/1871530323666221229120303. Endocr Metab Immune Disord Drug Targets. 2024. PMID: 36582066
-
Placental Regulation of Energy Homeostasis During Human Pregnancy.Endocrinology. 2020 Jul 1;161(7):bqaa076. doi: 10.1210/endocr/bqaa076. Endocrinology. 2020. PMID: 32417921 Free PMC article. Review.
-
Study on the Relationship and Predictive Value of First-Trimester Pregnancy-Associated Plasma Protein-A, Maternal Factors, and Biochemical Parameters in Gestational Diabetes Mellitus: A Large Case-Control Study in Southern China Mothers.Diabetes Metab Syndr Obes. 2023 Apr 1;16:947-957. doi: 10.2147/DMSO.S398530. eCollection 2023. Diabetes Metab Syndr Obes. 2023. PMID: 37033400 Free PMC article.
References
-
- American Diabetes Association. Gestational diabetes mellitus. Diabetes Care. 2004;27:S88–90. - PubMed
-
- Ferrara A. Increasing prevalence of gestational diabetes mellitus: a public health perspective. Diabetes Care. 2007;30:S141–6. - PubMed
-
- Bellamy L, Casas JP, Hingorani AD, Williams D. Type 2 diabetes mellitus after gestational diabetes: a systematic review and meta-analysis. Lancet. 2009;373:1773–9. - PubMed
MeSH terms
Substances
Grants and funding
- HHSN275201000001Z/HD/NICHD NIH HHS/United States
- HHSN275200800003C/HD/NICHD NIH HHS/United States
- HHSN275201000009C/HD/NICHD NIH HHS/United States
- HHSN275200800014C/HD/NICHD NIH HHS/United States
- P30 ES005605/ES/NIEHS NIH HHS/United States
- HHSN275200800002I/HD/NICHD NIH HHS/United States
- HHSN275200800028C/HD/NICHD NIH HHS/United States
- HHSN275200800002C/HD/NICHD NIH HHS/United States
- HHSN275200800013C/HD/NICHD NIH HHS/United States
- HHSN275200800012C/HD/NICHD NIH HHS/United States
- HHSN275200800003I/HD/NICHD NIH HHS/United States
- HHSN275201000001G/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources

