Personalized axillary dissection: the number of excised lymph nodes of nodal-positive breast cancer patients has no significant impact on relapse-free and overall survival
- PMID: 28439713
- PMCID: PMC11818957
- DOI: 10.1007/s00432-017-2425-3
Personalized axillary dissection: the number of excised lymph nodes of nodal-positive breast cancer patients has no significant impact on relapse-free and overall survival
Abstract
Purpose: Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the staging of clinically node-negative breast cancer patients (BCP), demonstrating equivalent survival to ALND while resulting in reduced morbidity. ALND has remained the standard of care for the majority of BCP with clinical axillary metastases or metastases found on SLN biopsy. More recently, it is debated whether ALND could be avoided not only in SLN-negative BCP but also in selected SLN-positive disease or even in all patients. This analysis of pN+ BCP shows the impact of the number of excised lymph nodes on RFS and OAS adjusted by age, tumor size, intrinsic subtypes and adjuvant systemic therapy.
Methods: In this retrospective, multicenter cohort study, we investigated data from 2992 pN+ primary BCP recruited from 17 participating certified breast cancer centers in Germany between 2001 and 2008 within the BRENDA study group.
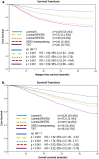
Results: The median number of excised lymph nodes was 17. The number of excised lymph nodes was neither significant for RFS (p = 0.085) nor for OAS (p = 0.285). Adjustments were made for age, tumor size and intrinsic subtypes. The most important significant parameters for RFS were intrinsic subtypes (p < 0.001) and tumor size (p < 0.001) and for OAS age (p < 0.001) and intrinsic subtypes (p < 0.001). There were no significant differences in RFS and OAS in any subgroup stratified by the number of excised lymph nodes. Only for T3/T4 tumors, there is a very small significant advantage of ALND for RFS but not for OAS. After adjusting in addition by guideline adherence of adjuvant systemic therapy (AST), intrinsic subtypes and guideline-adherent AST are the most important significant (p < 0.001) parameters for RFS and OAS.
Conclusions: The number of excised lymph nodes of pN+ BCP neither correlates with RFS nor with OAS. Survival of pN+ BCP is primarily determined by the biology and the guideline-adherent AST based on the corresponding intrinsic subtypes. These results support the omission of a radical ALND at least for pN+ patients scheduled for breast-conserving surgery (not mastectomy), provided they receive whole breast irradiation and guideline-adherent AST.
Keywords: Axillary lymph node dissection; Breast cancer; Lymph node; Sentinel node; Survival.
Conflict of interest statement
All authors declare that there are no potential conflicts of interest, including any financial, personal or other relationships with people or organizations that could inappropriately influence this work.
Figures


References
-
- Donker M, van Tienhoven G, Straver ME et al (2014) Radiotherapy or surgery of the axilla after a positive sentinel node in breast cancer (EORTC 10981-22023 AMAROS): a randomised, multicentre, open-label, phase 3 non-inferiority trial. Lancet Oncol 15:1303–1310. doi:10.1016/S1470-2045(14)70460-7 - PMC - PubMed
-
- Engel J, Emeny RT, Hölzel D (2012) Positive lymph nodes do not metastasize. Cancer Metastasis Rev 31:235–246. doi:10.1007/s10555-011-9343-7 - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

