The role of bile acids in nonalcoholic fatty liver disease and nonalcoholic steatohepatitis
- PMID: 28442273
- PMCID: PMC5812256
- DOI: 10.1016/j.mam.2017.04.004
The role of bile acids in nonalcoholic fatty liver disease and nonalcoholic steatohepatitis
Abstract
Nonalcoholic fatty liver disease is growing in prevalence worldwide. It is marked by the presence of macrosteatosis on liver histology but is often clinically asymptomatic. However, it can progress into nonalcoholic steatohepatitis which is a more severe form of liver disease characterized by inflammation and fibrosis. Further progression leads to cirrhosis, which predisposes patients to hepatocellular carcinoma or liver failure. The mechanism by which simple steatosis progresses to steatohepatitis is not entirely clear. However, multiple pathways have been proposed. A common link amongst many of these pathways is disruption of the homeostasis of bile acids. Other than aiding in the absorption of lipids and lipid-soluble vitamins, bile acids act as ligands. For example, they bind to farnesoid X receptor, which is critically involved in many of the pathways responsible for maintaining bile acid, glucose, and lipid homeostasis. Alterations to these pathways can lead to dysregulation of energy balance and increased inflammation and fibrosis. Repeated insults over time may be the key to development of steatohepatitis. For this reason, current drug therapies target aspects of these pathways to try to reduce and halt inflammation and fibrosis. This review will focus on the role of bile acids in these various pathways and how changes in these pathways may result in steatohepatitis. While there is no approved pharmaceutical treatment for either hepatic steatosis or steatohepatitis, this review will also touch upon the multitude of potential therapies.
Keywords: Bile acids; Enterohepatic circulation; Farnesoid X receptor (FXR); Gut-liver crosstalk; Nonalcoholic fatty liver disease (NAFLD); Nonalcoholic steatohepatitis (NASH).
Copyright © 2017 Elsevier Ltd. All rights reserved.
Figures
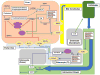
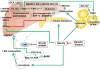
References
-
- Aguilar-Olivos NE, Carrillo-Cordova D, Oria-Hernandez J, Sanchez-Valle V, Ponciano-Rodriguez G, Ramirez-Jaramillo M, Chable-Montero F, Chavez-Tapia NC, Uribe M, Mendez-Sanchez N. The nuclear receptor FXR, but not LXR, up-regulates bile acid transporter expression in nonalcoholic fatty liver disease. Ann Hepatol. 2015;14(4):487–493. - PubMed
-
- Aranha MM, Cortez-Pinto H, Costa A, da Silva IB, Camilo ME, de Moura MC, Rodrigues CM. Bile acid levels are increased in the liver of patients with steatohepatitis. Eur J Gastroenterol Hepatol. 2008;20(6):519–525. - PubMed
-
- Bartram HP, Draenert R, Dusel G, Richter F, Liebscher E, Christl SU, Scheppach W, Kasper H. Effects of sodium selenite on deoxycholic acid-induced hyperproliferation of human colonic mucosa in short-term culture. Cancer Epidemiol Biomarkers Prev. 1998;7(12):1085–1089. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

