Non-surgical treatment of transverse deficiency in adults using Microimplant-assisted Rapid Palatal Expansion (MARPE)
- PMID: 28444019
- PMCID: PMC5398849
- DOI: 10.1590/2177-6709.22.1.110-125.sar
Non-surgical treatment of transverse deficiency in adults using Microimplant-assisted Rapid Palatal Expansion (MARPE)
Abstract
Introduction: Maxillary transverse deficiency is a highly prevalent malocclusion present in all age groups, from primary to permanent dentition. If not treated on time, it can aggravate and evolve to a more complex malocclusion, hindering facial growth and development. Aside from the occlusal consequences, the deficiency can bring about serious respiratory problems as well, due to the consequent nasal constriction usually associated. In growing patients, this condition can be easily handled with a conventional rapid palatal expansion. However, mature patients are frequently subjected to a more invasive procedure, the surgically-assisted rapid palatal expansion (SARPE). More recently, researches have demonstrated that it is possible to expand the maxilla in grown patients without performing osteotomies, but using microimplants anchorage instead. This novel technique is called microimplant-assisted rapid palatal expansion (MARPE).
Objective: The aim of the present article was to demonstrate and discuss a MARPE technique developed by Dr. Won Moon and colleagues at University of California - Los Angeles (UCLA).
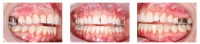
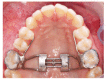
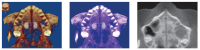
Methods: All laboratory and clinical steps needed for its correct execution are thoroughly described. For better comprehension, a mature patient case is reported, detailing all the treatment progress and results obtained.
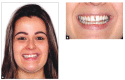
Conclusion: It was concluded that the demonstrated technique could be an interesting alternative to SARPE in the majority of non-growing patients with maxillary transverse deficiency. The present patient showed important occlusal and respiratory benefits following the procedure, without requiring any surgical intervention.
Introdução:: a deficiência transversa da maxila é uma má oclusão com alta prevalência em todas as faixas etárias, da dentição decídua à permanente. Se não for corrigida, pode agravar-se com o passar do tempo, prejudicando o crescimento e desenvolvimento facial. Além dos prejuízos oclusais, essa deficiência pode trazer problemas respiratórios também severos, devido à consequente constrição da cavidade nasal. Em pacientes em crescimento, a sua resolução é relativamente simples, por meio da expansão rápida convencional da maxila. Porém, os pacientes já maduros geralmente são encaminhados para um procedimento mais invasivo, a expansão rápida de maxila assistida cirurgicamente (SARPE). Mais recentemente, pesquisadores têm demonstrado que é possível executar a expansão palatal esquelética em pacientes adultos sem auxílio de osteotomias, mas sim com auxílio de mini-implantes. Essa técnica é denominada Microimplant-Assisted Rapid Palatal Expansion, ou MARPE.
Objetivo:: o objetivo do presente artigo é demonstrar e discutir uma das técnicas disponíveis de MARPE, desenvolvida por Won Moon e colaboradores, na University of California, Los Angeles (UCLA).
Métodos:: a técnica encontra-se detalhadamente descrita, com as etapas laboratoriais e clínicas que devem ser seguidas para sua correta execução. Para descrevê-la, é apresentado o caso clínico de uma paciente adulta, detalhando toda a sequência do tratamento e os resultados obtidos.
Conclusão:: a técnica apresentada pode ser uma alternativa não invasiva à SARPE na resolução da deficiência transversa de maxila, podendo ser empregada na maioria dos pacientes com crescimento facial finalizado. A paciente apresentada demonstrou benefícios significativos nos aspectos oclusal e respiratório, sem a necessidade de intervenção cirúrgica.
Conflict of interest statement
The authors report no commercial, proprietary or financial interest in the products or companies described in this article.
Patients displayed in this article previously approved the use of their facial and intraoral photographs.
Figures
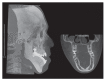
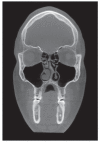
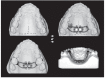
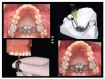




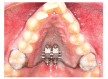


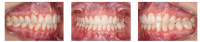
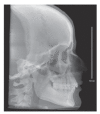
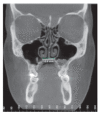
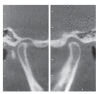
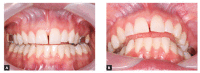
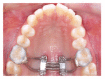

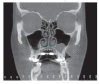
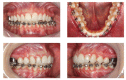
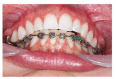
References
-
- Kurol J, Berglund L. Longitudinal study and cost-benefit analysis of the effect of early treatment of posterior cross-bites in the primary dentition. Eur J Orthod. 1992;14(3):173–179. - PubMed
-
- Silva OG, Filho, Santamaria M, Jr, Capelozza L., Filho Epidemiology of posterior crossbite in the primary dentition. J Clin Pediatr Dent. 2007;32(1):73–78. - PubMed
-
- Modeer T, Odenrick L, Lindner A. Sucking habits and their relation to posterior cross-bite in 4-year-old children. Scand J Dent Res. 1982;90(4):323–328. - PubMed
-
- Lione R, Franchi L, Huanca Ghislanzoni LT, Primozic J, Buongiorno M, Cozza P. Palatal surface and volume in mouth-breathing subjects evaluated with three-dimensional analysis of digital dental casts-a controlled study. Eur J Orthod. 2015;37(1):101–104. - PubMed
-
- Moss ML. The functional matrix hypothesis revisited. 1. The role of mechanotransduction. Am J Orthod Dentofacial Orthop. 1997 Jul;112(1):8–11. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

