Serelaxin treatment promotes adaptive hypertrophy but does not prevent heart failure in experimental peripartum cardiomyopathy
- PMID: 28453725
- PMCID: PMC5412020
- DOI: 10.1093/cvr/cvw245
Serelaxin treatment promotes adaptive hypertrophy but does not prevent heart failure in experimental peripartum cardiomyopathy
Abstract
Aims: Peripartum cardiomyopathy (PPCM) is a systolic left ventricular dysfunction developing in the peripartum phase in previously healthy women. Relaxin-2 is a pregnancy hormone with potential beneficial effects in heart failure patients. We evaluated Relaxin-2 as a potential diagnostic marker and/or a therapeutic agent in PPCM.
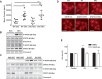
Methods and results: In healthy peripartum women, serum Relaxin-2 levels (measured by ELISA in the second half of pregnancy) were elevated showing a decreasing trend in the first postpartum week and returned to non-pregnant levels thereafter. In PPCM patients diagnosed in the first postpartum week, serum Relaxin-2 levels were lower compared to healthy postpartum stage-matched controls. In PPCM patients diagnosed later (0.5-10 months postpartum) Relaxin-2 levels were in the range of non-pregnant controls and not different from healthy postpartum stage-matched controls. In mice, serum Relaxin-1 (functional equivalent of human Relaxin-2) was increased late in pregnancy and rapidly cleared in the first postpartum week. In mice with PPCM due to a cardiomyocyte-specific knockout of STAT3 (CKO) neither low nor high dose of recombinant Relaxin-2 (serelaxin, sRlx-LD: 30 µg/kg/day; sRlx-HD: 300 µg/kg/day) affected cardiac fibrosis, inflammation and heart failure but sRlx-HD increased capillary/cardiomyocyte ratio. sRlx-HD significantly increased heart/body weight ratio and cardiomyocyte cross-sectional area in postpartum CKO and wild-type mice without changing the foetal gene expression program (ANP or β-MHC). sRlx-HD augmented plasma Prolactin levels in both genotypes, which induced cardiac activation of STAT5. In vitro analyses showed that Prolactin induces cardiomyocyte hypertrophy via activation of STAT5.
Conclusion: Although Relaxin-2 levels seemed lower in PPCM patients diagnosed early postpartum, we observed a high pregnancy-related variance of serum Relaxin-2 levels peripartum making it unsuitable as a biomarker for this condition. Supplementation with sRlx may contribute to angiogenesis and compensatory hypertrophy in the diseased heart, but the effects are not sufficient to prevent heart failure in an experimental PPCM model.
Keywords: Biomarker; Heart failure; Hypertrophy; Peripartum cardiomyopathy; Relaxin; STAT3; STAT5; Serelaxin.
© The Author 2017. Published by Oxford University Press on behalf of the European Society of Cardiology.
Figures





Comment in
-
Relaxin: reproductive safeguard turned cardiac?Cardiovasc Res. 2017 May 1;113(6):553-555. doi: 10.1093/cvr/cvx059. Cardiovasc Res. 2017. PMID: 28453739 No abstract available.
References
-
- Bathgate RA, Halls ML, van der Westhuizen ET, Callander GE, Kocan M, Summers RJ.. Relaxin family peptides and their receptors. Physiol Rev 2013;93:405–480. - PubMed
-
- Conrad KP, Shroff SG.. Effects of relaxin on arterial dilation, remodeling, and mechanical properties. Curr Hypertens Rep 2011;13:409–420. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

