Classification of full-thickness rotator cuff lesions: a review
- PMID: 28461921
- PMCID: PMC5367545
- DOI: 10.1302/2058-5241.1.160005
Classification of full-thickness rotator cuff lesions: a review
Abstract
Rotator cuff lesions (RCL) have considerable variability in location, tear pattern, functional impairment, and repairability.Historical classifications for differentiating these lesions have been based upon factors such as the size and shape of the tear, and the degree of atrophy and fatty infiltration. Additional recent descriptions include bipolar rotator cuff insufficiency, 'Fosbury flop tears', and musculotendinous lesions.Recommended treatment is based on the location of the lesion, patient factors and associated pathology, and often includes personal experience and data from case series. Development of a more comprehensive classification which integrates historical and newer descriptions of RCLs may help to guide treatment further. Cite this article: Lädermann A, Burkhart SS, Hoffmeyer P, et al. Classification of full thickness rotator cuff lesions: a review. EFORT Open Rev 2016;1:420-430. DOI: 10.1302/2058-5241.1.160005.
Keywords: classification; massive rotator cuff tear; repair; repairable and non-repairable; rotator cuff lesion; shoulder imaging; tear pattern.
Conflict of interest statement
Conflict of Interest: One or more of the authors has declared the following potential conflict of interest or source of funding: S.S.B. is a consultant for and receives royalties from Arthrex, Inc. (Naples, Florida). P.J.D. is a consultant for and receives research support from Arthrex, Inc.
Figures
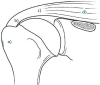
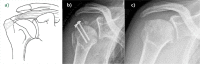
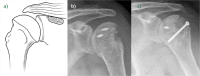
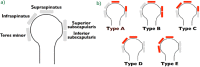
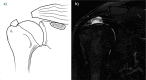
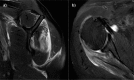
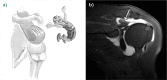
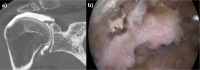
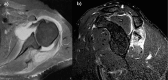
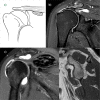
References
-
- Court-Brown CM, Garg A, McQueen MM. The epidemiology of proximal humeral fractures. Acta Orthop Scand 2001;72:365-371. - PubMed
-
- Neer CS., II Displaced proximal humeral fractures. I. Classification and evaluation. J Bone Joint Surg [Am] 1970;52-A:1077-1089. - PubMed
-
- Bono CM, Renard R, Levine RG, Levy AS. Effect of displacement of fractures of the greater tuberosity on the mechanics of the shoulder. J Bone Joint Surg [Br] 2001;83-B:1056-1062. - PubMed
-
- Lädermann A, Denard PJ, Burkhart SS. Arthroscopic management of proximal humerus malunion with tuberoplasty and rotator cuff retensioning. Arthroscopy 2012;28:1220-1229. - PubMed
-
- Greiner S, Scheibel M. Bony avulsions of the rotator cuff: arthroscopic concepts. Der Orthopade 2011;40:21-4,26-30. [Article in German]. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

