Management of ankle fractures in the elderly
- PMID: 28461954
- PMCID: PMC5367590
- DOI: 10.1302/2058-5241.1.000023
Management of ankle fractures in the elderly
Abstract
The incidence and severity of ankle fractures in elderly patients is increasing steadily. These injuries are challenging to treat and prone to complications.Individual fracture treatment is tailored depending on bone quality, skin conditions, comorbidities, and functional demand of the patient. This article provides a review of current techniques to obtain stable fixation despite poor bone quality. To avoid complications, it is imperative to consider and treat comorbidities such as diabetes and osteoporosis.In the absence of severe systemic comorbidities, the results after open reduction and internal fixation of malleolar fractures in patients above and below 60 years of age are nearly identical, while nonoperative treatment of unstable fractures leads to significantly inferior outcomes. Therefore, the general indications for surgery in elderly patients should not differ from those in younger patients.However, it is essential to detect severe conditions such as Charcot neuro-osteoarthropathy because these require a completely different treatment regime, and standard internal fixation will invariably fail in these patients. Cite this article: Rammelt S. Management of ankle fractures in the elderly. EFORT Open Rev 2016;1:239-246. DOI: 10.1302/2058-5241.1.000023.
Keywords: Charcot neuroarthropathy; complications; diabetes; dislocation; osteoporosis; posterior tibia; syndesmosis.
Conflict of interest statement
Conflict of Interest: The author is a member of the AOTrauma Foot & Ankle Expert Group and the AOTrauma Foot & Ankle Education Task Force. As such he is involved in implant development for Trauma Surgery and receives travel support from AOTrauma for Meetings and Courses. The author receives research grants for investigations on biomaterials and bone healing from the Deutsche Forschungsgemeinschaft (German Research Association, DFG).
Figures
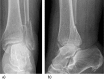




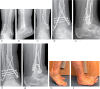
Similar articles
-
Current management of trimalleolar ankle fractures.EFORT Open Rev. 2021 Aug 10;6(8):692-703. doi: 10.1302/2058-5241.6.200138. eCollection 2021 Aug. EFORT Open Rev. 2021. PMID: 34532077 Free PMC article. Review.
-
Repair of syndesmosis injury in ankle fractures: Current state of the art.EFORT Open Rev. 2018 Jan 25;3(1):24-29. doi: 10.1302/2058-5241.3.170017. eCollection 2018 Jan. EFORT Open Rev. 2018. PMID: 29657842 Free PMC article.
-
Ankle fractures in diabetic patients.EFORT Open Rev. 2020 Sep 10;5(8):457-463. doi: 10.1302/2058-5241.5.200025. eCollection 2020 Aug. EFORT Open Rev. 2020. PMID: 32953131 Free PMC article. Review.
-
[One of the pitfalls in the surgical treatment of maisonneuve fractures: a case report].Beijing Da Xue Xue Bao Yi Xue Ban. 2017 Apr 18;49(2):354-356. Beijing Da Xue Xue Bao Yi Xue Ban. 2017. PMID: 28416851 Chinese.
-
Bicortical fixation of medial malleolar fractures: a review of 23 cases at risk for complicated bone healing.J Foot Ankle Surg. 2012 Jan-Feb;51(1):39-44. doi: 10.1053/j.jfas.2011.09.007. J Foot Ankle Surg. 2012. PMID: 22196457
Cited by
-
Short Term Complications in Geriatric Ankle Fractures Using a Protocolized Approach to Surgical Treatment: Is Early Weight Bearing Safe?Iowa Orthop J. 2020;40(1):159-165. Iowa Orthop J. 2020. PMID: 32742225 Free PMC article.
-
Ankle fractures in Finland: 118,929 operatively treated between 1987 and 2019.Acta Orthop. 2022 Feb 11;93:327-333. doi: 10.2340/17453674.2022.2071. Acta Orthop. 2022. PMID: 35147707 Free PMC article.
-
An overview on the treatment and outcome factors of ankle fractures in elderly men and women aged 80 and over: a systematic review.Arch Orthop Trauma Surg. 2022 Nov;142(11):3311-3325. doi: 10.1007/s00402-021-04161-y. Epub 2021 Sep 21. Arch Orthop Trauma Surg. 2022. PMID: 34546421 Free PMC article.
-
Retrograde tibiotalocalcaneal nailing for the treatment of acute ankle fractures in the elderly: a systematic review and meta-analysis.EFORT Open Rev. 2022 Sep 19;7(9):628-643. doi: 10.1530/EOR-22-0017. EFORT Open Rev. 2022. PMID: 36125009 Free PMC article. Review.
-
Osteoporotic ankle fractures: A narrative review of management options.J Clin Orthop Trauma. 2020 May-Jun;11(3):380-387. doi: 10.1016/j.jcot.2019.10.010. Epub 2019 Nov 4. J Clin Orthop Trauma. 2020. PMID: 32405196 Free PMC article. Review.
References
-
- Kannus P, Palvanen M, Niemi S, Parkkari J, Jarvinen M. Increasing number and incidence of low-trauma ankle fractures in elderly people: Finnish statistics during 1970-2000 and projections for the future. Bone 2002;31:430-3. - PubMed
-
- Rammelt S, Heim D, Hofbauer LC, Grass R, Zwipp H. Problems and controversies in the treatment of ankle fractures. Unfallchirurg 2011;114:847-60. - PubMed
-
- Court-Brown CM, Biant LC, Clement ND, Bugler KE, Duckworth AD, McQueen MM. Open fractures in the elderly. The importance of skin ageing. Injury 2015;46:189-94. - PubMed
-
- Ali MS, McLaren CA, Rouholamin E, O’Connor BT. Ankle fractures in the elderly: nonoperative or operative treatment. J Orthop Trauma 1987;1:275-80. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

