Minimally invasive distal pancreatectomy for PNETs: laparoscopic or robotic approach?
- PMID: 28477012
- PMCID: PMC5464919
- DOI: 10.18632/oncotarget.17513
Minimally invasive distal pancreatectomy for PNETs: laparoscopic or robotic approach?
Abstract
Background: The most effective and radical treatment for pancreatic neuroendocrine tumors (PNETs) is surgical resection. Minimally invasive surgery has been increasingly used in pancreatectomy. Initial results in robotic distal pancreatectomy (RDP) have been encouraging. Nonetheless, data comparing outcomes of RDP with those of laparoscopic distal pancreatectomy (LDP) in treating PNETs are rare. The aim of this study was to compare the safety and efficacy of RDP and LDP for PNETs.
Methods: From September 2010 to January 2017, operative parameters and perioperative outcomes in an initial experience with 43 consecutive patients undergoing RDP were collected and compared with those in 31 patients undergoing LDP.
Results: Patients undergoing RDP and LDP demonstrated equivalent age, sex, ASA score, tumor location and tumor size. Operating time, length of resected pancreas, postoperative length of hospital stay and rates of conversion to open, pancreatic fistula, transfusion and reoperation were not statistically different. Patients in the RDP group were associated with significantly higher overall (79.1 vs. 48.4 %, P = 0.006) and Kimura spleen preservation rates (72.1 vs. 16.1%, P < 0.001) and had reduced risk of excessive blood loss (50 vs. 200mL, P < 0.001). Oncological outcomes in this series were superior for the RDP group with more lymph node harvest for G2 and G3 PNETs (3.5 vs. 2, P = 0.034).
Conclusions: Both RDP and LDP are efficacious and safe methods in treating PNETs located in the body or tail of pancreas. Robotic approach offers advantages with less intraoperative blood loss, higher spleen preservation rate and more lymph node harvest. It may be sensible to choose RDP for patients who fit indications for scheduled spleen preservation.
Keywords: PNETs; distal pancreatectomy; laparoscopic surgery; robotic surgery.
Conflict of interest statement
There are no conflicts to disclose.
Figures



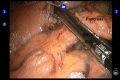

References
-
- Marx S, Spiegel AM, Skarulis MC, Doppmann JL, Collins FS, Liotta LA. Multiple endocrine neoplasia type 1: clinical and genetic topics. Ann Intern Med. 1998;129:484–494. - PubMed
-
- Milan SA, Yeo CJ. Neuroendocrine tumors of the pancreas. Curr Opin Oncol. 2012;24:46–55. - PubMed
-
- Zikusoka MN, Kidd M, Eick G, Latich I, Modlin IM. The molecular genetics of gastroenteropancreatic neuroendocrine tumors. Cancer. 2005;104:2292–309. Review. - PubMed
-
- Srirajaskanthan R, Toumpanakis C, Karpathakis A, Marelli L, Quigley AM, Dusmet M, Meyer T, Caplin ME. Surgical management and palliative treatment in bronchial neuroendocrine tumours: a clinical study of 45 patients. Lung Cancer. 2009;65:68–73. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

