Rapid development of metastatic pulmonary calcifications in primary hyperparathyroidism: a case report and literature review
- PMID: 28482911
- PMCID: PMC5423015
- DOI: 10.1186/s13000-017-0628-1
Rapid development of metastatic pulmonary calcifications in primary hyperparathyroidism: a case report and literature review
Abstract
Background: Metastatic pulmonary calcification (MPC) is rarely reported in primary hyperparathyroidism, especially MPC develops quickly. We report such a case here with a literature review.
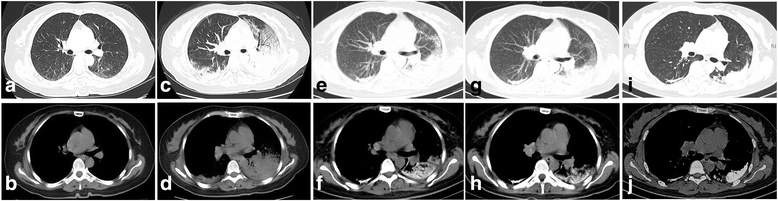
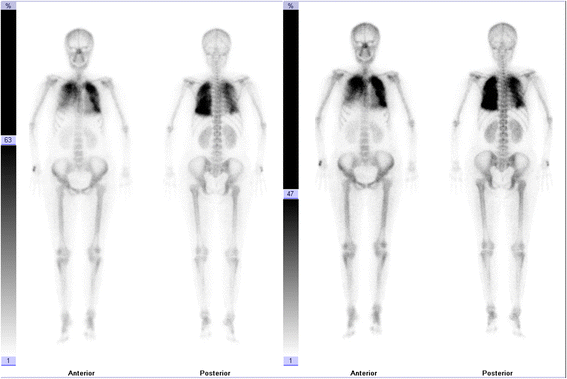
Case presentation: A 41-year-old woman presented with cough and dyspnea. Data from clinical, radiological, pathological, technetium (99mTc)-methylene diphosphonate (MDP) bone scintillation imaging, and 99mTc-methoxy isobutyl isonitrile (MIBI) thyroid imaging were studied. 99mTc-MIBI thyroid imaging indicated hyperparathyroidism. Chest computed tomography (CT) scans showed rapidly progressive bilateral pulmonary multiple high-density shadows with mass consolidation and exudation in only five days. 99mTc-MDP bone scintillation imaging indicated bilateral pulmonary calcifications. CT-guided lung biopsy showed multifocal irregularities of calcium deposition and calcified bodies in the pulmonary interstitium. The patient showed gradually clinical and radiological improvement after surgical removal of the parathyroid adenoma.
Conclusion: Rapidly progressive MPC tends to be misdiagnosed as many primary pulmonary diseases. 99mTc-MDP bone scintillation imaging and pulmonary biopsy could be performed to differentiate metastatic pulmonary calcification from other diseases. Surgical resection of the parathyroid gland is helpful for treatment of MPC in patients with primary hyperparathyroidism and is regularly recommended.
Keywords: 99mTc-MDP bone scintillation imaging; 99mTc-MIBI thyroid imaging; Metastatic pulmonary calcification; Primary hyperparathyroidism.
Figures


Similar articles
-
Correlation between serum calcium levels and dual-phase (99m)Tc-sestamibi parathyroid scintigraphy in primary hyperparathyroidism.Clin Physiol Funct Imaging. 2012 Jan;32(1):19-24. doi: 10.1111/j.1475-097X.2011.01048.x. Epub 2011 Aug 24. Clin Physiol Funct Imaging. 2012. PMID: 22136277
-
Multiple brown tumors in primary hyperparathyroidism caused by an adenoma mimicking metastatic bone disease with false positive results on computed tomography and Tc-99m sestamibi imaging: MR findings.Endocr J. 2007 Apr;54(2):205-10. doi: 10.1507/endocrj.k05-175. Epub 2007 Jan 22. Endocr J. 2007. PMID: 17237612
-
Comparison of 99mTc-sestamibi and 11C-methionine PET/CT in the localization of parathyroid adenomas in primary hyperparathyroidism.Rev Esp Med Nucl Imagen Mol. 2014 Mar-Apr;33(2):93-8. doi: 10.1016/j.remn.2013.08.002. Epub 2013 Oct 11. Rev Esp Med Nucl Imagen Mol. 2014. PMID: 24125595
-
Unusual case of solitary functioning bone metastasis from a "parathyroid adenoma": imagiologic diagnosis and treatment with percutaneous vertebroplasty--case report and literature review.J Clin Endocrinol Metab. 2013 Sep;98(9):3555-61. doi: 10.1210/jc.2013-2014. Epub 2013 Jul 16. J Clin Endocrinol Metab. 2013. PMID: 23861459 Review.
-
[Primary hyperparathyroidism due to an intrathoracic parathyroid adenoma. - A case report and review of the literature].Laeknabladid. 2010 Jul-Aug;96(7-8):469-72. doi: 10.17992/lbl.2010.0708.307. Laeknabladid. 2010. PMID: 20601747 Review. Icelandic.
Cited by
-
Acute respiratory distress syndrome driven by severe hypercalcemia and acute kidney injury: A case report and literature review of a rare, life-threatening complication.Clin Nephrol Case Stud. 2022 Jan 24;10:21-27. doi: 10.5414/CNCS110464. eCollection 2022. Clin Nephrol Case Stud. 2022. PMID: 35106272 Free PMC article.
-
Primary hyperparathyroidism characterized by diffuse homogeneous metastatic pulmonary calcification: A case report.Medicine (Baltimore). 2018 Nov;97(44):e13107. doi: 10.1097/MD.0000000000013107. Medicine (Baltimore). 2018. PMID: 30383698 Free PMC article.
-
Discovery of primary hyperparathyroidism following an endoscopic resection of the prostate: case report.J Surg Case Rep. 2022 May 27;2022(5):rjac247. doi: 10.1093/jscr/rjac247. eCollection 2022 May. J Surg Case Rep. 2022. PMID: 35665381 Free PMC article.
-
Pulmonary alveolar microlithiasis.Eur Respir Rev. 2020 Nov 27;29(158):200024. doi: 10.1183/16000617.0024-2020. Print 2020 Dec 31. Eur Respir Rev. 2020. PMID: 33246992 Free PMC article. Review.
-
An unusual cause of pulmonary calcification.BMJ Case Rep. 2019 Jun 18;12(6):e229725. doi: 10.1136/bcr-2019-229725. BMJ Case Rep. 2019. PMID: 31217215 Free PMC article.
References
-
- Shindo M, Lee JA, Lubitz CC, McCoy KL, Orloff LA, Tufano RP, et al. The Changing Landscape of Primary, Secondary, and Tertiary Hyperparathyroidism: Highlights from the American College of Surgeons Panel, “What’s New for the Surgeon Caring for Patients with Hyperparathyroidism”. J Am Coll Surg. 2016;222(6):1240–1250. doi: 10.1016/j.jamcollsurg.2016.02.024. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

