Inequity in organ allocation for patients awaiting liver transplantation: Rationale for uncapping the model for end-stage liver disease
- PMID: 28483678
- PMCID: PMC7735955
- DOI: 10.1016/j.jhep.2017.04.022
Inequity in organ allocation for patients awaiting liver transplantation: Rationale for uncapping the model for end-stage liver disease
Abstract
Background & aim: The goal of organ allocation is to distribute a scarce resource equitably to the sickest patients. In the United States, the Model for End-stage Liver Disease (MELD) is used to allocate livers for transplantation. Patients with greater MELD scores are at greater risk of death on the waitlist and are prioritized for liver transplant (LT). The MELD is capped at 40 however, and patients with calculated MELD scores >40 are not prioritized despite increased mortality. We aimed to evaluate waitlist and post-transplant survival stratified by MELD to determine outcomes in patients with MELD >40.
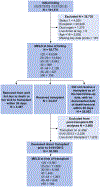
Methods: Using United Network for Organ Sharing data, we identified patients listed for LT from February 2002 through to December 2012. Waitlist candidates with MELD ⩾40 were followed for 30days or until the earliest occurrence of death or transplant.
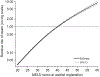
Results: Of 65,776 waitlisted patients, 3.3% had MELD ⩾40 at registration, and an additional 7.3% had MELD scores increase to ⩾40 after waitlist registration. A total of 30,369 (46.2%) underwent LT, of which 2,615 (8.6%) had MELD ⩾40 at transplant. Compared to MELD 40, the hazard ratio of death within 30days of registration was 1.4 (95% CI 1.2-1.6) for patients with MELD 41-44, 2.6 (95% CI 2.1-3.1) for MELD 45-49, and 5.0 (95% CI 4.1-6.1) for MELD ⩾50. There was no difference in 1- and 3-year survival for patients transplanted with MELD >40 compared to MELD=40. A survival benefit associated with LT was seen as MELD increased above 40.
Conclusions: Patients with MELD >40 have significantly greater waitlist mortality but comparable post-transplant outcomes to patients with MELD=40 and, therefore, should be given priority for LT. Uncapping the MELD will allow more equitable organ distribution aligned with the principle of prioritizing patients most in need. Lay summary: In the United States (US), organs for liver transplantation are allocated by an objective scoring system called the Model for End-stage Liver Disease (MELD), which aims to prioritize the sickest patients for transplant. The greater the MELD score, the greater the mortality without liver transplant. The MELD score, however, is artificially capped at 40 and thus actually disadvantages the sickest patients with end-stage liver disease. Analysis of the data advocates uncapping the MELD score to appropriately prioritize the patients most in need of a liver transplant.
Keywords: Liver allocation; Liver transplantation; Model for end-stage liver disease (MELD); Post-transplant outcome; Regional disparity; Share 35; Waitlist mortality.
Copyright © 2017 European Association for the Study of the Liver. Published by Elsevier B.V. All rights reserved.
Conflict of interest statement
Conflict of interest
The authors who have taken part in this study declared that they do not have anything to disclose regarding funding or conflict of interest with respect to this manuscript.
Please refer to the accompanying ICMJE disclosure forms for further details.
Figures

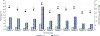
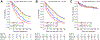
Comment in
-
Necessity of time series analysis and effects of direct-acting antivirals on HCV patients awaiting liver transplantation.J Hepatol. 2018 Mar;68(3):628-629. doi: 10.1016/j.jhep.2017.07.039. Epub 2017 Sep 20. J Hepatol. 2018. PMID: 28939131 No abstract available.
References
-
- Hussong S. Administrative developments: DHHS issues organ allocation final rule. J Law Med Ethics 1999;27:380–382. - PubMed
-
- Freeman RB Jr, Wiesner RH, Roberts JP, McDiarmid S, Dykstra DM, Merion RM. Improving liver allocation: MELD and PELD. Am J Transplant 2004;4:114–131. - PubMed
-
- Freeman RB Jr, Edwards EB. Liver transplant waiting time does not correlate with waiting list mortality: implications for liver allocation policy. Liver Transpl 2000;6:543–552. - PubMed
-
- Wiesner RH, McDiarmid SV, Kamath PS, Edwards EB, Malinchoc M, Kremers WK, et al. MELD and PELD: application of survival models to liver allocation. Liver Transpl 2001;7:567–580. - PubMed
-
- Freeman RB Jr, Wiesner RH, Harper A, McDiarmid SV, Lake J, Edwards E, et al. The new liver allocation system: moving toward evidence-based transplantation policy. Liver Transpl 2002;8:851–858. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

