Advanced Age as a Predictor of Survival and Weaning in Venoarterial Extracorporeal Oxygenation: A Retrospective Observational Study
- PMID: 28484710
- PMCID: PMC5397620
- DOI: 10.1155/2017/3505784
Advanced Age as a Predictor of Survival and Weaning in Venoarterial Extracorporeal Oxygenation: A Retrospective Observational Study
Abstract
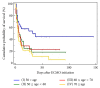
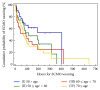
Background. In most reports on ECMO treatment, advanced age is classified as a contraindication to VA ECMO. We attempted to investigate whether advanced age would be a main risk factor deciding VA ECMO application and performing VA ECMO support. We determined whether advanced age should be regarded as an absolute or relative contraindication to VA ECMO and could affect weaning and survival rates of VA ECMO patients. Methods. VA ECMO was performed on 135 adult patients with primary cardiogenic shock between January 2010 and December 2014. Successful weaning was defined as weaning from ECMO followed by survival for more than 48 hours. Results. Among the 135 patients, 35 survived and were discharged uneventfully, and the remaining 100 did not survive. There were significant differences in survival between age groups, and older age showed a lower survival rate with statistical significance (P = .01). By multivariate logistic regression analysis, age was not significantly associated with in-hospital mortality (P = .83) and was not significantly associated with VA ECMO weaning (P = .11). Conclusions. Advanced age is an undeniable risk factor for VA ECMO; however, patients of advanced age should not be excluded from the chance of recovery after VA ECMO treatment.
Figures
Similar articles
-
Veno-arterial ECMO ventricular assistance as a direct bridge to heart transplant: A single center experience in a low-middle income country.Clin Transplant. 2024 Jun;38(6):e15334. doi: 10.1111/ctr.15334. Clin Transplant. 2024. PMID: 38864350
-
Predictors of Mortality in Venoarterial Extracorporeal Membrane Oxygenation Regardless of Early Left Ventricular Unloading: A National Experience.J Cardiothorac Vasc Anesth. 2025 Apr;39(4):949-956. doi: 10.1053/j.jvca.2025.01.013. Epub 2025 Jan 13. J Cardiothorac Vasc Anesth. 2025. PMID: 39884906
-
The Effectiveness of Levosimendan on Veno-Arterial Extracorporeal Membrane Oxygenation Management and Outcome: A Systematic Review and Meta-Analysis.J Cardiothorac Vasc Anesth. 2021 Aug;35(8):2483-2495. doi: 10.1053/j.jvca.2021.01.019. Epub 2021 Jan 16. J Cardiothorac Vasc Anesth. 2021. PMID: 33583718
-
Unifying Weaning Success Criteria to Bridge the Extracorporeal Membrane Oxygenation Gap: Variations in Determinants Based on Definitions of Successful Weaning.J Cardiothorac Vasc Anesth. 2025 Aug;39(8):2102-2110. doi: 10.1053/j.jvca.2025.05.015. Epub 2025 May 13. J Cardiothorac Vasc Anesth. 2025. PMID: 40450395
-
Extra-corporeal membrane oxygenation for refractory cardiogenic shock after adult cardiac surgery: a systematic review and meta-analysis.J Cardiothorac Surg. 2017 Jul 17;12(1):55. doi: 10.1186/s13019-017-0618-0. J Cardiothorac Surg. 2017. PMID: 28716039 Free PMC article.
Cited by
-
Patients with fulminant myocarditis supported with veno-arterial extracorporeal membrane oxygenation: a systematic review and meta-analysis of short-term mortality and impact of risk factors.Heart Fail Rev. 2023 Mar;28(2):347-357. doi: 10.1007/s10741-022-10277-z. Epub 2022 Oct 7. Heart Fail Rev. 2023. PMID: 36205853 Free PMC article.
-
Can we predict patient outcome before extracorporeal membrane oxygenation for refractory cardiac arrest?Scand J Trauma Resusc Emerg Med. 2020 Jun 23;28(1):58. doi: 10.1186/s13049-020-00753-6. Scand J Trauma Resusc Emerg Med. 2020. PMID: 32576294 Free PMC article.
-
Multiparameters associated to successful weaning from VA ECMO in adult patients with cardiogenic shock or cardiac arrest: Systematic review and meta-analysis.Ann Card Anaesth. 2023 Jan-Mar;26(1):4-11. doi: 10.4103/aca.aca_79_22. Ann Card Anaesth. 2023. PMID: 36722581 Free PMC article.
-
The ABCDE approach to difficult weaning from venoarterial extracorporeal membrane oxygenation.Crit Care. 2022 Jul 15;26(1):216. doi: 10.1186/s13054-022-04089-8. Crit Care. 2022. PMID: 35841052 Free PMC article. Review.
-
Impact of levosimendan on weaning from peripheral venoarterial extracorporeal membrane oxygenation in intensive care unit.Ann Intensive Care. 2019 Feb 1;9(1):24. doi: 10.1186/s13613-019-0503-1. Ann Intensive Care. 2019. PMID: 30707314 Free PMC article.
References
-
- Gibbon J. H., Jr. Application of a mechanical heart and lung apparatus to cardiac surgery. Minnesota medicine. 1954;37(3):171–185. - PubMed
-
- Dorson W., Baker E., Cohen M. L., et al. A perfusion system for infants. Transactions—American Society for Artificial Internal Organs. 1969;15(1):155–160. - PubMed
-
- White J. J., Andrews H. G., Risemberg H., Mazur D., Haller J. A., Jr. Prolonged respiratory support in newborn infants with a membrane oxygenator. Surgery. 1971;70(2):288–296. - PubMed
-
- Shekar K., Mullany D. V., Thomson B., Ziegenfuss M., Platts D. G., Fraser J. F. Extracorporeal life support devices and strategies for management of acute cardiorespiratory failure in adult patients: a comprehensive review. Critical Care. 2014;18(3):p. 219. doi: 10.1186/cc13865. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

