Association of a Primary Stroke Center Protocol for Suspected Stroke by Large-Vessel Occlusion With Efficiency of Care and Patient Outcomes
- PMID: 28492918
- PMCID: PMC5710532
- DOI: 10.1001/jamaneurol.2017.0477
Association of a Primary Stroke Center Protocol for Suspected Stroke by Large-Vessel Occlusion With Efficiency of Care and Patient Outcomes
Abstract
Importance: While prehospital triage to the closest comprehensive stroke center (CSC) may improve the delivery of care for patients with suspected emergent large-vessel occlusion (ELVO), efficient systems of care must also exist for patients with ELVO who first present to a primary stroke center (PSC).
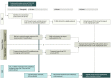
Objective: To describe the association of a PSC protocol focused on 3 key steps (early CSC notification based on clinical severity, vessel imaging at the PSC, and cloud-based image sharing) with the efficiency of care and the outcomes of patients with suspected ELVO who first present to a PSC.
Design, setting, and participants: In this retrospective cohort study, 14 regional PSCs unfamiliar with the management of patients with ELVO were instructed on the use of the following protocol for patients presenting with a Los Angeles Motor Scale score 4 or higher: (1) notify the CSC on arrival, (2) perform computed tomographic angiography concurrently with noncontract computed tomography of the brain and within 30 minutes of arrival, and (3) share imaging data with the CSC using a cloud-based platform. A total of 101 patients were transferred from regional PSCs to the CSC between July 1, 2015, and May 31, 2016, and received mechanical thrombectomy for acute ischemic stroke. The CSC serves approximately 1.7 million people and partners with 14 PSCs located between 6.4 and 73.6 km away. All consecutive patients with internal carotid artery or middle cerebral artery occlusions transferred over an 11-month period were reviewed, and they were divided into 2 groups based on whether the PSC protocol was partially or fully executed.
Main outcomes and measures: The primary outcomes were efficiency measures including time from PSC door in to PSC door out, time from PSC door to CSC groin puncture, and 90-day modified Rankin Scale score (range, 0-6; scores of 0-2 indicate a good outcome).
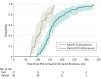
Results: Although 101 patients were transferred, only 70 patients met the inclusion criteria during the study period. The protocol was partially executed for 48 patients (68.6%) (mean age, 77 years [interquartile range, 65-84 years]; 22 of the 48 patients [45.0%] were women) and fully executed for 22 patients (31.4%) (mean age, 76 years [interquartile range, 59-86 years]; 13 of the 22 patients [59.1%] were women). When fully executed, the protocol was associated with a reduction in the median time for PSC arrival to CSC groin puncture (from 151 minutes [95% CI, 141-166 minutes] to 111 minutes [95% CI, 88-130 minutes]; P < .001). This was primarily related to an improvement in the time from PSC door in to door out that reduced from a median time of 104 minutes (95% CI, 82-112 minutes) to a median time of 64 minutes (95% CI, 51-71.0 minutes) (P < .001). When the protocol was fully executed, patients were twice as likely to have a favorable outcome (50% vs 25%, P < .04).
Conclusions and relevance: When fully implemented, a standardized protocol at PSCs for patients with suspected ELVO consisting of early CSC notification, computed tomographic angiography on arrival to the PSC, and cloud-based image sharing is associated with a reduction in time to groin puncture and improved outcomes.
Conflict of interest statement
Figures

Comment in
- doi: 10.1001/jamaneurol.2017.0324
Similar articles
-
Deconstruction of Interhospital Transfer Workflow in Large Vessel Occlusion: Real-World Data in the Thrombectomy Era.Stroke. 2017 Jul;48(7):1976-1979. doi: 10.1161/STROKEAHA.117.017235. Epub 2017 May 16. Stroke. 2017. PMID: 28512170
-
Door-in-Door-Out Time at Primary Stroke Centers May Predict Outcome for Emergent Large Vessel Occlusion Patients.Stroke. 2018 Dec;49(12):2969-2974. doi: 10.1161/STROKEAHA.118.021936. Stroke. 2018. PMID: 30571428
-
Two Paradigms for Endovascular Thrombectomy After Intravenous Thrombolysis for Acute Ischemic Stroke.JAMA Neurol. 2017 May 1;74(5):549-556. doi: 10.1001/jamaneurol.2016.5823. JAMA Neurol. 2017. PMID: 28319240 Free PMC article.
-
Intra-arterial treatment of patients with acute ischemic stroke and internal carotid artery occlusion: a literature review.J Neurointerv Surg. 2015 Jan;7(1):8-15. doi: 10.1136/neurintsurg-2013-011004. Epub 2014 Jan 2. J Neurointerv Surg. 2015. PMID: 24385555 Review.
-
The Safety and Efficacy of Mechanical Thrombectomy in Posterior VS. Anterior Emergent Large Vessel Occlusion: A Systematic Review and Meta-analysis.J Stroke Cerebrovasc Dis. 2020 Mar;29(3):104545. doi: 10.1016/j.jstrokecerebrovasdis.2019.104545. Epub 2019 Dec 24. J Stroke Cerebrovasc Dis. 2020. PMID: 31879134
Cited by
-
Trauma Communications Center Coordinated Severity-Based Stroke Triage: Protocol of a Hybrid Type 1 Effectiveness-Implementation Study.Front Neurol. 2021 Dec 6;12:788273. doi: 10.3389/fneur.2021.788273. eCollection 2021. Front Neurol. 2021. PMID: 34938265 Free PMC article.
-
Effect of Interhospital Transfer on Endovascular Treatment for Acute Ischemic Stroke.Stroke. 2019 Apr;50(4):923-930. doi: 10.1161/STROKEAHA.118.024091. Stroke. 2019. PMID: 30862265 Free PMC article.
-
Risk Assessment of the Door-In-Door-Out Process at Primary Stroke Centers for Patients With Acute Stroke Requiring Transfer to Comprehensive Stroke Centers.J Am Heart Assoc. 2021 Sep 21;10(18):e021803. doi: 10.1161/JAHA.121.021803. Epub 2021 Sep 17. J Am Heart Assoc. 2021. PMID: 34533049 Free PMC article.
-
Accuracy of Emergency Medical Services Dispatcher and Crew Diagnosis of Stroke in Clinical Practice.Front Neurol. 2017 Sep 14;8:466. doi: 10.3389/fneur.2017.00466. eCollection 2017. Front Neurol. 2017. PMID: 28959230 Free PMC article.
-
The Impact of COVID-19 on Emergent Large-Vessel Occlusion: Delayed Presentation Confirmed by ASPECTS.AJNR Am J Neuroradiol. 2020 Dec;41(12):2271-2273. doi: 10.3174/ajnr.A6800. Epub 2020 Sep 3. AJNR Am J Neuroradiol. 2020. PMID: 32883669 Free PMC article.
References
-
- Berkhemer OA, Fransen PS, Beumer D, et al. ; MR CLEAN Investigators . A randomized trial of intraarterial treatment for acute ischemic stroke. N Engl J Med. 2015;372(1):11-20. - PubMed
-
- Campbell BC, Mitchell PJ, Kleinig TJ, et al. ; EXTEND-IA Investigators . Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med. 2015;372(11):1009-1018. - PubMed
-
- Goyal M, Demchuk AM, Menon BK, et al. ; ESCAPE Trial Investigators . Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med. 2015;372(11):1019-1030. - PubMed
-
- Jovin TG, Chamorro A, Cobo E, et al. ; REVASCAT Trial Investigators . Thrombectomy within 8 hours after symptom onset in ischemic stroke. N Engl J Med. 2015;372(24):2296-2306. - PubMed
-
- Powers WJ, Derdeyn CP, Biller J, et al. ; American Heart Association Stroke Council . 2015 American Heart Association/American Stroke Association focused update of the 2013 Guidelines for the Early Management of Patients With Acute Ischemic Stroke regarding endovascular treatment: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2015;46(10):3020-3035. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Miscellaneous

