Trastuzumab uptake and its relation to efficacy in an animal model of HER2-positive breast cancer brain metastasis
- PMID: 28493046
- PMCID: PMC5495871
- DOI: 10.1007/s10549-017-4279-4
Trastuzumab uptake and its relation to efficacy in an animal model of HER2-positive breast cancer brain metastasis
Abstract
Purpose: The extent to which efficacy of the HER2 antibody Trastuzumab in brain metastases is limited by access of antibody to brain lesions remains a question of significant clinical importance. We investigated the uptake and distribution of trastuzumab in brain and mammary fat pad grafts of HER2-positive breast cancer to evaluate the relationship of these parameters to the anti-tumor activity of trastuzumab and trastuzumab emtansine (T-DM1).
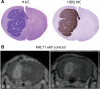
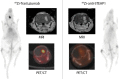
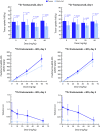
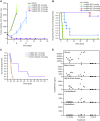
Methods: Mouse transgenic breast tumor cells expressing human HER2 (Fo2-1282 or Fo5) were used to establish intracranial and orthotopic tumors. Tumor uptake and tissue distribution of systemically administered 89Zr-trastuzumab or muMAb 4D5 (murine parent of trastuzumab) were measured by PET and ELISA. Efficacy of muMAb 4D5, the PI3K/mTOR inhibitor GNE-317, and T-DM1 was also assessed.
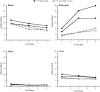
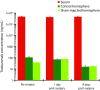
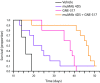
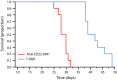
Results: 89Zr-trastuzumab and muMAb 4D5 exhibited robust uptake into Fo2-1282 brain tumors, but not normal brains. Uptake into brain grafts was similar to mammary grafts. Despite this, muMAb 4D5 was less efficacious in brain grafts. Co-administration of muMAb 4D5 and GNE-317, a brain-penetrant PI3K/mTOR inhibitor, provided longer survival in mice with brain lesions than either agent alone. Moreover, T-DM1 increased survival in the Fo5 brain metastasis model.
Conclusions: In models of HER2-positive breast cancer brain metastasis, trastuzumab efficacy does not appear to be limited by access to intracranial tumors. Anti-tumor activity improved with the addition of a brain-penetrant PI3K/mTOR inhibitor, suggesting that combining targeted therapies is a more effective strategy for treating HER2-positive breast cancer brain metastases. Survival was also extended in mice with Fo5 brain lesions treated with T-DM1.
Keywords: Blood–brain barrier; Brain metastasis; Breast cancer; T-DM1; Trastuzumab.
Conflict of interest statement
All authors are current or former employees of Genentech, Inc. and/or own stock in F. Hoffmann-La Roche, Ltd.
Figures
Comment in
-
Antibody-based therapies for the treatment of brain metastases from HER2-positive breast cancer: time to rethink the importance of the BBB?Breast Cancer Res Treat. 2017 Sep;165(2):467-468. doi: 10.1007/s10549-017-4351-0. Epub 2017 Jun 22. Breast Cancer Res Treat. 2017. PMID: 28643019 No abstract available.
-
Response Letter.Breast Cancer Res Treat. 2017 Sep;165(2):469-470. doi: 10.1007/s10549-017-4352-z. Epub 2017 Jun 30. Breast Cancer Res Treat. 2017. PMID: 28667455 No abstract available.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

