Lower Risk of Heart Failure and Death in Patients Initiated on Sodium-Glucose Cotransporter-2 Inhibitors Versus Other Glucose-Lowering Drugs: The CVD-REAL Study (Comparative Effectiveness of Cardiovascular Outcomes in New Users of Sodium-Glucose Cotransporter-2 Inhibitors)
- PMID: 28522450
- PMCID: PMC5515629
- DOI: 10.1161/CIRCULATIONAHA.117.029190
Lower Risk of Heart Failure and Death in Patients Initiated on Sodium-Glucose Cotransporter-2 Inhibitors Versus Other Glucose-Lowering Drugs: The CVD-REAL Study (Comparative Effectiveness of Cardiovascular Outcomes in New Users of Sodium-Glucose Cotransporter-2 Inhibitors)
Abstract
Background: Reduction in cardiovascular death and hospitalization for heart failure (HHF) was recently reported with the sodium-glucose cotransporter-2 inhibitor (SGLT-2i) empagliflozin in patients with type 2 diabetes mellitus who have atherosclerotic cardiovascular disease. We compared HHF and death in patients newly initiated on any SGLT-2i versus other glucose-lowering drugs in 6 countries to determine if these benefits are seen in real-world practice and across SGLT-2i class.
Methods: Data were collected via medical claims, primary care/hospital records, and national registries from the United States, Norway, Denmark, Sweden, Germany, and the United Kingdom. Propensity score for SGLT-2i initiation was used to match treatment groups. Hazard ratios for HHF, death, and their combination were estimated by country and pooled to determine weighted effect size. Death data were not available for Germany.
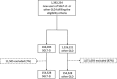
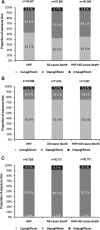
Results: After propensity matching, there were 309 056 patients newly initiated on either SGLT-2i or other glucose-lowering drugs (154 528 patients in each treatment group). Canagliflozin, dapagliflozin, and empagliflozin accounted for 53%, 42%, and 5% of the total exposure time in the SGLT-2i class, respectively. Baseline characteristics were balanced between the 2 groups. There were 961 HHF cases during 190 164 person-years follow-up (incidence rate, 0.51/100 person-years). Of 215 622 patients in the United States, Norway, Denmark, Sweden, and the United Kingdom, death occurred in 1334 (incidence rate, 0.87/100 person-years), and HHF or death in 1983 (incidence rate, 1.38/100 person-years). Use of SGLT-2i, versus other glucose-lowering drugs, was associated with lower rates of HHF (hazard ratio, 0.61; 95% confidence interval, 0.51-0.73; P<0.001); death (hazard ratio, 0.49; 95% confidence interval, 0.41-0.57; P<0.001); and HHF or death (hazard ratio, 0.54; 95% confidence interval, 0.48-0.60; P<0.001) with no significant heterogeneity by country.
Conclusions: In this large multinational study, treatment with SGLT-2i versus other glucose-lowering drugs was associated with a lower risk of HHF and death, suggesting that the benefits seen with empagliflozin in a randomized trial may be a class effect applicable to a broad population of patients with type 2 diabetes mellitus in real-world practice.
Clinical trial registration: URL: http://www.clinicaltrials.gov. Unique identifier: NCT02993614.
Keywords: canagliflozin; dapagliflozin; death; diabetes mellitus; empagliflozin; heart failure; sodium glucose transporter 2.
© 2017 The Authors.
Figures


Comment in
-
Reality and Truth: Balancing the Hope and the Hype of Real-World Evidence.Circulation. 2017 Jul 18;136(3):260-262. doi: 10.1161/CIRCULATIONAHA.117.029233. Circulation. 2017. PMID: 28716830 No abstract available.
-
Sodium-glucose cotransporter 2 inhibitors and death and heart failure in type 2 diabetes.Ann Transl Med. 2017 Dec;5(23):470. doi: 10.21037/atm.2017.09.22. Ann Transl Med. 2017. PMID: 29285503 Free PMC article. No abstract available.
-
Comparative effectiveness of cardiovascular outcomes in new users of sodium-glucose cotransporter-2 inhibitors: SGLT2 inhibitors in the real world.Ann Transl Med. 2017 Dec;5(23):474. doi: 10.21037/atm.2017.10.11. Ann Transl Med. 2017. PMID: 29285507 Free PMC article. No abstract available.
-
Letter by Tampaki et al Regarding Article, "Lower Risk of Heart Failure and Death in Patients Initiated on Sodium-Glucose Cotransporter-2 Inhibitors Versus Other Glucose-Lowering Drugs: The CVD-REAL Study (Comparative Effectiveness of Cardiovascular Outcomes in New Users of Sodium-Glucose Cotransporter-2 Inhibitors)".Circulation. 2018 Feb 27;137(9):982-983. doi: 10.1161/CIRCULATIONAHA.117.030339. Circulation. 2018. PMID: 29483176 No abstract available.
-
Letter by Koh Regarding Article, "Lower Risk of Heart Failure and Death in Patients Initiated on Sodium-Glucose Cotransporter-2 Inhibitors Versus Other Glucose-Lowering Drugs: The CVD-REAL Study (Comparative Effectiveness of Cardiovascular Outcomes in New Users of Sodium-Glucose Cotransporter-2 Inhibitors)".Circulation. 2018 Feb 27;137(9):984-985. doi: 10.1161/CIRCULATIONAHA.117.030650. Circulation. 2018. PMID: 29483177 No abstract available.
-
Letter by Taegtmeyer and Karlstaedt Regarding Article, "Lower Risk of Heart Failure and Death in Patients Initiated on Sodium-Glucose Cotransporter-2 Inhibitors Versus Other Glucose-Lowering Drugs: The CVD-REAL Study (Comparative Effectiveness of Cardiovascular Outcomes in New Users of Sodium-Glucose Cotransporter-2 Inhibitors)".Circulation. 2018 Feb 27;137(9):986-987. doi: 10.1161/CIRCULATIONAHA.117.031193. Circulation. 2018. PMID: 29483178 Free PMC article. No abstract available.
-
Letter by Jin-shan and Xue-bin Regarding Article, "Lower Risk of Heart Failure and Death in Patients Initiated on Sodium-Glucose Cotransporter-2 Inhibitors Versus Other Glucose-Lowering Drugs: The CVD-REAL Study (Comparative Effectiveness of Cardiovascular Outcomes in New Users of Sodium-Glucose Cotransporter-2 Inhibitors)".Circulation. 2018 Feb 27;137(9):988. doi: 10.1161/CIRCULATIONAHA.117.031407. Circulation. 2018. PMID: 29483179 No abstract available.
-
Response by Kosiborod et al to Letters Regarding Article, "Lower Risk of Heart Failure and Death in Patients Initiated on Sodium-Glucose Cotransporter-2 Inhibitors Versus Other Glucose-Lowering Drugs: The CVD-REAL Study (Comparative Effectiveness of Cardiovascular Outcomes in New Users of Sodium-Glucose Cotransporter-2 Inhibitors)".Circulation. 2018 Feb 27;137(9):989-991. doi: 10.1161/CIRCULATIONAHA.117.031847. Circulation. 2018. PMID: 29483180 No abstract available.
-
Sodium-glucose cotransporter-2 inhibitors and cardiovascular outcomes: insights from the CVD-REAL study.Ann Transl Med. 2018 Feb;6(3):55. doi: 10.21037/atm.2017.11.08. Ann Transl Med. 2018. PMID: 29610747 Free PMC article. No abstract available.
References
-
- Sarwar N, Gao P, Seshasai SR, Gobin R, Kaptoge S, Di Angelantonio E, Ingelsson E, Lawlor DA, Selvin E, Stampfer M, Stehouwer CD, Lewington S, Pennells L, Thompson A, Sattar N, White IR, Ray KK, Danesh J Emerging Risk Factors Collaboration. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet. 2010;375:2215–2222. doi: 10.1016/S0140-6736(10)60484-9. - PMC - PubMed
-
- Schocken DD, Benjamin EJ, Fonarow GC, Krumholz HM, Levy D, Mensah GA, Narula J, Shor ES, Young JB, Hong Y American Heart Association Council on Epidemiology and Prevention; American Heart Association Council on Clinical Cardiology; American Heart Association Council on Cardiovascular Nursing; American Heart Association Council on High Blood Pressure Research; Quality of Care and Outcomes Research Interdisciplinary Working Group; Functional Genomics and Translational Biology Interdisciplinary Working Group. Prevention of heart failure: a scientific statement from the American Heart Association Councils on Epidemiology and Prevention, Clinical Cardiology, Cardiovascular Nursing, and High Blood Pressure Research; Quality of Care and Outcomes Research Interdisciplinary Working Group; and Functional Genomics and Translational Biology Interdisciplinary Working Group. Circulation. 2008;117:2544–2565. doi: 10.1161/CIRCULATIONAHA.107.188965. - PubMed
-
- Di Angelantonio E, Kaptoge S, Wormser D, Willeit P, Butterworth AS, Bansal N, O’Keeffe LM, Gao P, Wood AM, Burgess S, Freitag DF, Pennells L, Peters SA, Hart CL, Håheim LL, Gillum RF, Nordestgaard BG, Psaty BM, Yeap BB, Knuiman MW, Nietert PJ, Kauhanen J, Salonen JT, Kuller LH, Simons LA, van der Schouw YT, Barrett-Connor E, Selmer R, Crespo CJ, Rodriguez B, Verschuren WM, Salomaa V, Svärdsudd K, van der Harst P, Björkelund C, Wilhelmsen L, Wallace RB, Brenner H, Amouyel P, Barr EL, Iso H, Onat A, Trevisan M, D’Agostino RB, Sr, Cooper C, Kavousi M, Welin L, Roussel R, Hu FB, Sato S, Davidson KW, Howard BV, Leening MJ, Leening M, Rosengren A, Dörr M, Deeg DJ, Kiechl S, Stehouwer CD, Nissinen A, Giampaoli S, Donfrancesco C, Kromhout D, Price JF, Peters A, Meade TW, Casiglia E, Lawlor DA, Gallacher J, Nagel D, Franco OH, Assmann G, Dagenais GR, Jukema JW, Sundström J, Woodward M, Brunner EJ, Khaw KT, Wareham NJ, Whitsel EA, Njølstad I, Hedblad B, Wassertheil-Smoller S, Engström G, Rosamond WD, Selvin E, Sattar N, Thompson SG, Danesh J Emerging Risk Factors Collaboration. Association of cardiometabolic multimorbidity with mortality. JAMA. 2015;314:52–60. doi: 10.1001/jama.2015.7008. - PMC - PubMed
-
- Kannel WB, Hjortland M, Castelli WP. Role of diabetes in congestive heart failure: the Framingham study. Am J Cardiol. 1974;34:29–34. - PubMed
-
- IDF Diabetes Atlas Group. Update of mortality attributable to diabetes for the IDF diabetes atlas: estimates for the year 2011. Diabetes Res Clin Pract. 2013;100:277–279. doi: 10.1016/j.diabres.2013.02.005. - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

