Diagnostic Accuracy of Ga-68-HBED-CC-PSMA-Ligand-PET/CT before Salvage Lymph Node Dissection for Recurrent Prostate Cancer
- PMID: 28529650
- PMCID: PMC5436526
- DOI: 10.7150/thno.18421
Diagnostic Accuracy of Ga-68-HBED-CC-PSMA-Ligand-PET/CT before Salvage Lymph Node Dissection for Recurrent Prostate Cancer
Abstract
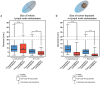
Background: By targeting the prostate-specific membrane antigen (PSMA) on prostate cancer (PCa) cells PSMA-PET/CT shows great potential in locating the site of biochemical recurrence even at low PSA (Prostate-specific antigen)-levels. Accurate imaging of PCa recurrent lymph node metastases (LNM) is crucial for metastases directed therapies such as salvage-lymph node dissection (salvage-LND). Objective: To evaluate the diagnostic accuracy of PSMA-PET/CT for detection of affected lymph-node regions at salvage-LND for nodal recurrence of PCa. Design, setting and participants: 30 patients with the suspicion of exclusively nodal PCa-relapse after primary therapy underwent a template pelvic and/or retroperitoneal salvage-LND after whole body 68-Ga-PSMA-PET/CT. The diagnostic accuracy of PET/CT was evaluated in comparison to the histopathology of 965 resected lymph nodes (LN) dissected from 68 main regions (pelvic left/right, retroperitoneal) and 289 subregions (common iliac, external iliac, obturator, internal iliac, presacral, aortic-bifurcation, aortal, caval). LNM and tumor deposits in LNM were measured bidimensionally in the histopathology. PSMA-expression was analyzed by immunohistochemistry in LNM. Results: LNM were present in 11.4% of the resected LN (110/965) resulting in 45 positive main regions and 85 positive subregions. PET/CT was true positive in 41 main regions and 69 subregions. Three PET-negative main regions and 16 PET-negative subregions finally contained LNM, the majority of these false negative subregions (13/16) were in neighboring regions of true-positive subregions. Sensitivity, specificity, positive predictive value, negative predictive value and accuracy were: main region-based 93.2%, 100%, 100%, 88.9% and 95.6%, subregion-based 81.2%, 99.5%, 98.6%, 92.7 and 94.1%. Median short diameters of tumor deposits in LNM resected from false-negative subregions (1.3 mm) were significantly smaller than in LNM removed from true-positive subregions (5.5 mm, p<0.0001). Based on anatomical subregions containing just one LNM, the necessary short diameter of tumor deposits in LNM required to reach a detection rate of 50% and 90% was estimated to be ≥ 2.3 mm and ≥ 4.5 mm, respectively. Conclusion: In men with biochemical PCa-relapse and positive PSMA-PET/CT, PET/CT detects metastatic affected anatomical regions with high accuracy at a main region and at a subregion-level. If the decision for salvage-LND is prompted by a positive PSMA-PET/CT, the size of metastases is crucial for accurate detection of affected regions. All LNM showed a clear PSMA-expression in the immunohistochemistry. Further studies need to investigate how to translate the high anatomical correlation observed between PET/CT and surgical findings into optimal approaches for target salvage-LND.
Keywords: PSMA-PET/CT; prostate cancer, lymph node metastases; salvage lymph node dissection; salvage lymphadenectomy..
Conflict of interest statement
Competing Interests: PTM received financial support for on-going research by GE and Piramal Imaging unrelated to the present study. CAJ, VD, TB, KS, WSS, UW, HCR, WV have no financial disclosures.
Figures




Comment in
-
Re: Diagnostic Accuracy of Ga-68-HBED-CC-PSMA-ligand-PET/CT Before Salvage Lymph Node Dissection for Recurrent Prostate Cancer.Eur Urol. 2017 Sep;72(3):470-471. doi: 10.1016/j.eururo.2017.05.007. Epub 2017 May 15. Eur Urol. 2017. PMID: 28522176 No abstract available.
-
PSMA-PET for Lymph Node Detection in Recurrent Prostate Cancer: How do we use the Magic Bullet?Theranostics. 2017 May 15;7(7):2046-2047. doi: 10.7150/thno.20855. eCollection 2017. Theranostics. 2017. PMID: 28638485 Free PMC article. No abstract available.
References
-
- Heidenreich A, Bastian PJ, Bellmunt J, Bolla M, Joniau S, van der Kwast T. et al. EAU guidelines on prostate cancer. Part II: Treatment of advanced, relapsing, and castration-resistant prostate cancer. European urology. 2014;65:467–79. - PubMed
-
- Heidenreich A, Bastian PJ, Bellmunt J, Bolla M, Joniau S, van der Kwast T. et al. EAU guidelines on prostate cancer. part 1: screening, diagnosis, and local treatment with curative intent-update 2013. European urology. 2014;65:124–37. - PubMed
-
- Picchio M, Briganti A, Fanti S, Heidenreich A, Krause BJ, Messa C. et al. The role of choline positron emission tomography/computed tomography in the management of patients with prostate-specific antigen progression after radical treatment of prostate cancer. European urology. 2011;59:51–60. - PubMed
-
- Jilg CA, Schultze-Seemann W, Drendel V, Vach W, Wieser G, Krauss T, Detection of Lymph Node Metastasis in Patients with Nodal Prostate Cancer Relapse Using F/C-Choline Positron Emission Tomography/Computerized Tomography. The Journal of urology; 2014. - PubMed
-
- Cimitan M, Evangelista L, Hodolic M, Mariani G, Baseric T, Bodanza V. et al. Gleason score at diagnosis predicts the rate of detection of 18F-choline PET/CT performed when biochemical evidence indicates recurrence of prostate cancer: experience with 1,000 patients. J Nucl Med. 2015;56:209–15. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

