Loss of 'homeostatic' microglia and patterns of their activation in active multiple sclerosis
- PMID: 28541408
- PMCID: PMC6057548
- DOI: 10.1093/brain/awx113
Loss of 'homeostatic' microglia and patterns of their activation in active multiple sclerosis
Abstract
Microglia and macrophages accumulate at the sites of active demyelination and neurodegeneration in the multiple sclerosis brain and are thought to play a central role in the disease process. We used recently described markers to characterize the origin and functional states of microglia/macrophages in acute, relapsing and progressive multiple sclerosis. We found microglia activation in normal white matter of controls and that the degree of activation increased with age. This microglia activation was more pronounced in the normal-appearing white matter of patients in comparison to controls and increased with disease duration. In contrast to controls, the normal-appearing white matter of patients with multiple sclerosis showed a significant reduction of P2RY12, a marker expressed in homeostatic microglia in rodents, which was completely lost in active and slowly expanding lesions. Early stages of demyelination and neurodegeneration in active lesions contained microglia with a pro-inflammatory phenotype, which expressed molecules involved in phagocytosis, oxidative injury, antigen presentation and T cell co-stimulation. In later stages, the microglia and macrophages in active lesions changed to a phenotype that was intermediate between pro- and anti-inflammatory activation. In inactive lesions, the density of microglia/macrophages was significantly reduced and microglia in part converted to a P2RY12+ phenotype. Analysis of TMEM119, which is expressed on microglia but not on recruited macrophages, demonstrated that on average 45% of the macrophage-like cells in active lesions were derived from the resident microglia pool. Our study demonstrates the loss of the homeostatic microglial signature in active multiple sclerosis with restoration associated with disease inactivity.
Keywords: demyelination; macrophages; microglia; multiple sclerosis; neurodegeneration.
© The Author (2017). Published by Oxford University Press on behalf of the Guarantors of Brain.
Figures

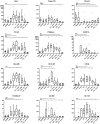


References
-
- Andersen CB, Stodkilde K, Saederup KL, Kuhlee A, Raunser S, Graversen JH. et al. Haptoglobin. Antioxid Redox Signal 2017; 26: 814–31. - PubMed
-
- Babinski J. Recherches sur l’anatomie pathologique de la sclerose en plaque et étude comparative des diverses variétés de la scleroses de la moelle. Arch Physiol 1885; 5: 186–207.
-
- Barnett MH, Prineas JW. Relapsing and remitting multiple sclerosis: pathology of the newly forming lesion. Ann Neurol 2004; 55: 458–68. - PubMed
-
- Bauer J, Lassmann H. Neuropathological techniques to investigate central nervous system sections in multiple sclerosis. Methods Mol Biol 2016; 1304: 211–29 - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases

