Pseudomonas aeruginosa urinary tract infections in hospitalized patients: Mortality and prognostic factors
- PMID: 28552972
- PMCID: PMC5446154
- DOI: 10.1371/journal.pone.0178178
Pseudomonas aeruginosa urinary tract infections in hospitalized patients: Mortality and prognostic factors
Abstract
Background: The aim of this study was to analyze the mortality and predictors of 30-day mortality among hospitalized patients with Pseudomonas aeruginosa urinary tract infection (PAUTI) and the impact of antibiotic treatment on survival.
Methods: Patients admitted to our hospital with PAUTI or those diagnosed of PAUTI during hospitalization for other disease between September 2012 and September 2014 were included. Repeated episodes from the same patient were excluded. Database with demographic, clinical and laboratory ítems was created. Empirical and definitive antibiotic therapy, antimicrobial resistance and all-cause mortality at 30 and 90 days were included.
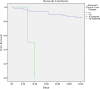
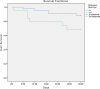
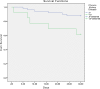
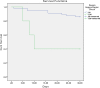
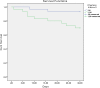
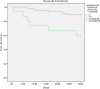
Results: 62 patients were included, with a mean age of 75 years. 51% were male. Mortality was 17.7% at 30 days and 33.9% at 90 days. Factors associated with reduced survival at 30 days were chronic liver disease with portal hypertension (P<0,01), diabetes mellitus (P = 0,04) chronic renal failure (P = 0,02), severe sepsis or septic shock (P<0,01), Charlson index > 3 (P = 0.02) and inadequated definitive antibiotic treatment (P<0,01). Independent risk factors for mortality in multivariate analysis were advanced chronic liver disease (HR 77,4; P<0,01), diabetes mellitus (HR 3,6; P = 0,04), chronic renal failure (HR 4,1; P = 0,03) and inadequated definitive antimicrobial treatment (HR 6,8; P = 0,01).
Conclusions: PAUTI are associated with high mortality in hospitalized patients, which increases significantly in those with severe comorbidity such as chronic renal failure, advanced liver disease or diabetes mellitus. Inadequated antibiotic treatment is associated with poor outcome, which remarks the importance of adjusting empirical antibiotic treatment based on the microbiological susceptibility results.
Conflict of interest statement
Figures
References
-
- Horcajada JP, Shaw E, Padilla B, Pintado V, Calbo E, Benito N, et al. Healthcare-associated, community-acquired and hospital-acquired bacteraemic urinary tract infections in hospitalized patients: a prospective multicentre cohort study in the era of antimicrobial resistance. Clin Microbiol Infect. 2013;9:962–8. - PubMed
-
- Gastmeier P. Nosocomial urinary tract infections: many unresolved questions. Clin Microbiol Infect. 2001;7:521–522. - PubMed
-
- Bouza E, San Juan R, Muñoz P, Voss A, Kluytmans J. A European perspective on nosocomial urinary tract infections I. Report on the microbiology workload, etiology and antimicrobial susceptibility (ESGNI-003 study). European Study Group on Nosocomial Infections. Clin Microbiol Infect. 2001: 7: 523–531. - PubMed
-
- Djordjevic Z, Folic MM, Zivic Z, Markovic V, Jankovic SM. Nosocomial urinary tract infections caused by Pseudomonas aeruginosa and Acinetobacter species: sensitivity to antibiotics and risk factors. Am J Infect Control. 2013;41:1182–7. doi: 10.1016/j.ajic.2013.02.018 - DOI - PubMed
-
- Horino T, Chiba A, Kawano S, Kato T, Sato F, Maruyama Y,et al. Clinical characteristics and risk factors for mortality in patients with bacteremia caused by Pseudomonas aeruginosa. Intern Med. 2012;51:59–64. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

