Maternal and Fetal Outcomes of Anticoagulation in Pregnant Women With Mechanical Heart Valves
- PMID: 28571631
- PMCID: PMC5457289
- DOI: 10.1016/j.jacc.2017.03.605
Maternal and Fetal Outcomes of Anticoagulation in Pregnant Women With Mechanical Heart Valves
Abstract
Background: Anticoagulation for mechanical heart valves during pregnancy is essential to prevent thromboembolic events. Each regimen has drawbacks with regard to maternal or fetal risk.
Objectives: This meta-analysis sought to estimate and compare the risk of adverse maternal and fetal outcomes in pregnant women with mechanical heart valves who received different methods of anticoagulation.
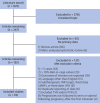
Methods: Studies were identified using a Medline search including all publications up to June 5, 2016. Study inclusion required reporting of maternal death, thromboembolism, and valve failure, and/or fetal spontaneous abortion, death, and congenital defects in pregnant women treated with any of the following: 1) a vitamin K antagonist (VKA) throughout pregnancy; 2) low-molecular-weight heparin (LMWH) throughout pregnancy; 3) LMWH for the first trimester, followed by a VKA (LMWH and VKA); or 4) unfractionated heparin for the first trimester, followed by a VKA (UFH and VKA).
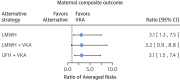
Results: A total of 800 pregnancies from 18 publications were included. Composite maternal risk was lowest with VKA (5%), compared with LMWH (16%; ratio of averaged risk [RAR]: 3.2; 95% confidence interval [CI]: 1.5 to 7.5), LMWH and VKA (16%; RAR: 3.1; 95% CI: 1.2 to 7.5), or UFH and VKA (16%; RAR: 3.1; 95% CI: 1.5 to 7.1). Composite fetal risk was lowest with LMWH (13%; RAR: 0.3; 95% CI: 0.1 to 0.8), compared with VKA (39%), LMWH and VKA (23%), or UFH and VKA (34%). No significant difference in fetal risk was observed between women taking ≤5 mg daily warfarin and those with an LMWH regimen (RAR: 0.9; 95% CI: 0.3 to 2.4).
Conclusions: VKA treatment was associated with the lowest risk of adverse maternal outcomes, whereas the use of LMWH throughout pregnancy was associated with the lowest risk of adverse fetal outcomes. Fetal risk was similar between women taking ≤5 mg warfarin daily and women treated with LMWH.
Keywords: fetal risk; maternal risk; pregnancy.
Copyright © 2017 The Authors. Published by Elsevier Inc. All rights reserved.
Figures




Comment in
-
Anticoagulation Therapy for Pregnant Women With Mechanical Prosthetic Heart Valves: How to Improve Safety?J Am Coll Cardiol. 2017 Jun 6;69(22):2692-2695. doi: 10.1016/j.jacc.2017.04.034. J Am Coll Cardiol. 2017. PMID: 28571632 No abstract available.
-
The Anticoagulation Conundrum of Mechanical Heart Valves in Pregnancy: Should DOACs Be Considered?J Am Coll Cardiol. 2017 Dec 19;70(24):3073-3074. doi: 10.1016/j.jacc.2017.09.1138. J Am Coll Cardiol. 2017. PMID: 29241498 No abstract available.
-
Reply: The Anticoagulation Conundrum of Mechanical Heart Valves in Pregnancy: Should DOACs Be Considered?J Am Coll Cardiol. 2017 Dec 19;70(24):3074-3075. doi: 10.1016/j.jacc.2017.09.1139. J Am Coll Cardiol. 2017. PMID: 29241499 No abstract available.
References
-
- Kujovich J.L. Hormones and pregnancy: thromboembolic risks for women. Br J Haematol. 2004;126:443–454. - PubMed
-
- Bonow R.O., Carabello B.A., Chatterjee K. 2008 Focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol. 2008;52:e1–e142. - PubMed
-
- Hall J.G., Pauli R.M., Wilson K.M. Maternal and fetal sequelae of anticoagulation during pregnancy. Am J Med. 1980;68:122–140. - PubMed
-
- Iturbe-Alessio I., Fonseca M.C., Mutchinik O., Santos M.A., Zajarias A., Salazar E. Risks of anticoagulant therapy in pregnant women with artificial heart valves. N Engl J Med. 1986;315:1390–1393. - PubMed
-
- Sareli P., England M.J., Berk M.R. Maternal and fetal sequelae of anticoagulation during pregnancy in patients with mechanical heart valve prostheses. Am J Cardiol. 1989;63:1462–1465. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

