The Lumbodorsal Fascia as a Potential Source of Low Back Pain: A Narrative Review
- PMID: 28584816
- PMCID: PMC5444000
- DOI: 10.1155/2017/5349620
The Lumbodorsal Fascia as a Potential Source of Low Back Pain: A Narrative Review
Abstract
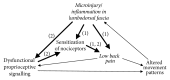
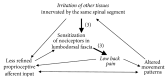
The lumbodorsal fascia (LF) has been proposed to represent a possible source of idiopathic low back pain. In fact, histological studies have demonstrated the presence of nociceptive free nerve endings within the LF, which, furthermore, appear to exhibit morphological changes in patients with chronic low back pain. However, it is unclear how these characteristics relate to the aetiology of the pain. In vivo elicitation of back pain via experimental stimulation of the LF suggests that dorsal horn neurons react by increasing their excitability. Such sensitization of fascia-related dorsal horn neurons, in turn, could be related to microinjuries and/or inflammation in the LF. Despite available data point towards a significant role of the LF in low back pain, further studies are needed to better understand the involved neurophysiological dynamics.
Figures

References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

