Association of Gestational Weight Gain With Maternal and Infant Outcomes: A Systematic Review and Meta-analysis
- PMID: 28586887
- PMCID: PMC5815056
- DOI: 10.1001/jama.2017.3635
Association of Gestational Weight Gain With Maternal and Infant Outcomes: A Systematic Review and Meta-analysis
Abstract
Importance: Body mass index (BMI) and gestational weight gain are increasing globally. In 2009, the Institute of Medicine (IOM) provided specific recommendations regarding the ideal gestational weight gain. However, the association between gestational weight gain consistent with theIOM guidelines and pregnancy outcomes is unclear.
Objective: To perform a systematic review, meta-analysis, and metaregression to evaluate associations between gestational weight gain above or below the IOM guidelines (gain of 12.5-18 kg for underweight women [BMI <18.5]; 11.5-16 kg for normal-weight women [BMI 18.5-24.9]; 7-11 kg for overweight women [BMI 25-29.9]; and 5-9 kg for obese women [BMI ≥30]) and maternal and infant outcomes.
Data sources and study selection: Search of EMBASE, Evidence-Based Medicine Reviews, MEDLINE, and MEDLINE In-Process between January 1, 1999, and February 7, 2017, for observational studies stratified by prepregnancy BMI category and total gestational weight gain.
Data extraction and synthesis: Data were extracted by 2 independent reviewers. Odds ratios (ORs) and absolute risk differences (ARDs) per live birth were calculated using a random-effects model based on a subset of studies with available data.
Main outcomes and measures: Primary outcomes were small for gestational age (SGA), preterm birth, and large for gestational age (LGA). Secondary outcomes were macrosomia, cesarean delivery, and gestational diabetes mellitus.
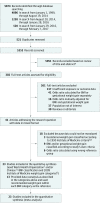
Results: Of 5354 identified studies, 23 (n = 1 309 136 women) met inclusion criteria. Gestational weight gain was below or above guidelines in 23% and 47% of pregnancies, respectively. Gestational weight gain below the recommendations was associated with higher risk of SGA (OR, 1.53 [95% CI, 1.44-1.64]; ARD, 5% [95% CI, 4%-6%]) and preterm birth (OR, 1.70 [1.32-2.20]; ARD, 5% [3%-8%]) and lower risk of LGA (OR, 0.59 [0.55-0.64]; ARD, -2% [-10% to -6%]) and macrosomia (OR, 0.60 [0.52-0.68]; ARD, -2% [-3% to -1%]); cesarean delivery showed no significant difference (OR, 0.98 [0.96-1.02]; ARD, 0% [-2% to 1%]). Gestational weight gain above the recommendations was associated with lower risk of SGA (OR, 0.66 [0.63-0.69]; ARD, -3%; [-4% to -2%]) and preterm birth (OR, 0.77 [0.69-0.86]; ARD, -2% [-2% to -1%]) and higher risk of LGA (OR, 1.85 [1.76-1.95]; ARD, 4% [2%-5%]), macrosomia (OR, 1.95 [1.79-2.11]; ARD, 6% [4%-9%]), and cesarean delivery (OR, 1.30 [1.25-1.35]; ARD, 4% [3%-6%]). Gestational diabetes mellitus could not be evaluated because of the nature of available data.
Conclusions and relevance: In this systematic review and meta-analysis of more than 1 million pregnant women, 47% had gestational weight gain greater than IOM recommendations and 23% had gestational weight gain less than IOM recommendations. Gestational weight gain greater than or less than guideline recommendations, compared with weight gain within recommended levels, was associated with higher risk of adverse maternal and infant outcomes.
Conflict of interest statement
Figures


Comment in
-
Gestational Weight Gain and Outcomes for Mothers and Infants.JAMA. 2017 Jun 6;317(21):2175-2176. doi: 10.1001/jama.2017.6265. JAMA. 2017. PMID: 28586874 No abstract available.
References
-
- Nohr EA, Vaeth M, Baker JL, Sørensen TIA, Olsen J, Rasmussen KM. Combined associations of prepregnancy body mass index and gestational weight gain with the outcome of pregnancy [erratum appears in Am J Clin Nutr. 2008;88(6):1705]. Am J Clin Nutr. 2008;87(6):1750-1759. - PubMed
-
- Hrolfsdottir L, Rytter D, Olsen SF, et al. Gestational weight gain in normal weight women and offspring cardio-metabolic risk factors at 20 years of age. Int J Obes (Lond). 2015;39(4):671-676. - PubMed
-
- Institute of Medicine Nutrition During Pregnancy: Part I: Weight Gain, Part II Nutrient Supplements. Washington, DC: National Academies Press; 1990. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

