Mobilized Peripheral Blood Stem Cells Versus Unstimulated Bone Marrow As a Graft Source for T-Cell-Replete Haploidentical Donor Transplantation Using Post-Transplant Cyclophosphamide
- PMID: 28644773
- PMCID: PMC5590802
- DOI: 10.1200/JCO.2017.72.8428
Mobilized Peripheral Blood Stem Cells Versus Unstimulated Bone Marrow As a Graft Source for T-Cell-Replete Haploidentical Donor Transplantation Using Post-Transplant Cyclophosphamide
Erratum in
-
Errata.J Clin Oncol. 2019 Feb 20;37(6):528. doi: 10.1200/JCO.19.00034. J Clin Oncol. 2019. PMID: 30768918 Free PMC article. No abstract available.
Abstract
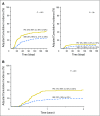
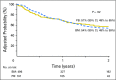
Purpose T-cell-replete HLA-haploidentical donor hematopoietic transplantation using post-transplant cyclophosphamide was originally described using bone marrow (BM). With increasing use of mobilized peripheral blood (PB), we compared transplant outcomes after PB and BM transplants. Patients and Methods A total of 681 patients with hematologic malignancy who underwent transplantation in the United States between 2009 and 2014 received BM (n = 481) or PB (n = 190) grafts. Cox regression models were built to examine differences in transplant outcomes by graft type, adjusting for patient, disease, and transplant characteristics. Results Hematopoietic recovery was similar after transplantation of BM and PB (28-day neutrophil recovery, 88% v 93%, P = .07; 100-day platelet recovery, 88% v 85%, P = .33). Risks of grade 2 to 4 acute (hazard ratio [HR], 0.45; P < .001) and chronic (HR, 0.35; P < .001) graft-versus-host disease were lower with transplantation of BM compared with PB. There were no significant differences in overall survival by graft type (HR, 0.99; P = .98), with rates of 54% and 57% at 2 years after transplantation of BM and PB, respectively. There were no differences in nonrelapse mortality risks (HR, 0.92; P = .74) but relapse risks were higher after transplantation of BM (HR, 1.49; P = .009). Additional exploration confirmed that the higher relapse risks after transplantation of BM were limited to patients with leukemia (HR, 1.73; P = .002) and not lymphoma (HR, 0.87; P = .64). Conclusion PB and BM grafts are suitable for haploidentical transplantation with the post-transplant cyclophosphamide approach but with differing patterns of treatment failure. Although, to our knowledge, this is the most comprehensive comparison, these findings must be validated in a randomized prospective comparison with adequate follow-up.
Figures


Comment in
-
Haploidentical Hematopoietic Cell Transplantation Using Post-Transplantation Cyclophosphamide: Does Graft Source Matter?J Clin Oncol. 2017 Sep 10;35(26):2984-2986. doi: 10.1200/JCO.2017.73.7775. Epub 2017 Jul 10. J Clin Oncol. 2017. PMID: 28692380 No abstract available.
References
-
- O’Donnell PV, Luznik L, Jones RJ, et al. Nonmyeloablative bone marrow transplantation from partially HLA-mismatched related donors using posttransplantation cyclophosphamide. Biol Blood Marrow Transplant. 2002;8:377–386. - PubMed
-
- Bashey A, Zhang X, Sizemore CA, et al. T-cell-replete HLA-haploidentical hematopoietic transplantation for hematologic malignancies using post-transplantation cyclophosphamide results in outcomes equivalent to those of contemporaneous HLA-matched related and unrelated donor transplantation. J Clin Oncol. 2013;31:1310–1316. - PubMed
-
- Raiola AM, Dominietto A, di Grazia C, et al. Unmanipulated haploidentical transplants compared with other alternative donors and matched sibling grafts. Biol Blood Marrow Transplant. 2014;20:1573–1579. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

