What will make a difference? Assessing the impact of policy and non-policy scenarios on estimations of the future GP workforce
- PMID: 28659172
- PMCID: PMC5490216
- DOI: 10.1186/s12960-017-0216-1
What will make a difference? Assessing the impact of policy and non-policy scenarios on estimations of the future GP workforce
Abstract
Background: Health workforce planning is based on estimates of future needs for and supply of health care services. Given the pipeline time lag for the training of health professionals, inappropriate workforce planning or policies can lead to extended periods of over- or under-supply of health care providers. Often these policy interventions focus on one determinant of supply and do not incorporate other determinants such as changes in population health which impact the need for services. The aim of this study is to examine the effect of the implementation of various workforce policies on the estimated future requirements of the GP workforce, using South Australia as a case study. This is examined in terms of the impact on the workforce gap (excess or shortage), the cost of these workforce policies, and their role in addressing potential non-policy-related future scenarios.
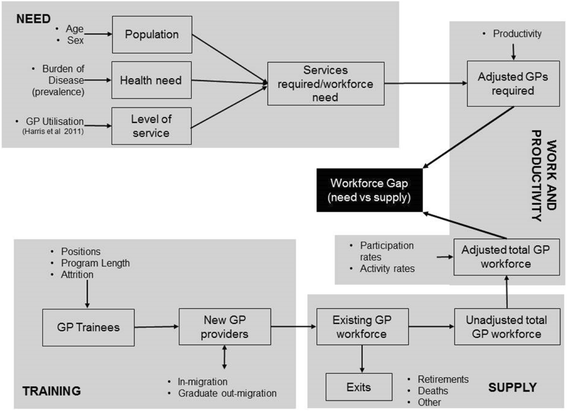
Methods: An integrated simulation model for the general practice workforce in South Australia was developed, which determines the supply and level of services required based on the health of the population over a projection period 2013-2033. The published model is used to assess the effects of various policy and workforce scenarios. For each policy scenario, associated costs were estimated and compared to baseline costs with a 5% discount rate applied.
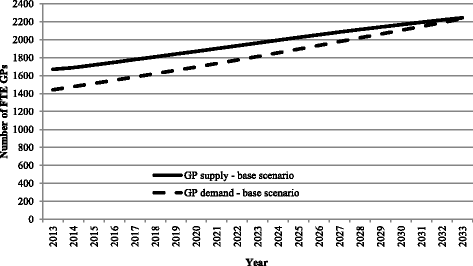
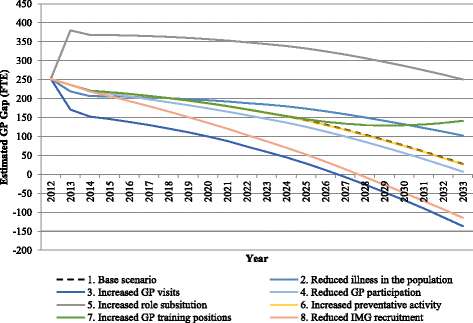
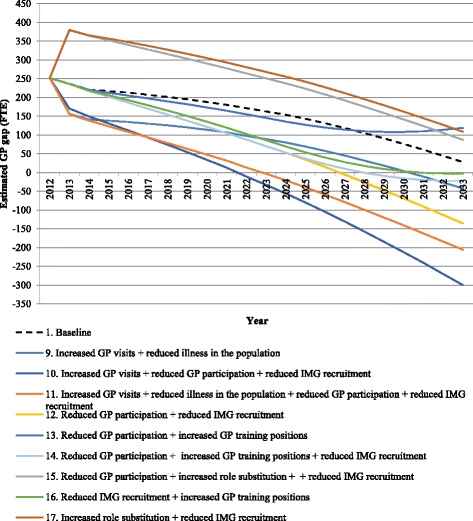
Results: The baseline scenario estimated an excess supply of GPs of 236 full-time equivalent (FTE) in 2013 but this surplus decreased to 28 FTE by 2033. The estimates based on single policy scenarios of role substitution and increased training positions continue the surplus, while a scenario that reduces the number of international medical graduates (IMGs) recruited estimated a move from surplus to shortage by 2033. The best-case outcome where the workforce achieves balance by 2023 and remains balanced to 2033, arose when GP participation rates (a non-policy scenario) were combined with the policy levers of increased GP training positions and reduced IMG recruitment. The cost of each policy varied, with increased role substitution and reduced IMG recruitment resulting in savings (AUD$752,946,586 and AUD$3,783,291 respectively) when compared to baseline costs. Increasing GP training costs over the projection period would cost the government an additional AUD$12,719,798.
Conclusions: Over the next 20 years, South Australia's GP workforce is predicted to remain fairly balanced. However, exogenous changes, such as increased demand for GP services may require policy intervention to address associated workforce shortfalls. The workforce model presented in this paper should be updated at regular intervals to inform the need for policy intervention.
Keywords: Cost; General practice; Simulation modelling; Workforce.
Conflict of interest statement
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
Similar articles
-
Improving the planning of the GP workforce in Australia: a simulation model incorporating work transitions, health need and service usage.Hum Resour Health. 2016 Apr 11;14:13. doi: 10.1186/s12960-016-0110-2. Hum Resour Health. 2016. PMID: 27067272 Free PMC article.
-
The never ending road: improving, adapting and refining a needs-based model to estimate future general practitioner requirements in two Australian states.Fam Pract. 2018 Mar 27;35(2):193-198. doi: 10.1093/fampra/cmx087. Fam Pract. 2018. PMID: 28973137
-
General practitioner workforce planning: assessment of four policy directions.BMC Health Serv Res. 2010 Jun 2;10:148. doi: 10.1186/1472-6963-10-148. BMC Health Serv Res. 2010. PMID: 20525163 Free PMC article.
-
Population risk factors and trends in health care and public policy.J Acad Nutr Diet. 2012 Mar;112(3 Suppl):S35-46. doi: 10.1016/j.jand.2011.12.011. J Acad Nutr Diet. 2012. PMID: 22709860 Review.
-
Reviewing reliance on overseas-trained doctors in rural Australia and planning for self-sufficiency: applying 10 years' MABEL evidence.Hum Resour Health. 2019 Jan 22;17(1):8. doi: 10.1186/s12960-018-0339-z. Hum Resour Health. 2019. PMID: 30670027 Free PMC article. Review.
Cited by
-
Managing uncertainty in forecasting health workforce demand using the Robust Workforce Planning Framework: the example of midwives in Belgium.Hum Resour Health. 2023 Sep 18;21(1):75. doi: 10.1186/s12960-023-00861-1. Hum Resour Health. 2023. PMID: 37723568 Free PMC article.
References
-
- Health Workforce Australia . Health workforce 2025: doctors, nurses and midwives Volume 1. Adelaide: HWA; 2012.
-
- Mason J. Review of Australian Government Health Workforce Programs. Canberra: Department of Health; 2013.
-
- Commonwealth Department of Health and aGed Care . More doctors for outer metropolitan areas measure. Canberra: Department of Health; 2000.
-
- Commonwealth Department of Health and Aged Care . More doctors, better services Regional Health Strategy. Canberra: Department of Health; 2000.
-
- Health Workforce Australia . Australia's future health workforce - doctors. Canberra: Health Workforce Australia; 2014.
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

