Vacuum-assisted early transanal closure of leaking low colorectal anastomoses: the CLEAN study
- PMID: 28664443
- PMCID: PMC5770507
- DOI: 10.1007/s00464-017-5679-6
Vacuum-assisted early transanal closure of leaking low colorectal anastomoses: the CLEAN study
Abstract
Introduction: Non-healing of anastomotic leakage can be observed in up to 50% after total mesorectal excision for rectal cancer. This study investigates the efficacy of early transanal closure of anastomotic leakage after pre-treatment with the Endosponge® therapy.
Methods: In this prospective, multicentre, feasibility study, transanal suturing of the anastomotic defect was performed after vacuum-assisted cleaning of the presacral cavity. Primary outcome was the proportion of patients with a healed anastomosis at 6 months after transanal closure. Secondary, healing at last follow-up, continuity, direct medical costs, functionality and quality of life were analysed.
Results: Between July 2013 and July 2015, 30 rectal cancer patients with a leaking low colorectal anastomosis were included, of whom 22 underwent neoadjuvant radiotherapy. Median follow-up was 14 (7-29) months. At 6 months, the anastomosis had healed in 16 (53%) patients. At last follow-up, anastomotic integrity was found in 21 (70%) and continuity was restored in 20 (67%) patients. Non-healing at 12 months was observed in 10/29 (34%) patients overall, and in 3/14 (21%) when therapy started within three weeks following the index operation. Major LARS was reported in 12/15 (80%) patients. The direct medical costs were €8933 (95% CI 7268-10,707) per patient.
Conclusion: Vacuum-assisted early transanal closure of a leaking anastomosis after total mesorectal excision with 73% preoperative radiotherapy showed that acceptable anastomotic healing rates and stoma reversal rates can be achieved. Early diagnosis and start of treatment seems crucial.
Keywords: Anastomotic leakage; Rectal cancer; Transanal closure; Vacuum therapy.
Conflict of interest statement
W.A.A. Borstlap, G.D. Musters, L.P.S. Stassen, H.L. van Westreenen, D. Hess, S. van Dieren, S. Festen, E.J. van der Zaag, P.J. Tanis and W.A. Bemelman have no conflicts of interest or financial ties to disclose.
Figures

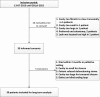


References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

