Predicting outcomes of gastric endoscopic submucosal dissection using a Bayesian approach: a step for individualized risk assessment
- PMID: 28670612
- PMCID: PMC5482747
- DOI: 10.1055/s-0043-106576
Predicting outcomes of gastric endoscopic submucosal dissection using a Bayesian approach: a step for individualized risk assessment
Abstract
Background and study aims: Efficacy and adverse events probabilities influence decisions regarding the best options to manage patients with gastric superficial lesions. We aimed at developing a Bayesian model to individualize the prediction of outcomes after gastric endoscopic submucosal dissection (ESD).
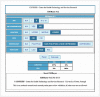
Patients and methods: Data from 245 gastric ESD were collected, including patient and lesion factors. The two endpoints were curative resection and post-procedural bleeding (PPB). Logistic regression and Bayesian networks were built for each outcome; their predictive value was evaluated in-sample and validated through leave-one-out and cross-validation. Clinical decision support was enhanced by the definition of risk matrices, direct use of Bayesian inference software and by a developed online platform.
Results: ESD was curative in 85.3 % and PPB occurred in 7.7 % of patients. In univariate analysis, male sex, ASA status, carcinoma histology, polypoid or depressed morphology, and lesion size ≥ 20 mm were associated with non-curative resection, while ASA status, antithrombotics and lesion size ≥ 20 mm were associated with PPB. Naïve Bayesian models presented AUROCs of ~80 % in the derivation cohort and ≥ 74 % in cross-validation for both outcomes. Risk matrices were computed, showing that lesions with cancer at biopsies, ≥ 20 mm, proximal or in the middle third, and polypoid are more prone to non-curative resection. PPB risk was < 5 % in lesions < 20 mm in the absence of antithrombotics.
Conclusions: The derived Bayesian model presented good discriminative power in the prediction of ESD outcomes and can be used to predict individualized probabilities, improving patient information and supporting clinical and management decisions.
Conflict of interest statement
Figures




Similar articles
-
Prediction model for non-curative resection of endoscopic submucosal dissection in patients with early gastric cancer.Gastrointest Endosc. 2017 May;85(5):976-983. doi: 10.1016/j.gie.2016.10.018. Epub 2016 Oct 15. Gastrointest Endosc. 2017. PMID: 27756614
-
AGA Institute Clinical Practice Update: Endoscopic Submucosal Dissection in the United States.Clin Gastroenterol Hepatol. 2019 Jan;17(1):16-25.e1. doi: 10.1016/j.cgh.2018.07.041. Epub 2018 Aug 2. Clin Gastroenterol Hepatol. 2019. PMID: 30077787 Review.
-
Prediction model for curative endoscopic submucosal dissection of undifferentiated-type early gastric cancer.Surg Endosc. 2022 Feb;36(2):1414-1423. doi: 10.1007/s00464-021-08426-w. Epub 2021 Mar 16. Surg Endosc. 2022. PMID: 33725190
-
Long-Term Outcomes of Gastric Endoscopic Submucosal Dissection: Focus on Metachronous and Non-Curative Resection Management.GE Port J Gastroenterol. 2017 Jan;24(1):31-39. doi: 10.1159/000450874. Epub 2016 Nov 30. GE Port J Gastroenterol. 2017. PMID: 28868336 Free PMC article.
-
Efficacy and safety of endoscopic submucosal dissection versus endoscopic mucosal resection for superficial esophageal carcinoma: a systematic review and meta-analysis.Dis Esophagus. 2021 Apr 7;34(4):doaa081. doi: 10.1093/dote/doaa081. Dis Esophagus. 2021. PMID: 32895709
Cited by
-
Machine Learning Improves the Prediction Rate of Non-Curative Resection of Endoscopic Submucosal Dissection in Patients with Early Gastric Cancer.Cancers (Basel). 2022 Jul 31;14(15):3742. doi: 10.3390/cancers14153742. Cancers (Basel). 2022. PMID: 35954406 Free PMC article.
-
Improving the Diagnosis and Treatment of Early Gastric Cancer in the West.GE Port J Gastroenterol. 2021 Dec 7;29(5):299-310. doi: 10.1159/000520529. eCollection 2022 Sep. GE Port J Gastroenterol. 2021. PMID: 36159192 Free PMC article. Review.
-
Risk-Scoring System for Prediction of Non-Curative Endoscopic Submucosal Dissection Requiring Additional Gastrectomy in Patients with Early Gastric Cancer.J Gastric Cancer. 2021 Dec;21(4):368-378. doi: 10.5230/jgc.2021.21.e33. Epub 2021 Nov 26. J Gastric Cancer. 2021. PMID: 35079439 Free PMC article.
-
Comprehensive review of Bayesian network applications in gastrointestinal cancers.World J Clin Oncol. 2025 Jun 24;16(6):104299. doi: 10.5306/wjco.v16.i6.104299. World J Clin Oncol. 2025. PMID: 40585838 Free PMC article. Review.
-
Should we recommend use of non-extension sign in Europe?Endosc Int Open. 2019 Jul;7(7):E883-E884. doi: 10.1055/a-0889-7987. Epub 2019 Jul 3. Endosc Int Open. 2019. PMID: 31288263 Free PMC article. No abstract available.
References
-
- Pimentel-Nunes P, Dinis-Ribeiro M, Ponchon T et al.Endoscopic submucosal dissection: European Society of Gastrointestinal Endoscopy (ESGE) Guideline. Endoscopy. 2015;47:829–854. - PubMed
-
- Lian J, Chen S, Zhang Y et al.A meta-analysis of endoscopic submucosal dissection and EMR for early gastric cancer. Gastrointestinal endoscopy. 2012;76:763–770. - PubMed
-
- Park Y M, Cho E, Kang H Y et al.The effectiveness and safety of endoscopic submucosal dissection compared with endoscopic mucosal resection for early gastric cancer: a systematic review and metaanalysis. Surgical endoscopy. 2011;25:2666–2677. - PubMed
-
- Pimentel-Nunes P, Mourao F, Veloso N et al.Long-term follow-up after endoscopic resection of gastric superficial neoplastic lesions in Portugal. Endoscopy. 2014;46:933–940. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

