Haploidentical allograft is superior to matched sibling donor allograft in eradicating pre-transplantation minimal residual disease of AML patients as determined by multiparameter flow cytometry: a retrospective and prospective analysis
- PMID: 28676064
- PMCID: PMC5496245
- DOI: 10.1186/s13045-017-0502-3
Haploidentical allograft is superior to matched sibling donor allograft in eradicating pre-transplantation minimal residual disease of AML patients as determined by multiparameter flow cytometry: a retrospective and prospective analysis
Abstract
Background: This study compared the effects of pre-transplantation minimal residual disease (pre-MRD) on outcomes in AML patients who underwent human leukocyte antigen-matched sibling donor transplantation (MSDT) or who received unmanipulated haploidentical allografts.
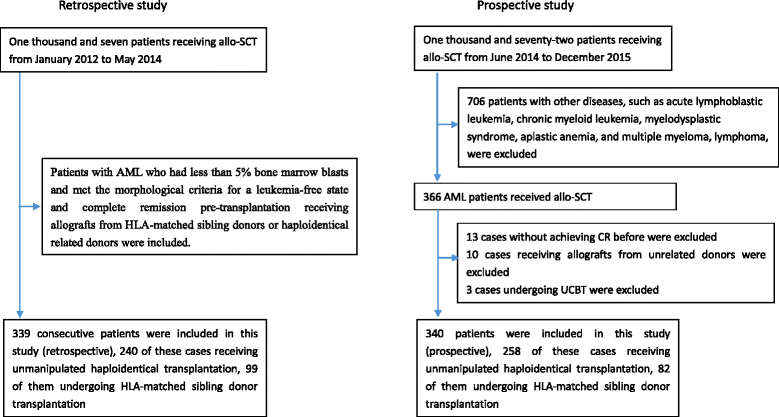
Methods: A retrospective study (n = 339) and a prospective study (n = 340) were performed. MRD was determined using multiparameter flow cytometry.
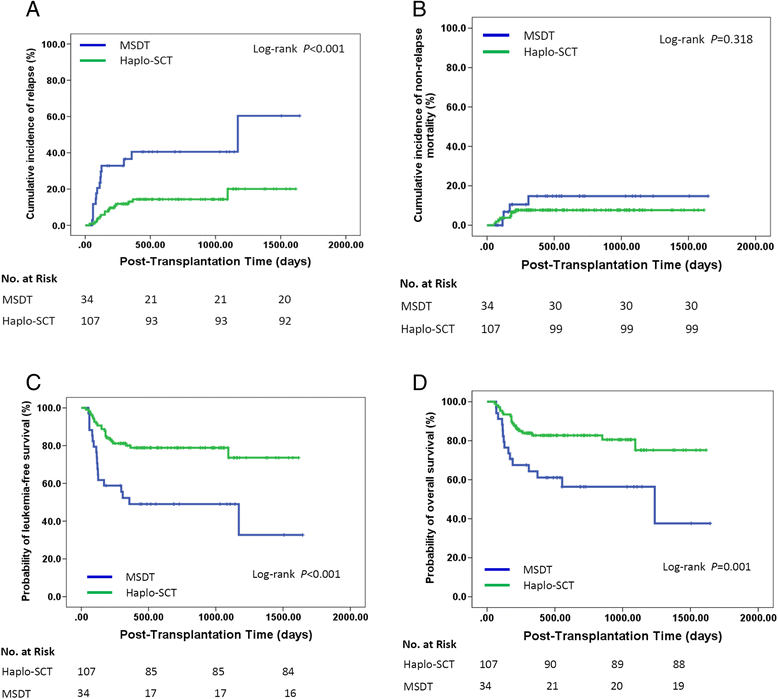
Results: Either after retrospective or prospective analysis, patients with negative pre-MRD (pre-MRDneg) had a lower incidence of relapse than those with positive pre-MRD (pre-MRDpos) in MSDT settings (P < 0.001 for all), but relapse was comparable in Haplo-SCT settings for patients with pre-MRDneg versus pre-MRDpos (P = 0.866 and 0.161, respectively). In either the retrospective (n = 65) or the prospective study (n = 76), pre-MRDpos subjects receiving Haplo-SCT experienced a lower incidence of relapse than those who underwent MSDT (P < 0.001 and p = 0.017, respectively). Of the patients with pre-MRDpos in either the total (n = 141) or the subgroup excluding cases which received donor lymphocyte infusion (DLI; n = 105), those who underwent MSDT had a higher incidence of relapse than those receiving haplo-SCT (P < 0.01 for all). Multivariate analysis showed that, for pre-MRDpos cases, haplo-SCT was associated with a low incidence of relapse and with better LFS and OS in either retrospective group, prospective group, combination groups, or subgroup not including cases which received DLI.
Conclusions: The results indicated that, for pre-MRD-positive AML patients, haplo-SCT was associated with lower incidence of relapse and better survival, suggesting a stronger anti-leukemia effect.
Keywords: Acute myeloid leukemia; Allogeneic stem cell transplantation; Minimal residual disease; Multiparameter flow cytometry; Unmanipulated haploidentical allografts.
Conflict of interest statement
Ethics approval and consent to participate
All of the included subjects provided written informed consent. The study was conducted in accordance with the Declaration of Helsinki and was approved by the Institutional Review Board of Peking University.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
-
- Walker I, Panzarella T, Couban S, et al. Pretreatment with anti-thymocyte globulin versus no anti-thymocyte globulin in patients with haematological malignancies undergoing haemopoietic cell transplantation from unrelated donors: a randomised, controlled, open-label, phase 3, multicentre trial. Lancet Oncol. 2016;17(2):164–173. doi: 10.1016/S1470-2045(15)00462-3. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

