Longitudinal immunological characterization of the first presensitized recipient of a face transplant
- PMID: 28679959
- PMCID: PMC5499367
- DOI: 10.1172/jci.insight.93894
Longitudinal immunological characterization of the first presensitized recipient of a face transplant
Abstract
Rejection affects greater than 80% of face transplants, yet no diagnostic criteria for antibody-mediated rejection (AMR) following face transplantation have been established. Given that different treatment strategies are required to address AMR and T cell-mediated rejection (TCMR), there is a critical need to delineate the features that can differentiate these two alloimmune responses. Here, we report the longitudinal immunological examination of what we believe to be the first and only highly sensitized recipient of a crossmatch-positive face transplant up to 4 years following transplantation. We conducted gene expression profiling on allograft biopsies collected during suspected AMR and TCMR episodes as well as during 5 nonrejection time points. Our data suggest that there are distinctive molecular features in AMR, characterized by overexpression of endothelial-associated genes, including ICAM1, VCAM1, and SELE. Although our findings are limited to a single patient, these findings highlight the potential importance of developing and implementing molecular markers to differentiate AMR from TCMR to guide clinical management. Furthermore, our case illustrates that molecular assessment of allograft biopsies offers the potential for new insights into the mechanisms underlying rejection. Finally, our medium-term outcomes demonstrate that face transplantation in a highly sensitized patient with a positive preoperative crossmatch is feasible and manageable.
Keywords: Immunology; Transplantation.
Conflict of interest statement
Figures
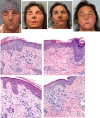
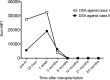
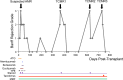



Similar articles
-
Investigation of Serum Angiotensin II Type 1 Receptor Antibodies at the Time of Renal Allograft Rejection.Ann Lab Med. 2015 May;35(3):314-20. doi: 10.3343/alm.2015.35.3.314. Epub 2015 Apr 1. Ann Lab Med. 2015. PMID: 25932439 Free PMC article.
-
Clinical and Pathological Features of Plasma Cell-Rich Acute Rejection After Kidney Transplantation.Transplantation. 2018 May;102(5):853-859. doi: 10.1097/TP.0000000000002041. Transplantation. 2018. PMID: 29319615
-
Gene Expression Profiling for the Identification and Classification of Antibody-Mediated Heart Rejection.Circulation. 2017 Mar 7;135(10):917-935. doi: 10.1161/CIRCULATIONAHA.116.022907. Epub 2017 Feb 1. Circulation. 2017. PMID: 28148598
-
ABO-compatible liver allograft antibody-mediated rejection: an update.Curr Opin Organ Transplant. 2015 Jun;20(3):314-24. doi: 10.1097/MOT.0000000000000194. Curr Opin Organ Transplant. 2015. PMID: 25944231 Free PMC article. Review.
-
Distinctive morphological features of antibody-mediated and T-cell-mediated acute rejection in pancreas allograft biopsies.Curr Opin Organ Transplant. 2012 Feb;17(1):93-9. doi: 10.1097/MOT.0b013e32834ee754. Curr Opin Organ Transplant. 2012. PMID: 22227719 Review.
Cited by
-
The role of C4d and donor specific antibodies in face and hand transplantation-a systematic review.Front Transplant. 2024 Sep 3;3:1442006. doi: 10.3389/frtra.2024.1442006. eCollection 2024. Front Transplant. 2024. PMID: 39291278 Free PMC article.
-
Tacrolimus-loaded Drug Delivery Systems in Vascularized Composite Allotransplantation: Lessons and Opportunities for Local Immunosuppression.Transplantation. 2025 Jan 1;109(1):142-152. doi: 10.1097/TP.0000000000005049. Epub 2024 May 21. Transplantation. 2025. PMID: 38773862 Free PMC article. Review.
-
Sex and Gender Differences in Face and Upper Extremity Allotransplantation: A Narrative Review of Implications and Impact.Cureus. 2025 Jan 24;17(1):e77938. doi: 10.7759/cureus.77938. eCollection 2025 Jan. Cureus. 2025. PMID: 39996233 Free PMC article. Review.
-
Cellular activation pathways and interaction networks in vascularized composite allotransplantation.Front Immunol. 2023 May 17;14:1179355. doi: 10.3389/fimmu.2023.1179355. eCollection 2023. Front Immunol. 2023. PMID: 37266446 Free PMC article. Review.
-
Trends, Gaps, and Collaboration in Facial Transplantation: A Bibliometric Study.Plast Reconstr Surg Glob Open. 2022 Apr 15;10(4):e4248. doi: 10.1097/GOX.0000000000004248. eCollection 2022 Apr. Plast Reconstr Surg Glob Open. 2022. PMID: 37073383 Free PMC article.
References
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

