Epidemiology and antifungal susceptibility of Candida species in a tertiary care hospital, Kolkata, India
- PMID: 28681016
- PMCID: PMC5490301
- DOI: 10.18869/acadpub.cmm.2.2.5
Epidemiology and antifungal susceptibility of Candida species in a tertiary care hospital, Kolkata, India
Abstract
Background and purpose: The incidence of fungal infection as well as candidemia has increased significantly, contributing to morbidity and mortality in the developed countries. The alarming increase in infections with multidrug resistant bacteria is due to overuse of a broad spectrum antimicrobials, which leads to over growth of Candida spp.; thus, enhancing its opportunity to cause the disease. A shift has been observed in the relative frequency of each Candida spp. Antifungal agents available for the treatment of systemic and invasive candidiasis are restricted to polyenes, allylamines, azoles, and the recent echinocandin class of molecules. In the past few decades, the incidence of resistance to antifungal treatment of Candida spp. has increased rapidly, which is of serious concern for healthcare professionals. Studies on prevalence of infections and antifungal susceptibility testing can help with deciding on clinical strategies to manage this problem. Herein, we aimed to identify the epidemiology of Candida spp. among blood culture isolates and to investigate the susceptibility pattern of these species to antifungal agents.
Materials and methods: Candida spp. were isolated from blood cultures from 70 patients in a tertiary care hospital, Kolkata, India. The growth of Candida spp. on sabouraud dextrose agar was confirmed by Gram staining, where gram-positive budding fungal cells were observed. The species identification as well as antifungal susceptibility testing were performed with VITEK 2 compact automated system using VITEK-2 cards for identification of yeast and yeast-like organisms) ID-YST card). Antifungal susceptibility testing was carried out with VITEK 2 fungal susceptibility card (AST-YS07 kit).
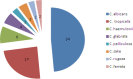
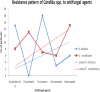
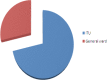
Results: Out of 70 samples, Candidaalbicans were isolated from 34 (%48.57) samples. The remaining 36 (%51.43) were non-albicans Candida ) NAC). Out of 34 C.Albicans, antifungal susceptiblity was detected in 28 isolates, all of which were sensitive to fluconazole (FLC .( Resistance to amphotericine B) AMP), flucytosine (5FC), voriconazole (VRC), and itraconazole (ITC) was observed in, %44.12 , %52.94 , %8.82 and %17.65 of the cases, respectively. For other Candida spp. (other than C.Albicans ,( antifungal susceptibility was evaluated for 36 isolates, among which resistance to AMP, FLC , 5FC, VRC , and ITC was found in, %30.56 , %61.11 , %33.33 , %19.44 and %38.89 cases, respectively.
Conclusion: Species-level identification of Candida and their antifungal sensitivity testing should to be performed to achieve better clinical result and to select an appropriate and effective antifungal therapy. High resistance to antifungal agents is an alarming sign to the healthcare professionals.
Keywords: Candida albicans; Fluconazole; Itraconazole; Non-albicans Candida; Voriconazol.
Conflict of interest statement
None declared.
Figures
Similar articles
-
Candida and candidaemia. Susceptibility and epidemiology.Dan Med J. 2013 Nov;60(11):B4698. Dan Med J. 2013. PMID: 24192246 Review.
-
Species distribution and drug susceptibility of candida in clinical isolates from a tertiary care centre at Indore.Indian J Med Microbiol. 2014 Jan-Mar;32(1):44-8. doi: 10.4103/0255-0857.124300. Indian J Med Microbiol. 2014. PMID: 24399387
-
Spectrum of candidal species isolated from neonates admitted in an Intensive Care Unit of teaching hospital of Kashmir, North India.J Lab Physicians. 2018 Jul-Sep;10(3):255-259. doi: 10.4103/JLP.JLP_1_18. J Lab Physicians. 2018. PMID: 30078958 Free PMC article.
-
Iranian HIV/AIDS patients with oropharyngeal candidiasis: identification, prevalence and antifungal susceptibility of Candida species.Lett Appl Microbiol. 2018 Oct;67(4):392-399. doi: 10.1111/lam.13052. Epub 2018 Aug 16. Lett Appl Microbiol. 2018. PMID: 30019443
-
Resistance in human pathogenic yeasts and filamentous fungi: prevalence, underlying molecular mechanisms and link to the use of antifungals in humans and the environment.Dan Med J. 2016 Oct;63(10):B5288. Dan Med J. 2016. PMID: 27697142 Review.
Cited by
-
A New Variant of Mutational and Polymorphic Signatures in the ERG11 Gene of Fluconazole-Resistant Candida albicans.Infect Drug Resist. 2022 Jun 17;15:3111-3133. doi: 10.2147/IDR.S360973. eCollection 2022. Infect Drug Resist. 2022. PMID: 35747333 Free PMC article.
-
Isolation and identification of Candida species from catheter-associated urinary tract infection in Thamar city hospitals, Yemen.Int Microbiol. 2025 Apr;28(4):739-749. doi: 10.1007/s10123-024-00578-8. Epub 2024 Aug 19. Int Microbiol. 2025. PMID: 39158667
-
Time-to-Positivity for Candida in Bloodstream Infections: Prognostic Implications for Mortality.Cureus. 2024 Aug 7;16(8):e66364. doi: 10.7759/cureus.66364. eCollection 2024 Aug. Cureus. 2024. PMID: 39246854 Free PMC article.
-
Prevalence and antifungal drug resistance of nosocomial Candida species isolated from two university hospitals in Egypt.Curr Med Mycol. 2021 Mar;7(1):31-37. doi: 10.18502/cmm.7.1.6181. Curr Med Mycol. 2021. PMID: 34553095 Free PMC article.
-
Wickerhamomyces anomalous: A Rare Cause of Fungemia Causing Febrile Neutropenia in Acute Lymphoblastic Leukemia.Case Rep Infect Dis. 2020 Dec 29;2020:8847853. doi: 10.1155/2020/8847853. eCollection 2020. Case Rep Infect Dis. 2020. PMID: 33457028 Free PMC article.
References
-
- Richardson M, Lass-Flörl C. Changing epidemiology of systemic fungal infections. Clin Microbial Infect. 2008;14(Suppl 4):5–24. - PubMed
-
- Wisplinghoff H, Bischoff T, Tallent SM, Seifert H, Wenzel RP, Edmond MB. Nosocomial bloodstream infections in US hospitals: analysis of 24,179 cases from a prospective nationwide surveillance study. Clin Infect Dis. 2004;39(3):309–17. - PubMed
-
- Marchetti O, Bille J, Fluckiger U, Eggimann P, Ruef C, Garbino J, et al. Epidemiology of candidaemia in Swiss tertiary care hospitals: secular trends, 1991-2000. Clin Infect Dis. 2004;38(3):311–20. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous