Functional and morphological evolution of remnant pancreas after resection for pancreatic adenocarcinoma
- PMID: 28700497
- PMCID: PMC5515769
- DOI: 10.1097/MD.0000000000007495
Functional and morphological evolution of remnant pancreas after resection for pancreatic adenocarcinoma
Abstract
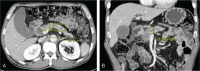
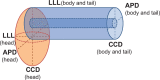
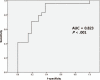
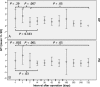
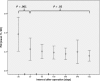
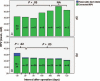
Functional and morphological evolution of remnant pancreas after resection for pancreatic adenocarcinoma is investigated.The medical records of 45 patients who had undergone radical resection for pancreatic adenocarcinoma from March 2010 to September 2013 were reviewed retrospectively. There were 34 patients in the pancreaticoduodenectomy (PD) group and 10 patients in the distal pancreatectomy (DP) group. One patient received total pancreatectomy. The endocrine function was measured using the glucose tolerance index (GTI), which was derived by dividing daily maximum serum glucose fluctuation by daily minimum glucose. Remnant pancreas volume (RPV) was estimated by considering pancreas body and tail as a column, and head as an ellipsoid, respectively. The pancreatic atrophic index (PAI) was defined as the ratio of pancreatic duct width to total pancreas width. Representative indices of each patient were compared before and after resection up to 2 years postoperatively.The area under receiver operating characteristic curve of GTI for diagnosing DM was 0.823 (95% confidence interval, 0.699-0.948, P < .001). Overall, GTI increased on postoperative day 1 (POD#1, mean ± standard deviation, 1.79 ± 1.40 vs preoperative, 1.02 ± 1.41; P = .001), and then decreased by day 7 (0.89 ± 1.16 vs POD#1, P < .001). In the PD group, the GTI on POD#14 became lower than preoperative (0.51 ± 0.38 vs 0.96 ± 1.37; P = .03). PAI in the PD group was significantly lower at 1 month postoperatively (0.22 ± 0.12 vs preoperative, 0.38 ± 0.18; P < .001). In the PD group, RPV was significantly lower at 1 month postoperatively (25.3 ± 18.3 cm vs preoperative, 32.4 ± 20.1 cm; P = .02), due to the resolution of pancreatic duct dilatation. RPV of the DP group showed no significant change. GTI was negatively related to RPV preoperatively (r = -0.317, P = .04), but this correlation disappeared postoperatively (r = -0.044, P = .62).Pancreatic endocrine functional deterioration in pancreatic adenocarcinoma patients may in part be due to pancreatic duct obstruction and dilatation caused by the tumor. After resection, this proportion of endocrine insufficiency is corrected.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures

Similar articles
-
Endocrine Function Impairment After Distal Pancreatectomy: Incidence and Related Factors.World J Surg. 2016 Feb;40(2):440-6. doi: 10.1007/s00268-015-3228-9. World J Surg. 2016. PMID: 26330237
-
Central Pancreatectomy Versus Distal Pancreatectomy and Pancreaticoduodenectomy for Benign and Low-Grade Malignant Neoplasms: A Retrospective and Propensity Score-Matched Study with Long-Term Functional Outcomes and Pancreas Volumetry.Ann Surg Oncol. 2020 Apr;27(4):1215-1224. doi: 10.1245/s10434-019-08095-z. Epub 2020 Jan 2. Ann Surg Oncol. 2020. PMID: 31898101
-
Three-dimensional remnant pancreatic volume ratio indicates postoperative pancreatic exocrine insufficiency in pancreatic cancer patients after distal pancreatectomy.Pancreatology. 2020 Jul;20(5):867-874. doi: 10.1016/j.pan.2020.06.018. Epub 2020 Jul 4. Pancreatology. 2020. PMID: 32654989
-
[Anatomy of the head of the pancreas and various limited resection procedures for intraductal papillary-mucinous tumors of the pancreas].Nihon Geka Gakkai Zasshi. 2003 Jun;104(6):460-70. Nihon Geka Gakkai Zasshi. 2003. PMID: 12854493 Review. Japanese.
-
Resection of the duodenum causes long-term endocrine and exocrine dysfunction after Whipple procedure for benign tumors - Results of a systematic review and meta-analysis.HPB (Oxford). 2020 Jun;22(6):809-820. doi: 10.1016/j.hpb.2019.12.016. Epub 2020 Jan 23. HPB (Oxford). 2020. PMID: 31983660
Cited by
-
Relationship between imaging changes of the pancreas and islet beta-cell function.World J Radiol. 2024 Dec 28;16(12):717-721. doi: 10.4329/wjr.v16.i12.717. World J Radiol. 2024. PMID: 39801662 Free PMC article.
-
Investigation of the influence of pancreatic surgery on new-onset and persistent diabetes mellitus.Ann Gastroenterol Surg. 2021 Feb 1;5(4):575-584. doi: 10.1002/ags3.12435. eCollection 2021 Jul. Ann Gastroenterol Surg. 2021. PMID: 34337306 Free PMC article.
-
The impact of postoperative exocrine index on non-alcoholic fatty liver disease following pancreaticoduodenectomy.Ann Gastroenterol Surg. 2022 Apr 25;6(5):704-711. doi: 10.1002/ags3.12572. eCollection 2022 Sep. Ann Gastroenterol Surg. 2022. PMID: 36091315 Free PMC article.
References
-
- Orr RK. Outcomes in pancreatic cancer surgery. Surg Clin North Am 2010;90:219–34. - PubMed
-
- Slezak LA, Andersen DK. Pancreatic resection: effects on glucose metabolism. World J Surg 2001;25:452–60. - PubMed
-
- Hüttner FJ, Koessler-Ebs J, Hackert T, et al. Meta-analysis of surgical outcome after enucleation versus standard resection for pancreatic neoplasms. Br J Surg 2015;102:1026–36. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

