A critical comparison of techniques for MRI-targeted biopsy of the prostate
- PMID: 28725585
- PMCID: PMC5503959
- DOI: 10.21037/tau.2017.03.77
A critical comparison of techniques for MRI-targeted biopsy of the prostate
Abstract
MRI-targeted biopsy is a promising technique that offers an improved detection of clinically significant prostate cancer over standard non-targeted biopsy. It is established that prostate MRI is of use in both the primary and repeat biopsy setting for the detection of significant prostate cancer. There are three approaches to targeting biopsies to areas of interest seen on prostate MRI. They each rely on the acquisition and reporting of a diagnostic quality multi-parametric MRI scan used to identify areas of interest, and the subsequent use of those diagnostic quality images in combination with real-time images of the prostate during the biopsy procedure. The three techniques are: visual registration of the MRI images with a real-time ultrasound image; software-assisted fusion of the MRI images and the real-time ultrasound images, and in-bore biopsy, which requires registration of a diagnostic quality MRI scan with a real time interventional MRI image. In this paper we compare the three techniques and evaluate those studies where there is a direct comparison of more than one MRI-targeting technique. PubMed was searched from inception to November 2016 using the search terms (cognitive registration OR visual registration OR fusion biopsy OR in-bore biopsy OR targeted biopsy) AND (prostate cancer OR prostate adenocarcinoma OR prostate carcinoma OR prostatic carcinoma OR prostatic adenocarcinoma) AND (MRI OR NMR OR magnetic resonance imaging OR mpMRI OR multiparametric MRI). The initial search included 731 abstracts. Eleven full text papers directly compared two or more techniques of MRI-targeting, and were selected for inclusion. The detection of clinically significant prostate cancer varied from 0% to 93.3% for visual registration, 23.2% to 100% for software-assisted registration and 29% to 80% for in-bore biopsy. Detection rates for clinically significant cancer are dependent on the prevalence of cancer within the population biopsied, which in turn is determined by the selection criteria [biopsy naïve, previous negative biopsy, prostate specific antigen (PSA) selection criteria, presence of a lesion on MRI]. Cancer detection rates varied more between study populations than between biopsy approaches. Currently there is no consensus on which type of MRI-targeted biopsy performs better in a given setting. Although there have been studies supporting each of the three techniques, substantial differences in methodology and reporting the findings make it difficult to reliably compare their outcomes.
Keywords: Image-guided biopsy; magnetic resonance imaging; prostate; prostatic neoplasms.
Conflict of interest statement
Conflicts of Interest: The authors have no conflicts of interest to declare.
Figures
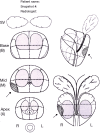
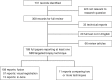
References
-
- Hodge KK, McNeal JE, Terris MK, et al. Random systematic versus directed ultrasound guided transrectal core biopsies of the prostate. J Urol 1989;142:71-4; discussion 74-5. - PubMed
-
- European Association of Urology. Guidelines on Prostate Cancer. 2013. Available online: https://uroweb.org/wp-content/uploads/1607-Prostate-Cancer_LRV3.pdf
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous
