Multicenter study of pars plana vitrectomy for optic disc pit maculopathy: MACPIT study
- PMID: 28731058
- PMCID: PMC5601440
- DOI: 10.1038/eye.2017.142
Multicenter study of pars plana vitrectomy for optic disc pit maculopathy: MACPIT study
Abstract
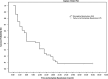
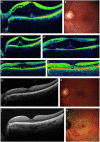
PurposeTo evaluate surgical intervention with pars plana vitrectomy (PPV) for correction of optic disc pit maculopathy (ODP-M).Patients and methodsRetrospective chart review from 13 centres of 51 eyes of 50 patients with ODP-M who underwent PPV between 2002-2014. Anatomic and final best-corrected visual acuity (BCVA) outcomes were evaluated for all cases with different adjuvant techniques.ResultsThere were 23 males and 27 females with median age 25.5 (6-68) years. Preoperative median foveal thickness was 694.5 (331-1384) μm and improved to 252.5 (153-1405) μm. Median BCVA improved from 20/200 (20/20000 to 20/40) to 20/40 (20/2000 to 20/20) with 20/40 or better in 31 eyes. Complete retinal reattachment was achieved in 44 eyes (86.3%) at 7.1 (5.9) months. The good surgical outcomes were achieved in different adjuvant groups. Median follow-up was 24 (6 to 120) months.ConclusionsThese results confirm the long-term effectiveness of PPV for ODP-M. Prospective studies are needed to determine the effectiveness of any adjuvant technique in improving the success of PPV for ODP-M.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
Comment in
-
Optic disc pit maculopathy.Eye (Lond). 2018 Aug;32(8):1419-1420. doi: 10.1038/s41433-018-0091-6. Epub 2018 Apr 13. Eye (Lond). 2018. PMID: 29666483 Free PMC article. No abstract available.
References
-
- Apple DJ, Rabb MF, Walsh PM. Congenital anomalies of the optic disc. Surv Ophthalmol 1998; 27: 3–41. - PubMed
-
- Gass JDM. Serous detachment of the macula secondary to congenital pit of the optic nerve head. Am J Ophthalmol 1969; 67: 821–841. - PubMed
-
- Jain N, Johnson MW. Pathogenesis and treatment of maculopathy associated with cavitary optic disc anomalies. Am J Ophthalmol 2014; 158: 423–435. - PubMed
-
- Gowdar JP, Rajesh B, Giridhar A, Gopalakrishnan M, Hussain R, Thachil T. An insight into the pathogenesis of optic disc pit-associated maculopathy with enhanced depth imaging. JAMA Ophthalmol 2015; 133: 466–469. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

